Atrial tachycardia is an abnormal heart rhythm in which the upper chambers of the heart beat faster than normal. During an episode of atrial tachycardia, your heart rate can rise above 100 beats per minute (bpm), even when you’re at rest.

This condition belongs to a broader category known as arrhythmia. Arrhythmias are disorders marked by a heart rate that may be:
- faster than normal
- slower than normal
- irregular or otherwise abnormal in rhythm
What is atrial tachycardia?
Atrial tachycardia refers to an unusually rapid heart rate that begins in the atria, the upper chambers of the heart.
The heart contains four chambers: two atria on top and two ventricles on the bottom. When a fast rhythm originates above the ventricles, it’s classified as supraventricular tachycardia.
The term “tachycardia” simply means a fast heart rate. It is described as atrial when it starts in the atria and ventricular when it begins in the lower chambers.
Atrial tachycardia is more frequently seen in individuals who have undergone heart surgery or who were born with congenital heart defects. In many cases, it doesn’t lead to noticeable symptoms or serious complications. However, persistent episodes can increase the likelihood of developing cardiomyopathy, a condition that affects the heart muscle.
Heart rhythm disturbances can also appear after surgical procedures. For individuals wondering What causes tachycardia after surgery, scar tissue formation, inflammation, fluid shifts, and stress on the heart are recognized contributors to abnormal electrical signaling in the atria.
During episodes of atrial tachycardia, the heart rate may exceed 100 bpm, even without physical exertion.
The primary forms of atrial tachycardia include:
- Focal atrial tachycardia: Caused by abnormal electrical impulses arising from a single area within the atria. It often occurs in situations that increase metabolic demand or stress the heart, such as infections.
- Multifocal atrial tachycardia: Develops when abnormal electrical activity originates from multiple sites within the atrium.
- Re-entrant atrial tachycardia: Commonly occurs after heart surgery due to the development of scar tissue that disrupts normal electrical pathways.
Learn more about arrhythmia and how it affects heart rhythm.
What are the symptoms of atrial tachycardia?
Some individuals with atrial tachycardia experience no symptoms at all. In certain cases, a doctor may identify the arrhythmia incidentally while monitoring heart activity for another medical reason.
When symptoms are present, they may include:
- chest pain
- lightheadedness
- dizziness
- faintness
- heart palpitations, or brief sensations of fluttering or pounding in the chest
- a clearly elevated heart rate
In some people, atrial tachycardia develops as a result of another underlying condition. For instance, multifocal atrial tachycardia is linked to chronic obstructive pulmonary disease (COPD) in approximately 60% of cases.
Symptoms of COPD may include:
- shortness of breath, particularly during or after physical activity
- a persistent cough that worsens over time
- frequent throat clearing
- recurrent respiratory infections
- fatigue and low energy
Is atrial tachycardia the same as AFib?
Atrial fibrillation (AFib) is the most common arrhythmia. Although both AFib and atrial tachycardia are types of supraventricular tachycardia, they differ in their underlying mechanisms, clinical features, and management strategies.
AFib is described as paroxysmal when episodes last fewer than 7 days and persistent when they continue beyond 7 days.
Individuals with AFib have an increased risk of blood clot formation. If a clot travels to the brain, it can result in a stroke.
Atrial flutter
Atrial flutter is another arrhythmia that begins in the atria.
In this condition, abnormal electrical impulses cause the atria to beat rapidly and ineffectively, leading to a fluttering motion rather than coordinated contractions.
Symptoms of atrial flutter are often milder compared with AFib, although medical evaluation is still important.
Explore the distinctions between atrial flutter and AFib for a clearer understanding of these rhythm disorders.
What causes atrial tachycardia?
Atrial tachycardia can arise from structural abnormalities in the heart that are present at birth or develop later in life. It is frequently observed in people who have undergone heart surgery for other cardiac conditions. In fact, when considering What causes tachycardia after surgery, postoperative inflammation, electrolyte imbalances, and surgical scar formation are recognized triggers for re-entrant atrial tachycardia.
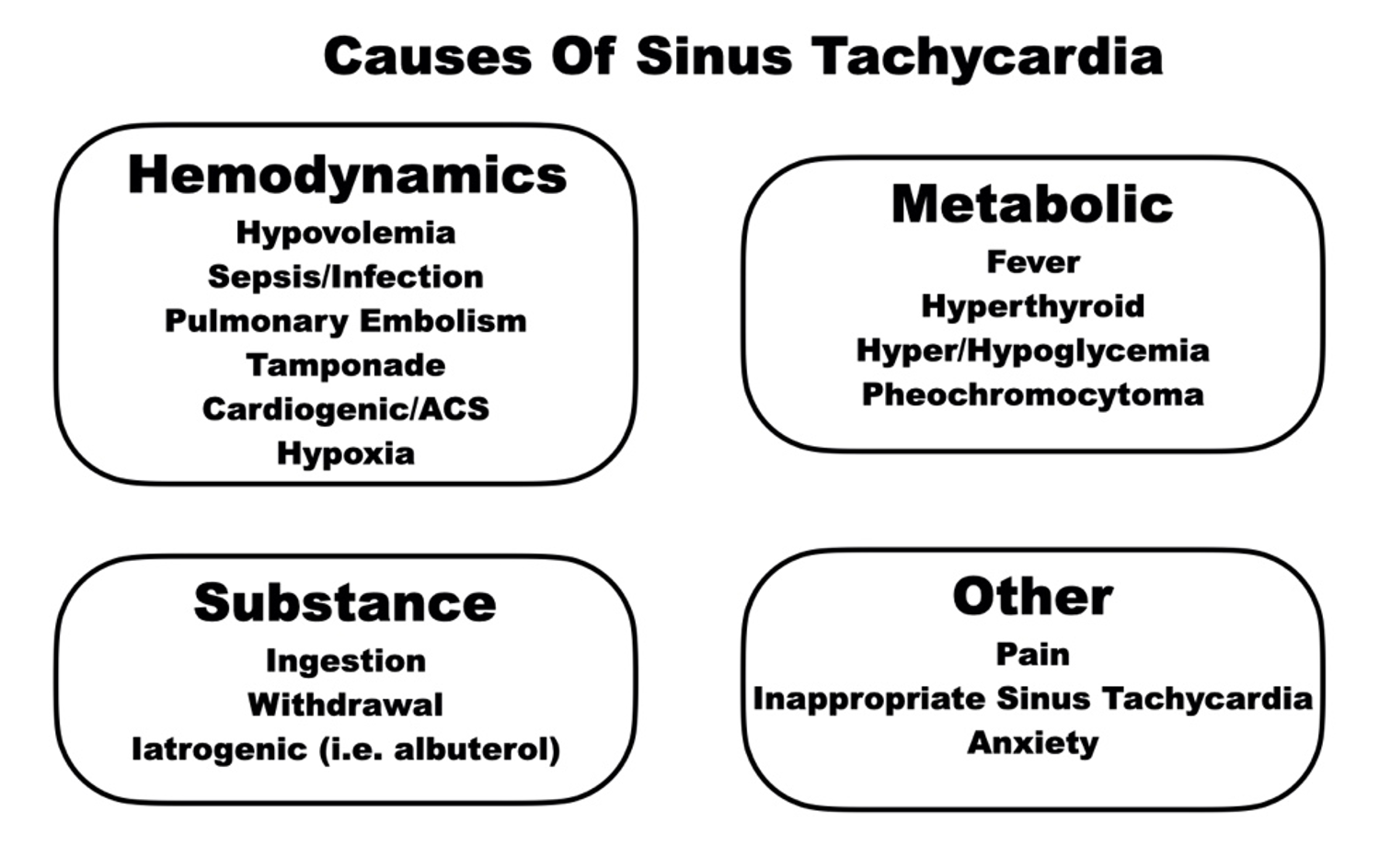
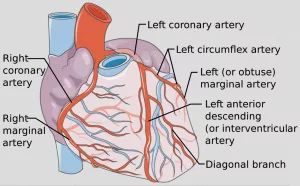
The condition may also signal underlying heart diseases such as coronary artery disease or heart failure.
However, atrial tachycardia can occur even in individuals without structural heart abnormalities. Potential triggers include:

- low blood oxygen levels
- lung disease
- heart disease
- stimulants such as cocaine, caffeine, and ephedra
- excessive alcohol consumption
- digoxin toxicity
Understanding the risk factors for arrhythmia can help guide prevention and early intervention.
How do doctors diagnose and treat atrial tachycardia?
Diagnosis typically involves an electrocardiogram (ECG), a noninvasive test that records the heart’s electrical activity. In some cases, atrial tachycardia is discovered unexpectedly during routine monitoring.
If an arrhythmia is suspected but not captured on a standard ECG, a doctor may recommend wearing a Holter monitor. This portable ECG device continuously records heart rhythms over several days, increasing the chance of detecting intermittent episodes.
Treatment
If atrial tachycardia is not producing symptoms and is unlikely to cause complications, a doctor may advise ongoing observation without immediate intervention.
Lifestyle modifications are often recommended to reduce triggers and support overall cardiovascular health. These may include:
- cutting back on caffeine
- managing stress effectively
- adopting a balanced diet with fewer processed foods
- reducing alcohol intake
When medical therapy is necessary, doctors may prescribe medications that slow the heart rate, such as calcium channel blockers or beta-blockers.
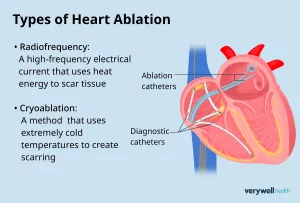
If medications do not adequately control the arrhythmia, a procedure called cardiac ablation may be considered. During this treatment, a specialist guides a thin, flexible catheter through a blood vessel to the heart.
An electrophysiology doctor uses an electrode to eliminate the small area of heart tissue responsible for the abnormal rhythm. In some cases, cryoablation is performed, which destroys the targeted tissue using extreme cold.
Management strategies can vary depending on the cause. For example, approaches to Postoperative tachycardia treatment may address inflammation, fluid balance, and underlying surgical factors. Patients recovering from surgery often ask How long does postoperative tachycardia last, and the duration can differ based on the individual’s health status and the type of procedure performed.
Discover more about diagnostic tests and procedures used to evaluate arrhythmia.
Outlook
Atrial tachycardia does not always cause complications or reduce life expectancy. However, it may be a sign of an underlying condition that requires treatment, such as COPD or coronary artery disease.
When atrial tachycardia persists over time, it can contribute to cardiomyopathy, a disorder affecting the heart muscle. Symptoms of cardiomyopathy may include:
- shortness of breath during exertion
- swelling in the lower extremities
- chest pain
Cardiomyopathy is also associated with a small risk of sudden cardiac death.
Takeaway
Atrial tachycardia is a fast heart rhythm that begins in the upper chambers of the heart. Some people experience no symptoms, while others may notice a rapid pulse, palpitations, or chest discomfort.
If you detect changes in your heart rhythm or develop concerning symptoms, it’s essential to seek medical evaluation. A healthcare professional can determine whether monitoring, medication, or a procedure is appropriate.
When treatment is required, options may include calcium channel blockers, beta-blockers, or cardiac ablation if medications are ineffective. Early assessment and individualized care are key to managing atrial tachycardia safely and effectively.


















Leave a Reply
You must be logged in to post a comment.