Split hand is a clinical phenomenon in which muscles on one side of the hand become noticeably weaker than others. It is frequently associated with early amyotrophic lateral sclerosis (ALS), although a few other uncommon neurological disorders can also lead to a similar pattern.
Amyotrophic lateral sclerosis (ALS) is a progressive neurodegenerative disease that results in the gradual loss of voluntary muscle control, including the muscles required for breathing. Because early symptoms can be subtle, many people search for a Do I have ALS quiz when they first notice hand weakness or muscle twitching. While online tools may raise awareness, only a thorough medical evaluation can determine the true cause of symptoms.

One hallmark early feature of ALS is weakness in the hand muscles. The distribution of this weakness tends to follow a recognizable pattern, initially impacting certain muscles while sparing others.
This characteristic presentation, known as “split hand,” may point toward ALS. However, physicians cannot rely on this sign alone to establish a definitive ALS diagnosis. It must be interpreted alongside other neurological findings and diagnostic tests.
What is the split hand test?
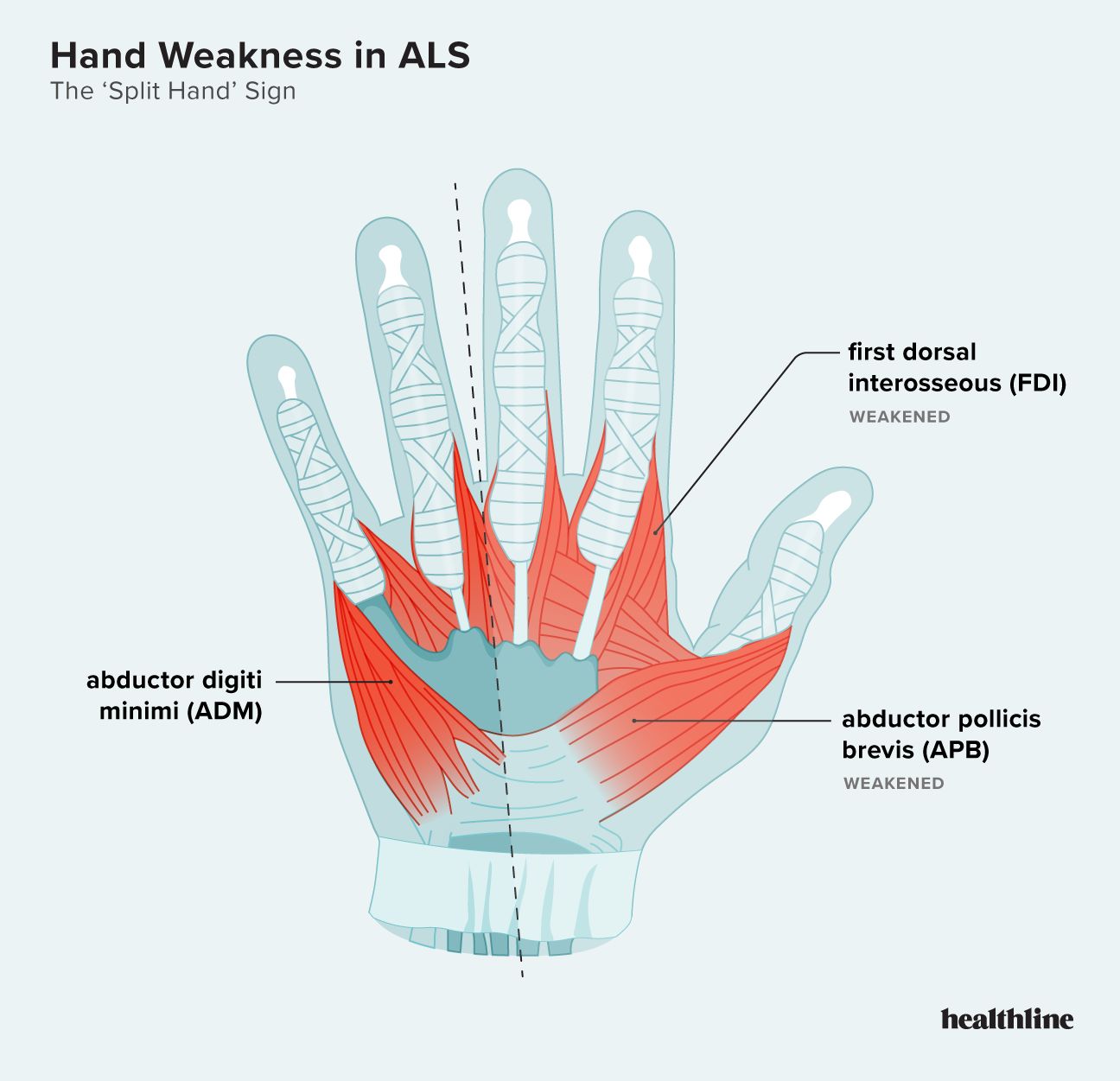
The split hand phenomenon describes a particular pattern of muscle atrophy that interferes with fine motor skills, such as pinching or bringing the thumb and index finger together.
This occurs because of wasting in the muscles at the base of the thumb — the abductor pollicis brevis (APB) — and in the muscle between the thumb and index finger, the first dorsal interosseous (FDI).
As these muscles shrink, the muscles near the little finger, especially the abductor digiti minimi (ADM) along the outer palm, typically remain preserved. This contrast in muscle involvement gives rise to the term “split hand.” As the condition advances, individuals may find themselves gripping objects primarily with the ring and little fingers due to reduced thumb strength and coordination.
In certain ALS cases, particularly bulbar onset ALS, both inner and outer hand muscles may eventually undergo atrophy. As the disease progresses, this broader muscle involvement can develop in any ALS subtype.
A neurologist can observe evidence of split hand using specialized nerve conduction testing. One commonly used method is the compound muscle action potential (CMAP) test, which evaluates electrical activity in specific hand muscles. By comparing signal strength between muscles, clinicians can identify which muscles show reduced nerve conduction and which remain relatively intact.
How does the split hand index help diagnose ALS?
To better quantify the imbalance in nerve conduction between affected and unaffected muscles, clinicians use specific calculations. The two key measurements include:
- Split hand ratio: This compares the CMAP values of APB/ADM or FDI/ADM to highlight relative weakness.
- Split hand index: This calculation multiplies the CMAP values of APB and FDI and then divides the result by the CMAP of ADM.
Another approach involves assessing F-wave persistence instead of CMAP. Although F-wave testing can be more sensitive in some cases, it requires repeated stimulation. F-wave responses measure the backfiring of motor neurons after electrical stimulation, offering additional insight into nerve health.
Split hand appears in about half of individuals diagnosed with ALS. Evidence suggests that the split hand index can assist physicians in identifying ALS, especially during early stages when symptoms are still evolving and patients may be actively seeking clarity through resources like a Do I have ALS quiz. Even so, it remains just one piece of the broader diagnostic picture.
How accurate is the split hand index in diagnosing ALS?
The split hand index supports — but does not replace — other established diagnostic evaluations for ALS. It is not used independently to confirm the disease.
A 2021 literature review reported that the split hand index demonstrated a sensitivity of 78% for ALS, meaning it correctly identified ALS in 78% of cases. Its specificity was 81%, indicating it accurately ruled out ALS in 81% of individuals without the condition.
Despite these relatively strong figures, limitations exist. Results may be less reliable when muscle atrophy is either minimal or very advanced. Additionally, the calculation assumes there is no concurrent nerve compression in the hand — such as carpal tunnel syndrome — that could distort nerve conduction findings.
Importantly, split hand is not exclusive to ALS. Specialists have documented similar patterns in other conditions, including:
- spinal muscular atrophy
- spinal and bulbar muscular atrophy (Kennedy’s disease)
- spinocerebellar ataxia-3
Because overlapping symptoms can occur, many people who worry about early hand weakness may ultimately discover signs you don’t have als after appropriate medical testing. Understanding these distinctions can help reduce unnecessary anxiety while encouraging timely evaluation.

