When asking, What is the first sign of Huntington’s disease, it’s important to understand that early symptoms are often subtle and easy to overlook. In many cases, the earliest indications involve minor changes in coordination. A person may appear slightly clumsy, experience unexpected difficulty with balance, or have trouble performing tasks that once felt automatic. These early neurological changes can develop gradually, making them difficult to immediately recognize as part of a larger condition.
In addition to physical coordination challenges, early cognitive changes may also emerge. Individuals might notice difficulty concentrating, making decisions, organizing tasks, or solving problems. These shifts can affect daily functioning at work or home. Because Huntington’s disease is a progressive neurodegenerative disorder, these mild symptoms tend to evolve slowly before becoming more noticeable over time.
The condition typically worsens gradually and may eventually lead to more defined physical symptoms, such as:
- uncontrolled movements
- difficulty walking
- unusual eye movements
- slurred speech
- difficulty eating
- insomnia
- fatigue
These uncontrolled movements, often associated with chorea, can interfere with everyday tasks and mobility. Walking may become unsteady, increasing the risk of falls. Changes in eye movement can affect reading and visual tracking, while slurred speech may make communication more challenging. Difficulty eating can sometimes contribute to unintended weight loss or nutritional concerns. Sleep disturbances like insomnia and persistent fatigue can further affect overall quality of life.
