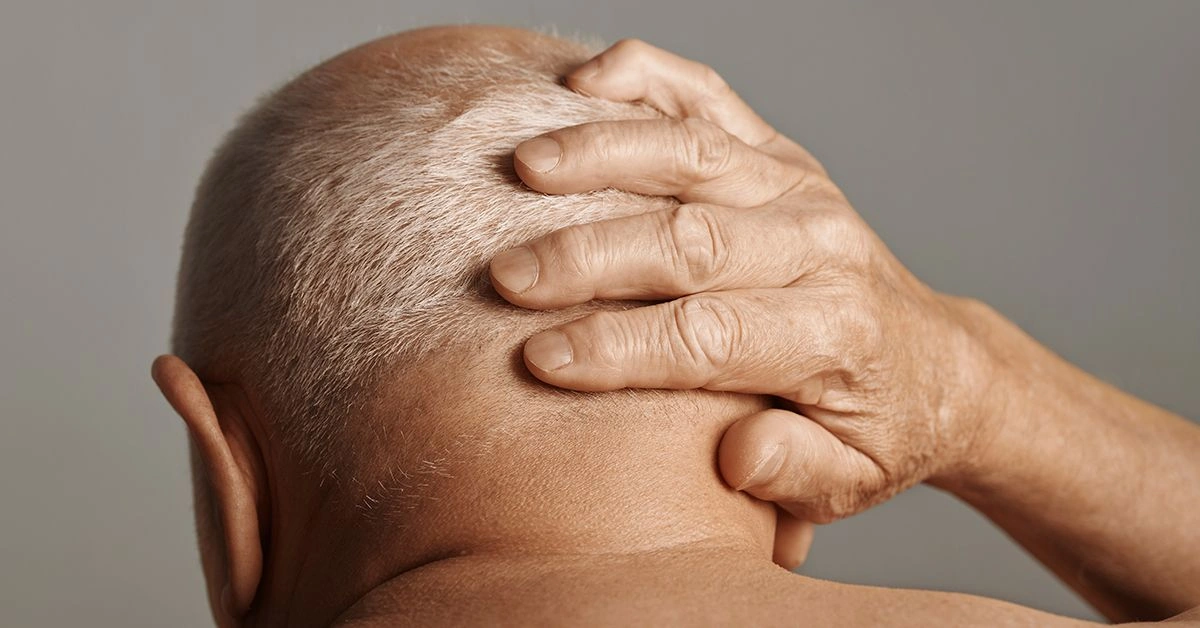
Suboccipital headaches commonly arise from compression of nerves at the rear of the neck. You might experience sharp, shooting pain across the scalp that can resemble migraine attacks.
The occipital bone sits at the lower back portion of the skull. “Suboccipital” denotes the area beneath this bone that houses muscles, nerves, and other vital structures.
Suboccipital headaches develop when nerves in this region become compressed. Several factors can cause this compression, including:
- arthritis
- tumors
- degeneration of cervical discs
A less common issue called Chiari malformation can also produce suboccipital headaches.
Continue reading to find out more about suboccipital headaches, including their causes, symptoms, and available treatments.
Suboccipital headache causes and triggers
When one of three nerves at the back of the neck becomes compressed, it can produce occipital neuralgia, characterized by stabbing or shooting head pain. These nerves are:
- greater occipital nerve
- lesser occipital nerve
- third occipital nerve
About 90% of cases originate from the greater occipital nerve. The lesser occipital nerve accounts for roughly 10%, while the third occipital nerve is an uncommon source.

Other reasons for suboccipital headaches include:
- irritation of nerves stemming from the upper spinal cord (cervicogenic headache)
- injury to the muscles at the back of the head
- Chiari malformation, where brain tissue protrudes into the spinal canal
Who gets suboccipital headaches?
Occipital neuralgia is estimated to affect around 3.2 per 100,000 people, with an average diagnosis age of 54 in studies from the Netherlands.
Possible contributing factors linked to occipital neuralgia include:
- osteoarthritis
- trauma to occipital nerves
- cervical disc disease
- tumors compressing the C2 or C3 nerve roots
- gout
- diabetes
- blood vessel inflammation
- infections
Cervicogenic headaches that result from irritation of neck nerves most often occur between ages 30 and 44.
The most frequent form of Chiari malformation is present in about 0.5–3.5% of people and is slightly more common in females than males.
