Actinic purpura is a benign condition characterized by easy bruising that primarily affects older adults. It is also commonly referred to as “senile purpura.” This condition develops because, as we age, the skin and underlying blood vessels become thinner and more delicate, making them increasingly vulnerable to bruising from even minor bumps or trauma. It differs from disorders that cause easy bruising due to underlying bleeding abnormalities.
For individuals searching for Mild elderly skin bruising pictures, actinic purpura is one of the most frequently identified causes of purple marks on aging skin. Reviewing reliable visual references, such as Elderly skin bruising pictures, can help distinguish typical age-related bruising from signs that may require medical evaluation.
Actinic purpura is relatively common, affecting approximately 10 percent of individuals over the age of 50. The prevalence rises steadily with advancing age, reflecting the cumulative effects of sun exposure and natural skin thinning over time.
What are the symptoms of actinic purpura?
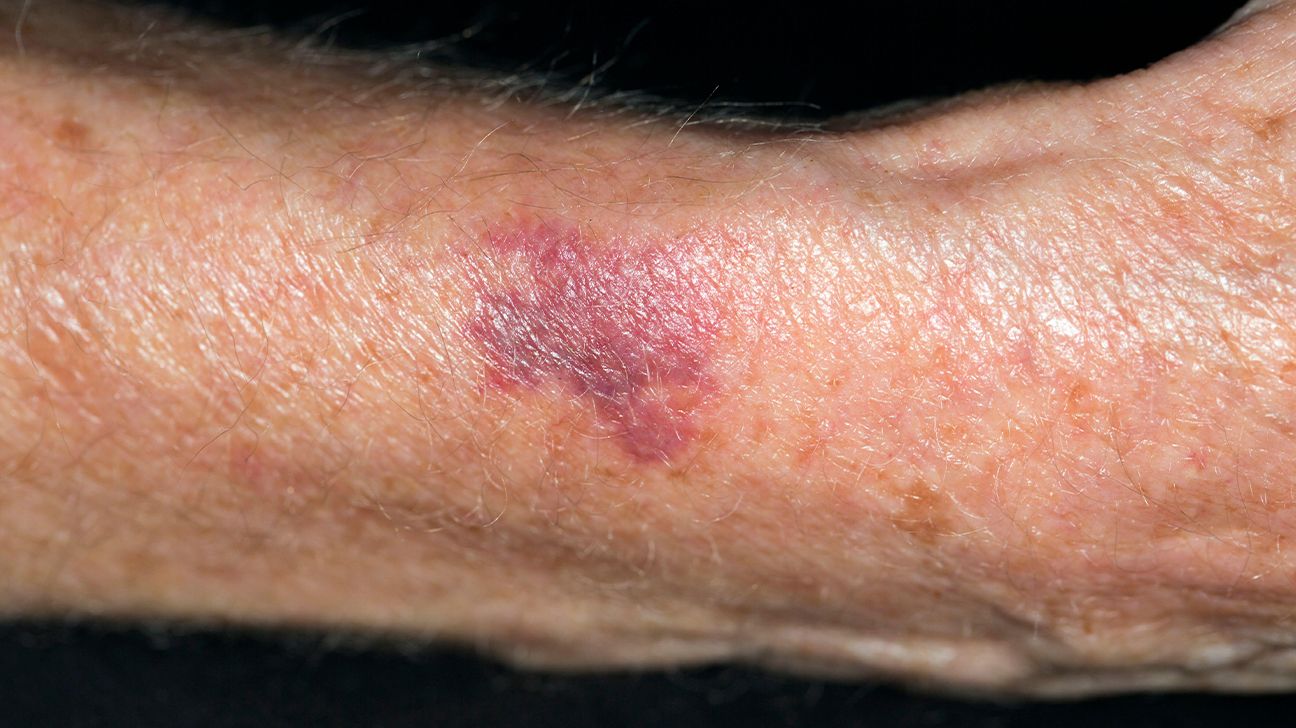
The hallmark sign of actinic purpura is the appearance of large, purplish-red bruises, most frequently seen on the backs of the hands and along the forearms. As these marks resolve, they often transition into a brownish discoloration.