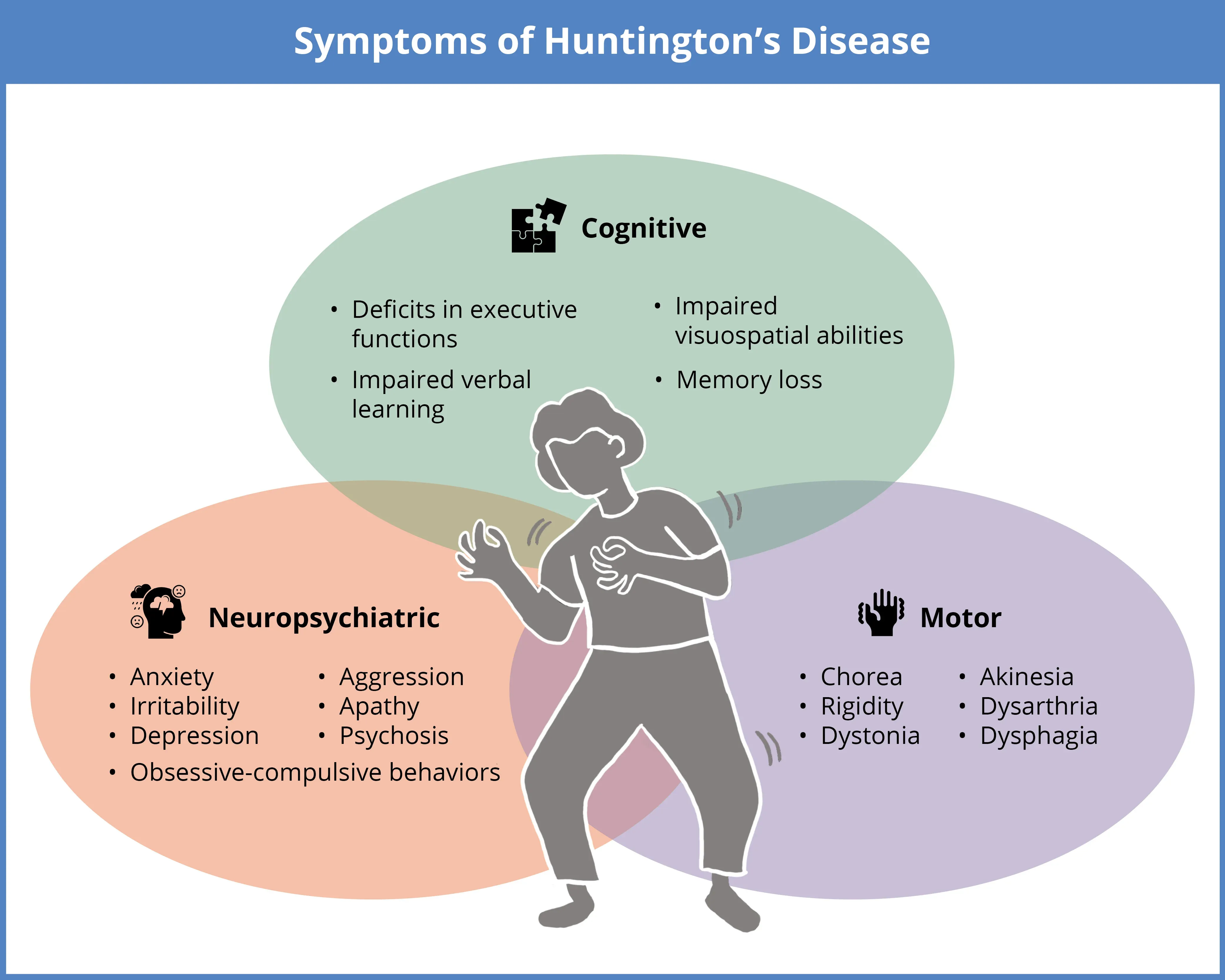
Beyond physical symptoms, Huntington’s disease can significantly influence emotional well-being and behavior. You may begin to feel:
- irritable
- uninterested in usual activities
- uninterested in socializing or being active
- apathetic
- depressed
- frustrated
Mood and personality changes are common and may even appear before noticeable motor symptoms. Some individuals withdraw socially or lose interest in hobbies they once enjoyed. Others may experience depression, irritability, or emotional instability. These psychiatric symptoms are not simply reactions to a diagnosis—they are part of the neurological changes occurring in the brain. As the disease advances, symptoms tend to intensify and become more apparent to both the individual and those around them.
Understanding What is the first sign of Huntington’s disease can be crucial for early evaluation, especially for individuals with a known family history. Since Huntington’s disease is inherited in an autosomal dominant pattern, having a parent with the condition significantly increases the likelihood of developing it. Early recognition allows for medical monitoring, supportive care planning, and informed decision-making.
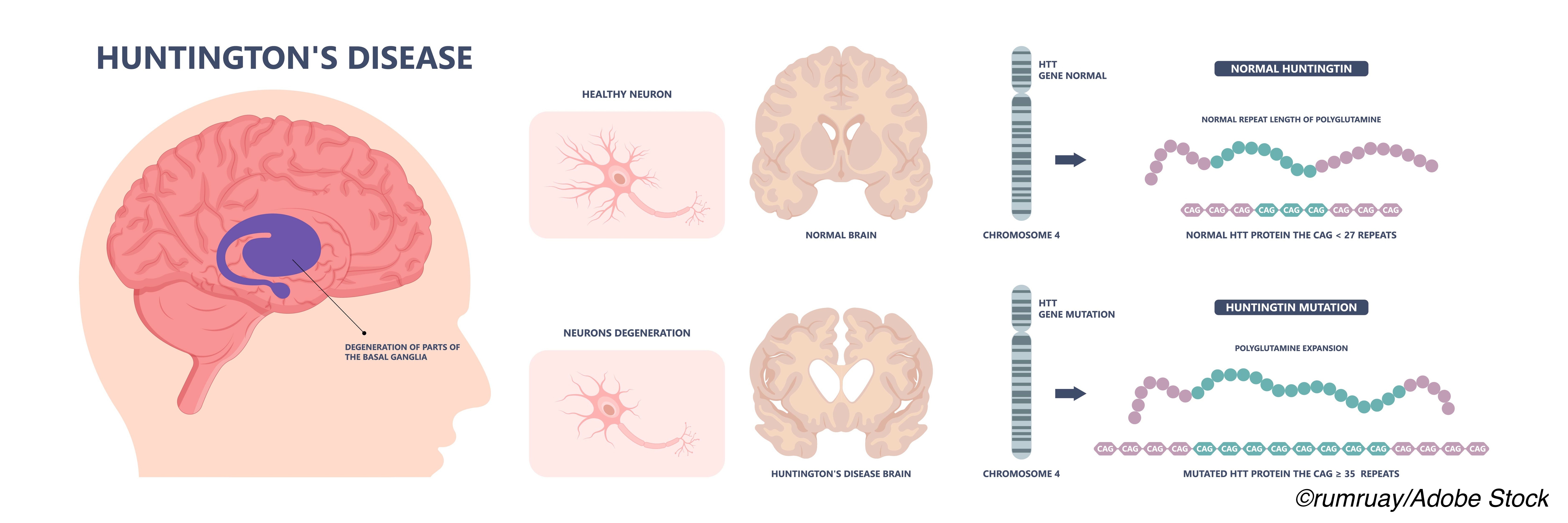
How is Huntington’s disease diagnosed?
