Fluctuating hormones in the perimenopausal period often lead to bouts of bloating. For many people, dietary tweaks, lifestyle shifts, or medications can significantly lessen menopause-related bloating.

Menopause is widely known for symptoms such as hot flashes and changes in reproductive function. Yet the hormonal shifts that come with menopause also produce a variety of other effects, including gastrointestinal symptoms like bloating.
Bloating produces a sensation of fullness, tightness, or swelling in the abdomen and sometimes other parts of the body. It can be uncomfortable and disruptive.
Continue reading to find out how to manage bloating associated with menopause and when it might indicate the need for medical evaluation.
What makes bloating happen during menopause?
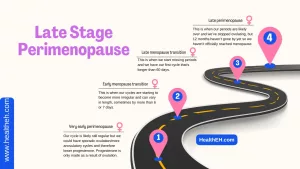
Menopause is defined by the absence of menstrual periods for 12 consecutive months, caused by the ovaries ceasing production of estrogen and progesterone. The gradual transition leading up to this phase is called perimenopause.
Hormone levels shift rapidly during perimenopause. Estrogen does far more than govern reproduction; it also helps control how your body manages water. Rapid ups and downs in estrogen during perimenopause can cause fluid retention, which may manifest as bloating.
Research, including a 2022 review, suggests that hormonal changes during this time may alter the gut microbiome. Those changes can affect intestinal motility and potentially contribute to bloating, though further study is needed.
Bloating is often more common in the perimenopausal stage than in menopause or postmenopause.
Postmenopausal bloating can also result from excess gas in the digestive tract. Causes include:
- diet
- exercise patterns
- stress
- smoking
- swallowed air
- an underlying health condition
After menopause, hormonal fluctuations are usually less dramatic, so persistent bloating is more likely linked to one of the factors above rather than ongoing hormonal swings.
How can I prevent or ease bloating during menopause?
Many people find relief from bloating through practical lifestyle changes. These strategies can also help reduce the chance of bloating developing in the first place.
- Modify your diet: Limit foods that trigger bloating, such as high-fat meals, certain gas-producing vegetables, and dairy if you’re sensitive. Steer clear of heavily processed foods high in sugar and salt. Some specialists suggest a low FODMAP approach for those with IBS-related bloating.
- Increase physical activity: Aim for regular workouts several times per week, mixing cardiovascular and strength-training exercises.
- Avoid gum and fizzy drinks: Chewing gum and carbonated beverages can introduce extra air into your stomach, leading to abdominal distension.
- Quit smoking and limit alcohol: Smoking can irritate the stomach lining, and alcohol may disturb fluid balance—both can contribute to bloating.
- Stay well hydrated: Inadequate fluid intake can paradoxically lead to fluid retention and bloating, so drink enough water.
There are also OTC and prescription options that can help prevent or treat bloating:
- Antibloating remedies: Available over the counter; a pharmacist or physician can suggest one that might work for you.
- Diuretics: Prescription medications that reduce fluid retention can be used under a doctor’s supervision when appropriate.
- Hormonal birth control pills: If you’re still menstruating, certain birth control pills can stabilize hormones and reduce bloating and other premenstrual symptoms. Discuss suitability with your clinician.
- Menopausal hormone therapy (MHT): Some people opt for MHT to even out estrogen and progesterone levels during menopause. Talk with your doctor about potential benefits and risks before starting.
Is it bloating or actual weight gain?
During perimenopause and menopause, it can be hard to tell whether you’re dealing with bloating or increased weight. Hormonal shifts at this time can make it easier to gain weight, especially around the midsection.
Weight gain isn’t only tied to menopause; aging, lifestyle choices, and genetics can also play major roles.
Bloating is typically temporary. You’ll notice your abdomen expanding and contracting over the course of a day with bloating. By contrast, true weight gain results in a more consistent increase in abdominal size that doesn’t vary as noticeably throughout the day.
When should I see a doctor?
Mild bloating during hormonal changes is common, but persistent or painful bloating merits prompt medical attention.
Ongoing bloating lasting weeks could signal ovarian cancer or another medical issue, such as:
- IBS
- gastroesophageal reflux disease
- celiac disease
Key points
Bloating is a common symptom during perimenopause and menopause, often linked to fluctuating hormones. Lifestyle modifications, dietary changes, and certain medications can help manage it.
After menopause, when estrogen and progesterone production declines and hormone levels stabilize, bloating tends to become less frequent.






















Leave a Reply
You must be logged in to post a comment.