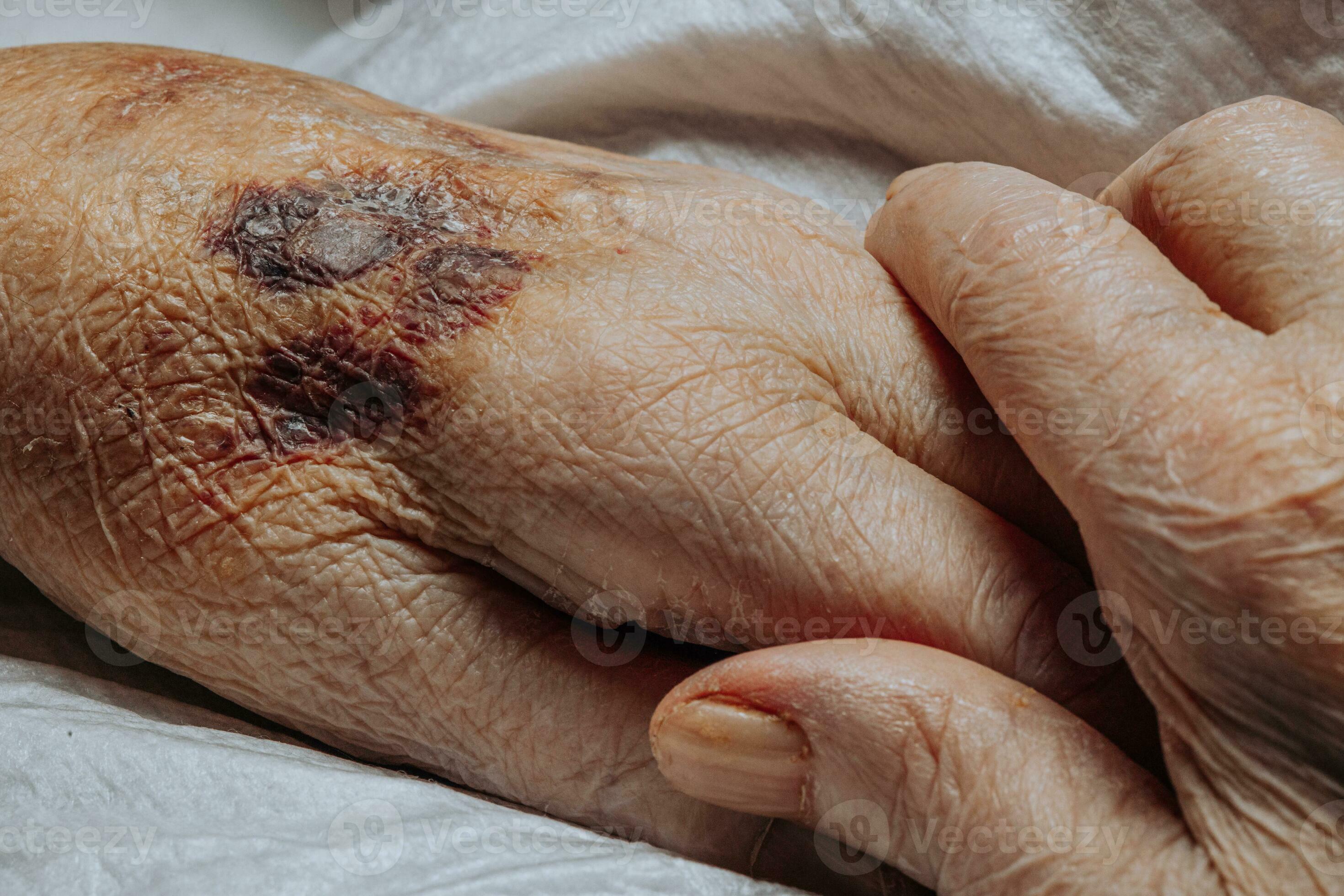
These bruises generally persist for one to three weeks before gradually fading. Unlike typical bruises that change colors—progressing through blue, green, or yellow stages during healing—lesions from actinic purpura tend to fade directly to brown. In some individuals, this brown pigmentation may linger and occasionally become permanent.
Although purpuric lesions are most commonly observed on sun-exposed areas such as the hands and forearms, they may also develop on mucous membranes, including those inside the mouth, and in rare cases, within internal organs.
What causes actinic purpura?
The primary contributing factor in the development of actinic purpura is thinning skin that is more susceptible to injury. Chronic sun exposure plays a significant role, as ultraviolet (UV) radiation gradually weakens connective tissue and damages collagen over time. This structural decline reduces the skin’s ability to protect the small blood vessels beneath it.
Vascular diseases and medications that influence blood vessel integrity can also increase the likelihood of developing actinic purpura. Conditions such as diabetes, rheumatoid arthritis, and lupus may further elevate the risk of purpuric lesions.
Certain medications, including corticosteroids and aspirin, can worsen or intensify bruising by affecting blood vessel strength or clotting mechanisms.
In many instances, actinic purpura appears after very minor trauma—sometimes so subtle that the individual does not recall any specific injury—even though the bruise may look severe.
How is actinic purpura diagnosed?