To diagnose Huntington’s disease, a doctor will typically use several types of tests to confirm if you have the condition. The diagnostic process is comprehensive and focuses on evaluating neurological function, family history, and genetic confirmation.
The evaluation usually begins with a detailed medical history. Your doctor will ask about your symptoms, when they started, and how they have progressed. They will also inquire about any family history of Huntington’s disease or related neurological disorders. This information is essential, as it can help identify inherited risk and rule out other medical conditions that may produce similar symptoms, such as Parkinson’s disease or other movement disorders.
A neurological exam is another important step. During this assessment, the physician evaluates reflexes, muscle strength, coordination, balance, eye movements, and cognitive abilities. They may ask you to perform specific tasks that test memory, concentration, and problem-solving skills. Subtle abnormalities in motor control or thinking patterns can provide important diagnostic clues.
If the clinical findings suggest Huntington’s disease but are not definitive, further testing may be recommended. Diagnostic imaging, such as a CT scan, can be used to examine the brain for structural changes. Imaging studies may reveal alterations in certain brain regions involved in movement and cognition. In many cases, genetic testing is ultimately used to confirm the diagnosis by identifying the specific gene mutation responsible for Huntington’s disease.
For individuals concerned about disease progression and long-term outlook, learning more about related topics such as Is Huntington’s disease fatal can provide additional clarity about what to expect and how to plan for the future.
Can Huntington’s disease be treated?
Huntington’s disease is a progressive condition that currently does not have a cure. While there is no way to stop or reverse the underlying genetic mutation, a variety of effective treatment strategies can help manage symptoms and improve daily functioning. Early intervention often plays a key role in maintaining independence and quality of life for as long as possible.
Treatment plans are typically personalized and may include medication to help alleviate specific symptoms, such as:
- vesicular monoamine transporter 2 (VMAT2) inhibitors, which can help treat involuntary movements
- antidepressants to help with any mood changes
VMAT2 inhibitors are commonly prescribed to reduce the severity of involuntary movements associated with Huntington’s disease. Antidepressants and other psychiatric medications may be recommended to address depression, anxiety, irritability, or mood instability. Managing emotional health is just as important as addressing physical symptoms, as mental well-being significantly influences overall quality of life.
In addition to medication, a multidisciplinary approach to care can be highly beneficial. There are several management options that can help to improve overall quality of life, such as:
- physical therapy, to help with mobility and balance
- speech therapy, to help with trouble speaking
- home modifications, such as installing handrails for support
- assistive devices, such as canes or a wheelchair, to help you move around more easily
Physical therapy focuses on maintaining strength, flexibility, and coordination. Regular guided exercises may reduce fall risk and promote safer movement. Speech therapy can address communication challenges and swallowing difficulties, helping to preserve independence and nutritional health. As mobility becomes more limited, assistive devices and adaptive home modifications can enhance safety and accessibility.

Lifestyle strategies may also support overall well-being. Maintaining a structured daily routine, engaging in appropriate physical activity, and ensuring adequate nutrition can make a meaningful difference. Emotional support from family, counseling services, and support groups may help individuals and caregivers cope with the psychological impact of the disease.
Because Huntington’s disease progresses over time, ongoing medical follow-up is essential. Healthcare providers can adjust treatments as symptoms change and provide guidance on long-term care planning. By understanding What is the first sign of Huntington’s disease and recognizing early warning signs, individuals at risk can seek timely evaluation, begin supportive therapies sooner, and make informed healthcare decisions.
Although the condition presents significant challenges, comprehensive symptom management and supportive care can help individuals live with greater comfort and dignity. Advances in research continue to explore new therapeutic approaches, offering hope for improved treatments in the future.




















Leave a Reply
You must be logged in to post a comment.