What tests are used to diagnose ALS?
There is currently no single definitive test for ALS. Diagnosis typically requires a combination of neurological examination and specialized investigations to exclude other causes of muscle weakness.
In addition to nerve conduction studies, a physician may recommend several other tests, such as:
- electromyography (EMG) to evaluate nerve and muscle function
- MRI to generate detailed images of the brain and spinal cord
- lumbar puncture to analyze cerebrospinal fluid and exclude alternative diagnoses
- muscle biopsy to help characterize the type of ALS
This comprehensive approach ensures that treatable conditions — including nerve compression syndromes, inflammatory disorders, or metabolic imbalances — are not overlooked. For individuals concerned after taking a Do I have ALS quiz, seeking prompt evaluation from a neurologist remains the most reliable next step.
Early signs and symptoms of ALS
ALS leads to progressive degeneration of motor neurons, gradually impairing voluntary movement. Early manifestations may include:
- muscle twitching (especially in the arm, leg, shoulder, or tongue)
- muscle cramps
- muscle stiffness (spasticity)
- muscle weakness (commonly in the neck, arm, or leg)
- slurred speech
- nasal speech
- difficulty chewing
- difficulty swallowing
Symptoms often begin asymmetrically, meaning one side of the body may be affected before the other. Over time, weakness can spread to additional muscle groups. Recognizing early warning signs and differentiating them from benign muscle twitches or anxiety-related sensations is critical. Some people find reassurance in reviewing 5 reasons you DON’T have ALS, but clinical assessment remains essential for clarity.
Frequently asked questions
What does ALS feel like in the hands?
In ALS, the hands may feel weak, yet typically not numb or painful. Individuals might notice dropping objects, struggling with buttons, or difficulty gripping items. The weakness is usually asymmetrical, so one hand may seem weaker than the other.
Which fingers are affected by ALS?
ALS most commonly involves the thumb and index finger, particularly the abductor pollicis brevis (ABD) and first dorsal interosseous (FDI), leading to impaired pinch strength and dexterity.
Are there other split limb signs that suggest ALS?
Researchers propose that a split elbow and a split leg may also indicate ALS.
Split elbow describes a scenario in which the bicep muscle is weaker than the tricep muscle, though research findings in ALS remain mixed.
Split leg refers to foot drop caused by asymmetrical weakening of ankle dorsiflexion muscles. However, foot drop can result from various neurological or orthopedic conditions and is not specific to ALS.
Takeaway
Many individuals with ALS develop split hand at some stage of the disease. While the split hand test and split hand index can strengthen clinical suspicion, they are not sufficient alone to confirm ALS. Diagnostic accuracy depends on a comprehensive neurological assessment, supportive testing, and careful exclusion of other disorders. If you are concerned about persistent hand weakness or other neurological symptoms, professional evaluation is the most important step toward clarity and appropriate care.





















Leave a Reply
You must be logged in to post a comment.