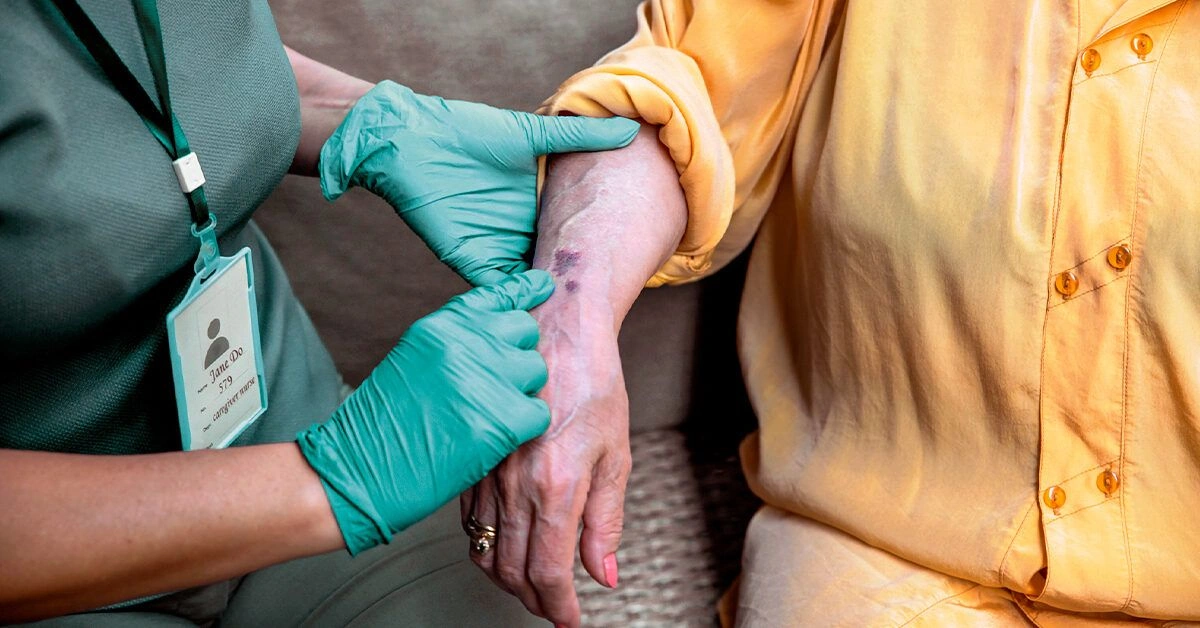
If you notice a sudden increase in large bruises, particularly on sun-exposed areas of your arms or hands, it is important to schedule an appointment with your healthcare provider.
Your doctor will review your symptoms, medical history, and current medications, followed by a physical examination. If the ecchymoses (lesions) are painless, localized to the hands and forearms, and not associated with other unusual bleeding symptoms, your physician will typically diagnose actinic purpura based on clinical findings alone.
In some cases, especially if the bruising pattern appears atypical, additional evaluation may be recommended to rule out other causes. For example, individuals comparing their symptoms with Cancer bruises pictures may become concerned about serious conditions. A medical assessment can help differentiate benign age-related bruising from bruising linked to hematologic or systemic disorders.
How is actinic purpura treated?
Most cases of actinic purpura do not require medical treatment, as the condition is harmless. However, some individuals seek therapy due to cosmetic concerns or frequent recurrence.
Your doctor may prescribe topical retinoids, which can help thicken the skin and slow further skin aging. By improving dermal structure, retinoids may reduce the likelihood of future purpuric lesions. It is important to note that retinoids can cause side effects, and for some patients, these adverse effects may outweigh the potential benefits.
Taking protective measures to prevent minor trauma is also beneficial. Wearing long sleeves or protective shin guards during activities can reduce the risk of impact-related bruising, especially in those with fragile skin.

Natural remedies
Some individuals explore supportive or complementary approaches. Taking citrus bioflavonoids twice daily has been suggested as a potential natural option for actinic purpura. One study demonstrated a 50 percent reduction in purpura lesions among a group of 70 older adults.
A 2015 study reported that applying epidermal growth factor directly to the skin twice daily increased skin thickness and reduced the number of purpuric lesions experienced by participants.
There has also been interest in topical vitamin K for managing bruising. One study found that using topical vitamin K after laser treatment helped reduce bruising. However, no studies have specifically evaluated topical vitamin K in individuals with senile purpura.
What is the outlook for actinic purpura?
Actinic purpura is a harmless and non-life-threatening condition. However, without preventive measures, the bruising may recur over time. Protecting your skin from additional sun damage by applying broad-spectrum sunscreen regularly can help slow further thinning and connective tissue damage.
Most purpuric lesions resolve within one to three weeks, although residual brown discoloration may persist in some cases. Consulting a dermatologist can provide additional guidance on minimizing the cosmetic appearance of these marks and developing a long-term skin protection plan.
For those researching Mild elderly skin bruising pictures to better understand normal age-related changes, it is essential to combine visual comparisons with professional medical advice. While actinic purpura is common and benign, any sudden, unexplained, or widespread bruising should always be evaluated by a healthcare professional to ensure accurate diagnosis and peace of mind.















Leave a Reply
You must be logged in to post a comment.