COVID-19 primarily affects the respiratory system, yet many people have reported symptoms that extend beyond the lungs, including issues involving the mouth.
There’s still much to uncover about how COVID-19 relates to a range of signs and symptoms. Nonetheless, emerging research is beginning to explore links between SARS-CoV-2 and oral health.
Read on to learn more about possible associations between dental complaints and COVID-19.
COVID-19 signs in the mouth, teeth, and gums
SARS-CoV-2, the virus behind COVID-19, enters the bloodstream by binding to a receptor known as ACE2. Think of this receptor as the gateway the virus uses to invade cells.
And where are ACE2-rich cells plentiful? In the oral cavity—on the tongue and gums.
Individuals with poorer oral health often have increased expression of ACE2 receptors, which may help explain a connection between COVID-19 and oral conditions.
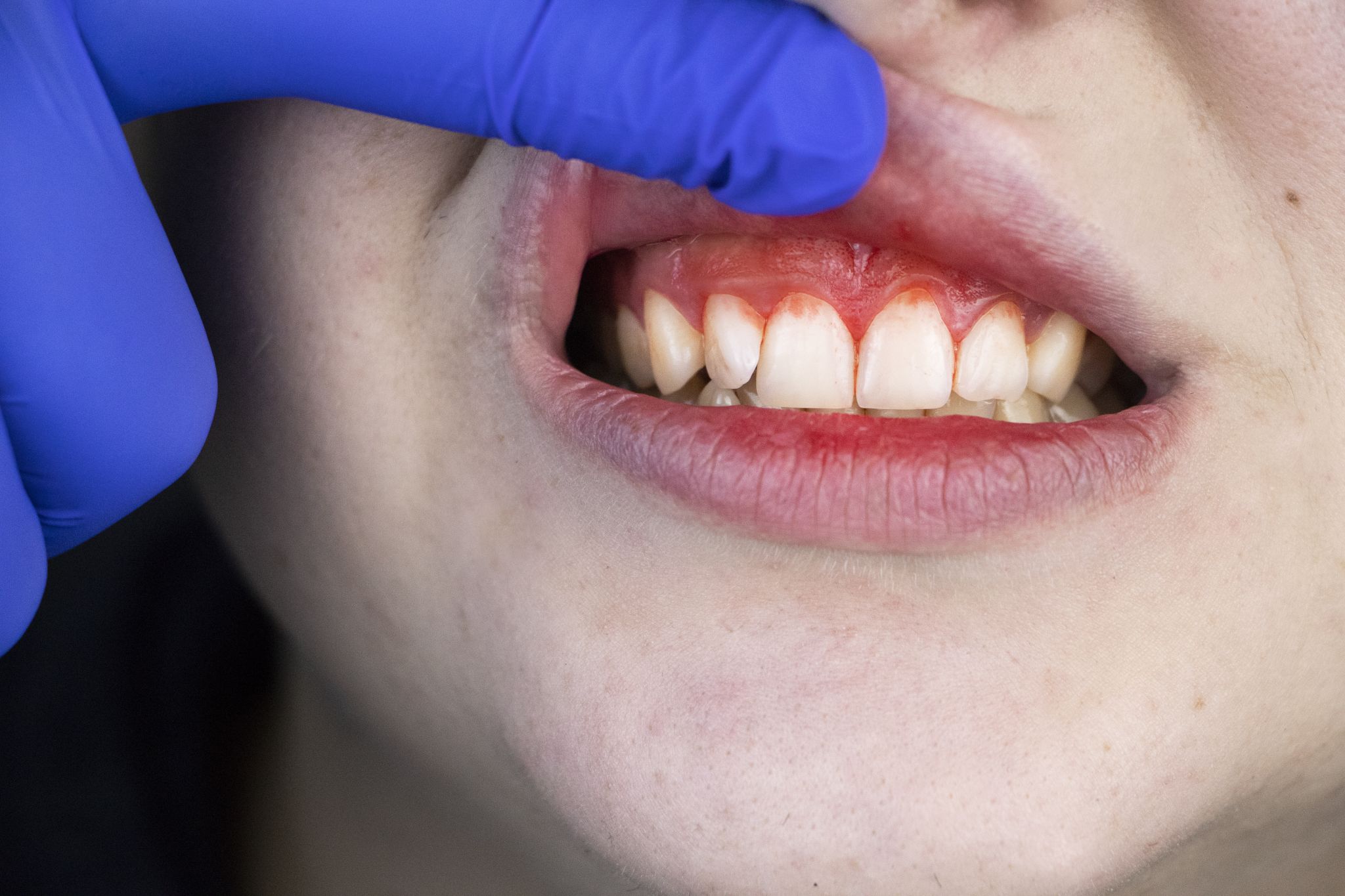
One study looked at the relationship between dental disease and COVID-19 outcomes. The researchers observed a notable association between the extent of dental disease and how severe COVID-19 became.
