A hemicolectomy is a surgical operation performed to remove a section of the large intestine, also known as the colon. This intervention is typically recommended when a portion of the colon has been damaged by disease or has developed cancer. In many cases, only the affected segment is excised, allowing the remaining sections to continue functioning within the digestive system.
When only part of the colon is removed, digestion can often proceed with minimal disruption. After the diseased segment is taken out, the two healthy ends are surgically connected. For many individuals, this reconnection results in little to no noticeable change in everyday digestion. However, understanding both the immediate recovery and the long-term side effects of right hemicolectomy or left-sided procedures is essential for informed decision-making and ongoing health management.

What it treats
A hemicolectomy may be advised for several medical conditions affecting the colon. Common reasons for this surgery include:
- cancer of your colon or bowels
- trauma or injury to your abdominal area
- inflammatory bowel disease (IBD), such as ulcerative colitis or Crohn’s disease
- polyps, or tissue growths in your colon that can become cancerous
- diverticulitis, which happens when diverticula (small pouches) in your colon get infected or inflamed
In many of these situations, removing the diseased portion of the colon helps prevent complications such as obstruction, bleeding, perforation, or the spread of cancer.
Types
There are two primary forms of hemicolectomy: right and left.
During a right hemicolectomy, the ascending colon (the section attached to the end of the small intestine), the right portion of the transverse colon (which extends across the abdomen), the cecum, and the appendix are removed. The surgeon then connects the small intestine to the remaining transverse colon. Patients researching the long-term side effects of right hemicolectomy should understand that this procedure alters the early part of the colon, which plays a role in absorbing fluids and certain nutrients.
In a left hemicolectomy, the descending colon and the left segment of the transverse colon are excised. This area connects to the rectum. Once removed, the surgeon joins the remaining transverse colon directly to the rectum, restoring bowel continuity.
Health considerations
You are generally considered a suitable candidate for this operation if you are in overall good health aside from the condition requiring treatment.
Certain factors, however, may increase the likelihood of complications. These include:
- pregnancy
- heart conditions
- bleeding or clotting problems
- scar tissue from previous colon or abdominal surgery
- being overweight or obese
- advanced colon cancer or other types of bowel cancer
Discuss your full medical history with your doctor before surgery, especially if any of these conditions apply. A thorough evaluation helps reduce surgical risks and supports safer recovery.
How to prepare for the surgery
Prior to surgery, you may undergo a comprehensive physical exam. This assessment allows your physician to identify any health concerns that could interfere with anesthesia or the surgical procedure.
Your doctor will also inform you if a stoma may be necessary. A stoma is created when the colon is connected directly to the skin’s surface. Waste then exits into a colostomy bag attached externally. Depending on your specific case, this may be temporary or permanent.
If you take medications, ask whether you should stop them beforehand. Many people are advised to discontinue blood thinners such as warfarin (Coumadin) or aspirin, as these drugs can increase bleeding risk during surgery.
A bowel preparation is often required a few days before the operation. This typically involves taking laxatives to empty the intestines. Clearing the digestive tract can simplify the procedure and reduce the risk of infection.
You may also need to fast for up to 12 hours prior to surgery. Your healthcare team will give you detailed instructions about when to stop eating and drinking.
Procedure
When you arrive
On the day of surgery, you’ll check in and change into a hospital gown. You’ll then be positioned on an operating table.
A doctor will administer general anesthesia so you remain asleep and unaware during the procedure.
An intravenous (IV) line will provide fluids, medications, and pain control. A nasogastric tube may be inserted through your nose into your stomach, and a catheter may be placed in your bladder to drain urine. Shortly after, the surgical process begins.
During the surgery
To remove the affected colon segment, the surgeon usually makes several small incisions in the abdomen, a technique known as laparoscopic (keyhole) surgery. In certain cases, open surgery is required, involving a larger incision to fully access the colon.
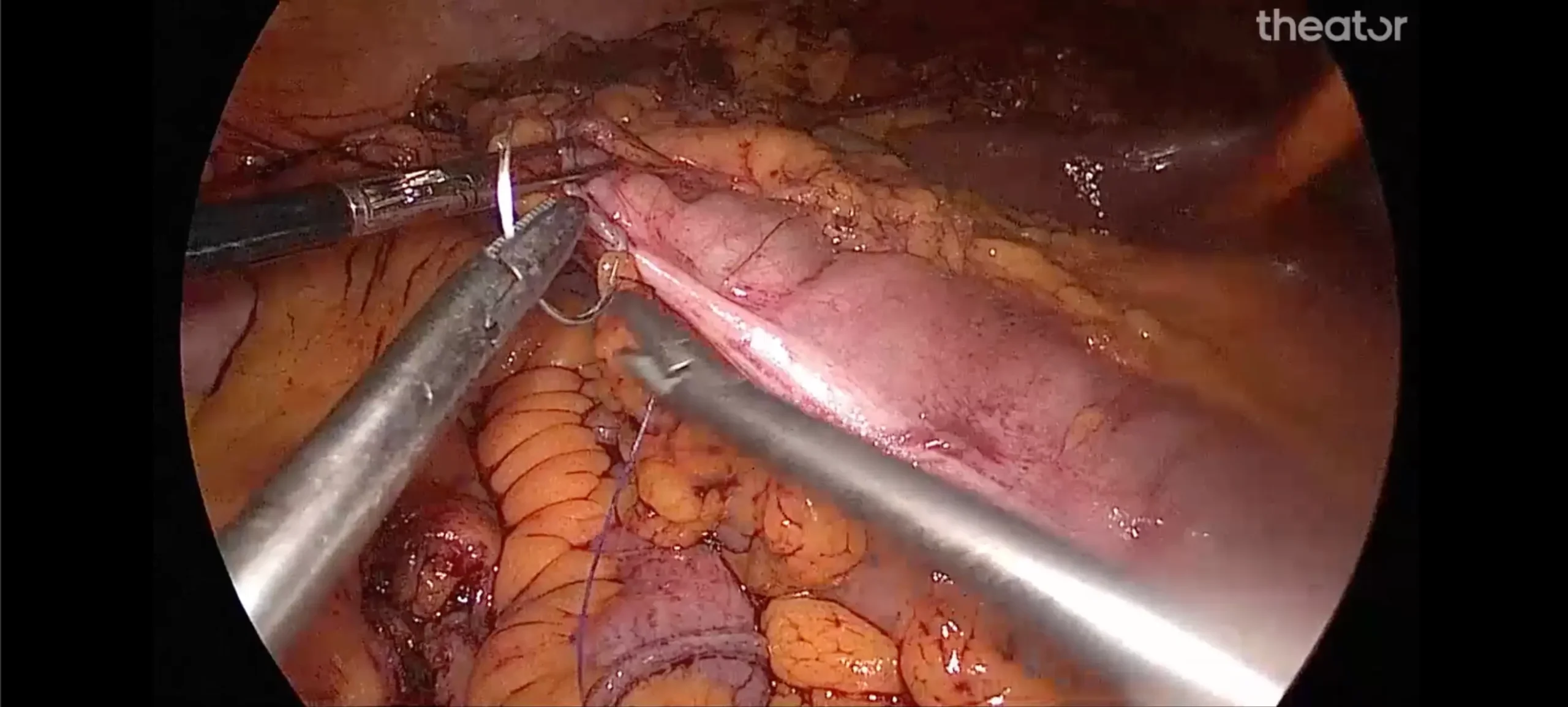
The surgeon removes the diseased portion of the colon along with any directly attached sections of intestine, such as the end of the small intestine or part of the rectum. Nearby lymph nodes and blood vessels connected to that colon segment are also removed, particularly in cancer cases.
After resection, the remaining sections are reconnected.
If you undergo a right hemicolectomy, the colon is joined to the end of the small intestine. If you have a left hemicolectomy, the remaining colon is attached to the rectum. This reconnection is called anastomosis.
If reconnection is not possible, the surgeon may create a stoma, connecting the colon to the abdominal skin. You would then wear a colostomy bag to collect waste. Depending on healing and underlying disease, this may be temporary or permanent.
A hemicolectomy generally lasts around two hours, although complications can extend this time.
Recovery
A hemicolectomy is considered major abdominal surgery. Full recovery may take several weeks or longer.
When you awaken, you may feel drowsy due to anesthesia. Initially, pain is often controlled with IV medications.