Suboccipital headache symptoms
Symptoms of occipital neuralgia include:
- constant pain described as: aching, burning, throbbing
- intermittent pain described as: shooting, shocking
As noted by the National Institute of Neurological Disorders and Stroke, pain is commonly felt in the:
- upper back
- rear of the head
- behind the eyes and ears, typically on one side
- scalp
- forehead
Pain usually begins at the base of the skull and radiates to the scalp on one or both sides. Simple actions like brushing your hair may provoke pain. Many people compare the sensation to migraine or cluster headaches.
Chiari malformation symptoms
Signs of a Chiari malformation can include:
- headaches
- neck pain
- dizziness
- balance difficulties
- blurred or double vision
- muscle weakness
Cervicogenic headache symptoms
Symptoms of a cervicogenic headache may include:
- throbbing head pain
- pain affecting one side of the face
- stiffness in the neck
- ache around the eyes
- pain that worsens with particular neck movements
Potential complications of suboccipital headaches
Occipital neuralgia and cervicogenic headaches can lead to pain that diminishes quality of life. Serious complications are uncommon, but there has been a report of intraventricular hemorrhage causing death after radiofrequency ablation, a seldom-used treatment for occipital neuralgia.
Many individuals with Chiari malformation have good outcomes, yet surgery for severe cases can bring complications such as:
- cerebrospinal fluid leakage
- meningitis
- infections
- unusual collections of cerebrospinal fluid
- brainstem dysfunction
- bleeding beneath the skull
- sleep apnea
- arterial injury
When to seek medical care
See a healthcare provider if you experience sharp or unusual pain in your neck or scalp, particularly if the pain is persistent and lacks a clear cause.
Suboccipital headache diagnosis
Tests used to diagnose suboccipital headaches may include:
- physical examination
- neurological assessment
- magnetic resonance imaging (MRI)
- computed tomography (CT) scans
- occipital nerve block procedures
Mild Chiari malformations are usually assessed with MRI in children and adults. More severe forms can be detected before birth with an ultrasound.
Suboccipital headache treatment
Treatment for suboccipital headaches can be surgical or nonsurgical.
Nonsurgical treatments
Conservative treatment options for occipital neuralgia and cervicogenic headaches include:
- Botox injections
- occipital nerve blocks
- medications such as anti-inflammatory drugs, muscle relaxants, and anticonvulsants
- physical therapy
- massage therapy
- heat therapy
Suboccipital headache exercises
Specific exercises can help strengthen neck muscles and reduce headaches caused by nerve compression. A physical therapist can create a tailored exercise plan to ease your symptoms.
Learn more about exercises for occipital neuralgia.
Surgical treatments
Possible surgical approaches include:
- occipital nerve stimulation, where an electrode is placed beneath the skin
- spinal cord stimulation
- C2 or C3 ganglionectomy (removal of sensory cells from the cervical ganglion)
Cervicogenic headache treatment
Physiotherapy is typically the first-line treatment for cervicogenic headaches. Other interventions include:
- corticosteroid injections
- aspirin or ibuprofen
- acetaminophen (Tylenol)
- muscle relaxants
- surgery to ease nerve compression
Chiari malformation treatment
A Chiari malformation that causes no symptoms may not need intervention. Surgery is considered if it produces symptoms.
Learn more about Chiari malformation surgery.
Living with suboccipital headaches
Many people with occipital neuralgia or cervicogenic headaches achieve short-term relief with treatment. Some experience symptom relief from nerve blocks lasting up to several months.
Mild Chiari malformations are generally not life-threatening, though some individuals may have ongoing weakness or difficulty walking.
Can you prevent suboccipital headaches?
Some risk factors for occipital neuralgia are modifiable. You might lower your risk of these headaches by:
- following a healthy diet to reduce diabetes risk
- exercising regularly to help prevent diabetes and degenerative disc disease
- avoiding tobacco to decrease disc disease risk (a doctor can help with a cessation plan)
- taking precautions to avoid traumatic injuries
- maintaining good posture to lessen neck strain
Takeaway
Conservative care like physiotherapy and medications may suffice to control symptoms. If these measures fail, surgery might be necessary. With appropriate treatment, many people experience symptom improvement.



















Leave a Reply
You must be logged in to post a comment.