Approximately 75 percent of participants with advanced dental problems required hospitalization for COVID-19, whereas none of those without clear dental issues were hospitalized.
This could reflect that people with worse oral health frequently have other chronic conditions as well.
That said, there are relatively few studies indicating that COVID-19 directly causes poor dental health. Significant reports describing oral symptoms as a typical part of COVID-19 presentations are also limited.
In a systematic review covering 54 studies of COVID-19 signs and symptoms, tooth pain or mouth-related complaints did not rank among the top 12 reported symptoms. Fever (81.2 percent), cough (58.5 percent), and fatigue (38.5 percent) were the most frequently noted.
However, that doesn’t rule out experiencing dental symptoms during or after COVID-19. Like with many illnesses, people may neglect self-care, change their diet, or reduce attention to oral hygiene, which can cause indirect dental effects.
Treating dental pain during or after COVID-19
If you have tooth pain during an active COVID-19 infection or shortly afterward, 400 milligrams of ibuprofen can provide better relief for dental pain than acetaminophen for some people. Applying cool compresses (a soft cloth dampened with cool water) to the outside of the cheek can also ease discomfort.
Some patients develop oral infections, like oral thrush, while infected with COVID-19. If that occurs, a clinician may prescribe antifungal treatment.
It’s also possible the timing is coincidental: a cavity or infected tooth might flare up while you have COVID-19. If over-the-counter pain relievers don’t control the pain, contact your dentist for guidance.
Frequently asked questions
Dentists often link good oral care with overall health. A 2020 study suggests that maintaining excellent oral hygiene could lessen the severity of COVID-19 symptoms if one becomes infected.
Although research remains limited, here are some possible connections between oral health and COVID-19 to consider.
Can bleeding gums be a sign of COVID-19?
Bleeding gums are not commonly listed among COVID-19 symptoms, according to a review of studies. In contrast, altered blood clotting rather than bleeding has been observed as a COVID-19-related issue.
Still, bleeding gums can indicate gum disease and shouldn’t be ignored. Your dentist may advise postponing an in-office visit until you’re recovered, but seek advice about managing the problem.
Does COVID-19 cause mouth rashes?
Rashes are not a frequently reported manifestation of COVID-19.
In a case report that noted a widespread rash in a patient, authors pointed out only 2 of 1,099 COVID-19 cases reported any rash. A rash localized to the mouth is not commonly reported in the current literature, so it’s unlikely to be caused by COVID-19. If you have mouth sores or a rash, discuss other potential causes with your healthcare provider.
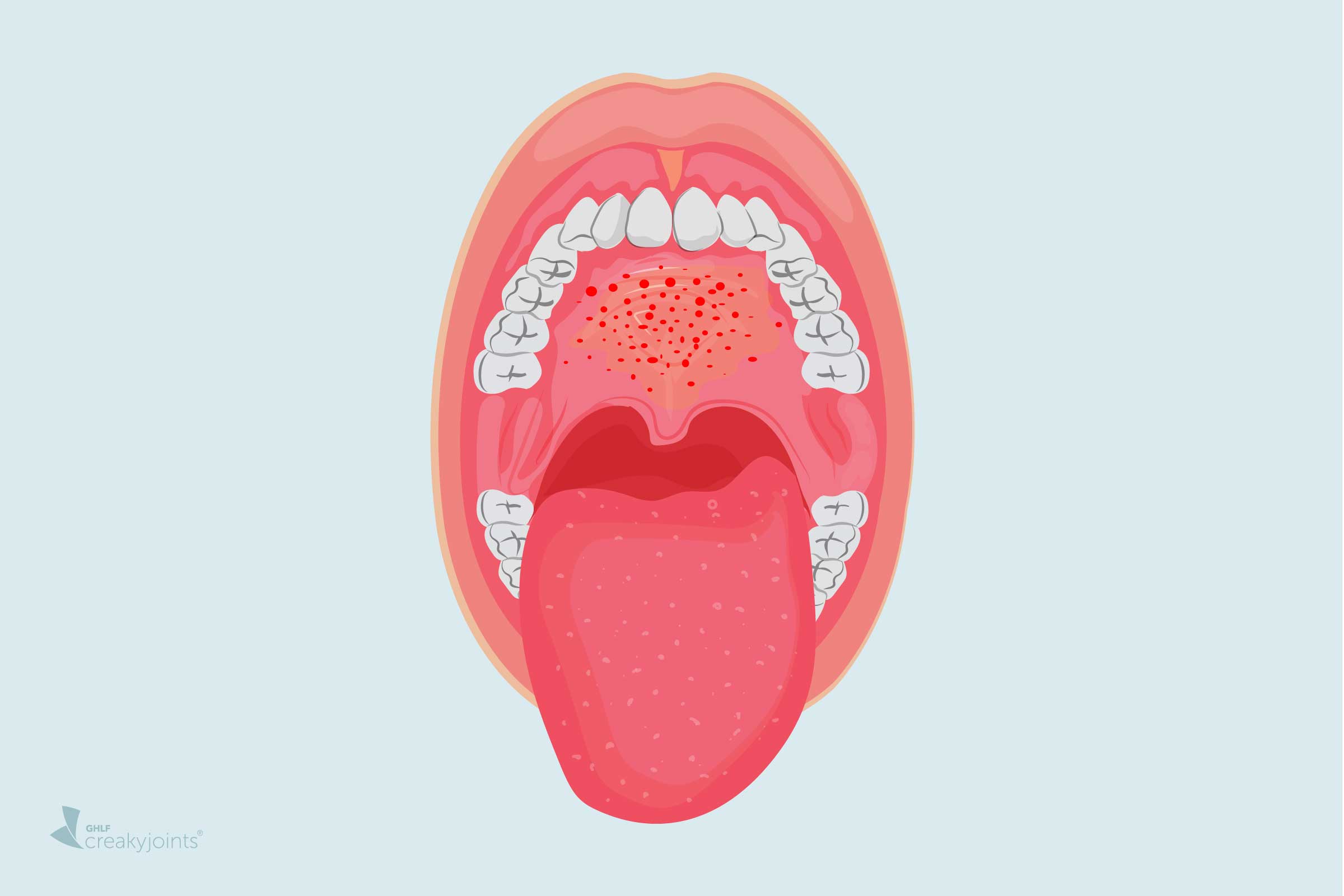
Is a white coating on the tongue linked to COVID-19?