Over the following days, your doctor will monitor your pain levels, bowel function, and ability to tolerate food. Before discharge, your care team will confirm that you can pass gas and stool and that no signs of infection or other complications are present.
Hospital stays range from a few days to one or two weeks, particularly if open surgery was performed.
Before going home, you may receive prescriptions such as ibuprofen (Advil) for pain and docusate (Colace) to reduce constipation. Supporting bowel regularity is especially important when considering the potential long-term side effects of right hemicolectomy, which can include changes in bowel habits. You can also explore guidance on Quality of life after right hemicolectomy to better understand recovery expectations.
At home, limit strenuous activity for several weeks. Avoid lifting heavy objects for at least six weeks or as directed by your surgeon.
Post-surgery diet
Even after partial colon removal, many people experience minimal long-term digestive disruption. In some cases, dietary adjustments are temporary and primarily needed during recovery.
If you develop diarrhea or abdominal cramping, your doctor may suggest foods that help regulate bowel movements, such as:
- applesauce
- bananas
- cheese
- fiber-rich foods or supplements
- oatmeal or cream of wheat
- pasta
- potatoes
- mild teas
- yogurt
Staying hydrated is crucial. Drinking water or electrolyte-containing beverages such as Gatorade can help prevent dehydration, particularly if bowel movements are more frequent. Over time, most individuals adapt, though some may notice persistent differences that are considered part of the long-term side effects of right hemicolectomy.
Risks
As with any major procedure, hemicolectomy carries risks related to anesthesia and surgery. Contact your doctor immediately if you experience:
- diarrhea or constipation that lasts for a few days
- fever of 100˚F (37.8˚C) or higher
- irritation or pus around the cuts in your abdomen
- pain in your abdominal area that doesn’t stop with medication
Other possible complications include:
- leakage around the area where your colon was rejoined
- blood clots in your lungs or legs during or after surgery
- infections
- damage to organs surrounding your colon
- blockage in your colon due to scar tissue
- lateral anterior resection syndrome (LARS), which can be a complication when part of the rectum is removed, but is not generally common following a hemicolectomy
Preventive strategies such as early mobilization, compression devices, and anticoagulant therapy may reduce the risk of blood clots.
Outlook
Within a few months, surgical incisions typically heal, and abdominal discomfort subsides.
If the hemicolectomy was performed to treat cancer, additional therapies such as chemotherapy may be necessary to prevent recurrence or spread. Regular follow-up appointments are essential.
If you require a colostomy bag, your doctor will discuss the expected duration and whether reversal is possible.
Most individuals return to a normal diet and daily routine after recovery. While many notice little change in bowel function, some may experience ongoing shifts in stool frequency or consistency. Understanding the potential long-term side effects of right hemicolectomy empowers patients to make lifestyle adjustments—such as balanced nutrition, adequate hydration, and regular medical follow-up—to maintain optimal colon health over time.






















Leave a Reply
You must be logged in to post a comment.