A white film on the tongue can stem from various causes. Oral candidiasis (thrush) is one common cause.
While COVID-19 doesn’t directly cause thrush, SARS-CoV-2 can impact immune function, potentially leaving someone more susceptible to secondary infections such as thrush.
Besides white patches or coating on the tongue and throat, oral thrush may cause:
- cracked skin at the corners of the mouth
- painful eating
- reduced taste sensation
- difficulty swallowing
- sore tongue
A healthcare provider can prescribe topical or oral antifungal medications to treat the fungus that causes thrush.
Have dentists seen more teeth grinding since the pandemic started?
Bruxism, or teeth grinding, commonly increases with stress.
A 2020 review emphasized links between stress and awake bruxism (clenching while awake). Given the pandemic’s added stress for many, an uptick in this issue would not be surprising.
Potential complications of persistent grinding include:
- tooth wear
- heightened sensitivity to temperature
- jaw muscle soreness or pain
If bruxism is bothering you, consult your healthcare provider about management strategies.
Is it safe to visit the dentist during the COVID-19 pandemic?
Dental practices can implement measures to reduce COVID-19 transmission risk. Some methods they may use to protect patients include:
Ask your dentist which precautions they’re following to help keep you safe.
Why might teeth become yellow or discolored after COVID-19?
Tooth discoloration or yellowing is not a well-established direct effect of COVID-19.
However, some treatments prescribed during COVID-19 care have been reported to cause tooth staining. For instance, one antibiotic example is doxycycline, which can lead to yellowing or staining of teeth.
Antibiotics don’t treat the virus itself, but they may be used to treat bacterial complications (such as secondary pneumonia) associated with COVID-19.
If you need medication while recovering from COVID-19, discuss potential side effects like tooth staining with your clinician to weigh risks and benefits.
Can COVID-19 make your teeth fall out?
There are no reports indicating teeth falling out as a direct consequence of COVID-19.
If someone is ill for an extended period and neglects oral hygiene, this could accelerate decay and eventual tooth loss. Still, at present there is no proven direct link between SARS-CoV-2 infection and spontaneous tooth loss.
Can COVID-19 cause jaw or tooth pain?
You might experience jaw or dental pain from stress-related jaw clenching during the pandemic. However, jaw or tooth pain is not a hallmark symptom of COVID-19 itself.
Takeaway
Ongoing research will keep exploring connections between COVID-19 and oral health outcomes.
Because new variants may emerge, future strains could potentially influence dental health differently. If you notice dental concerns, contact your dentist to preserve your oral health.



















Leave a Reply
You must be logged in to post a comment.