Delayed wound recovery and related complications are frequent among people with diabetes. Impaired circulation and nerve injury are key contributors to slower healing in those living with diabetes.
Foot sores are especially prevalent in people with diabetes. Slow healing can cause these sores to deteriorate or become infected, potentially resulting in tissue damage.
For this reason, regular self-examinations and vigilant monitoring of any wounds—particularly on the feet—are essential. Identifying and treating wounds early when you have diabetes may lower the likelihood of serious complications.
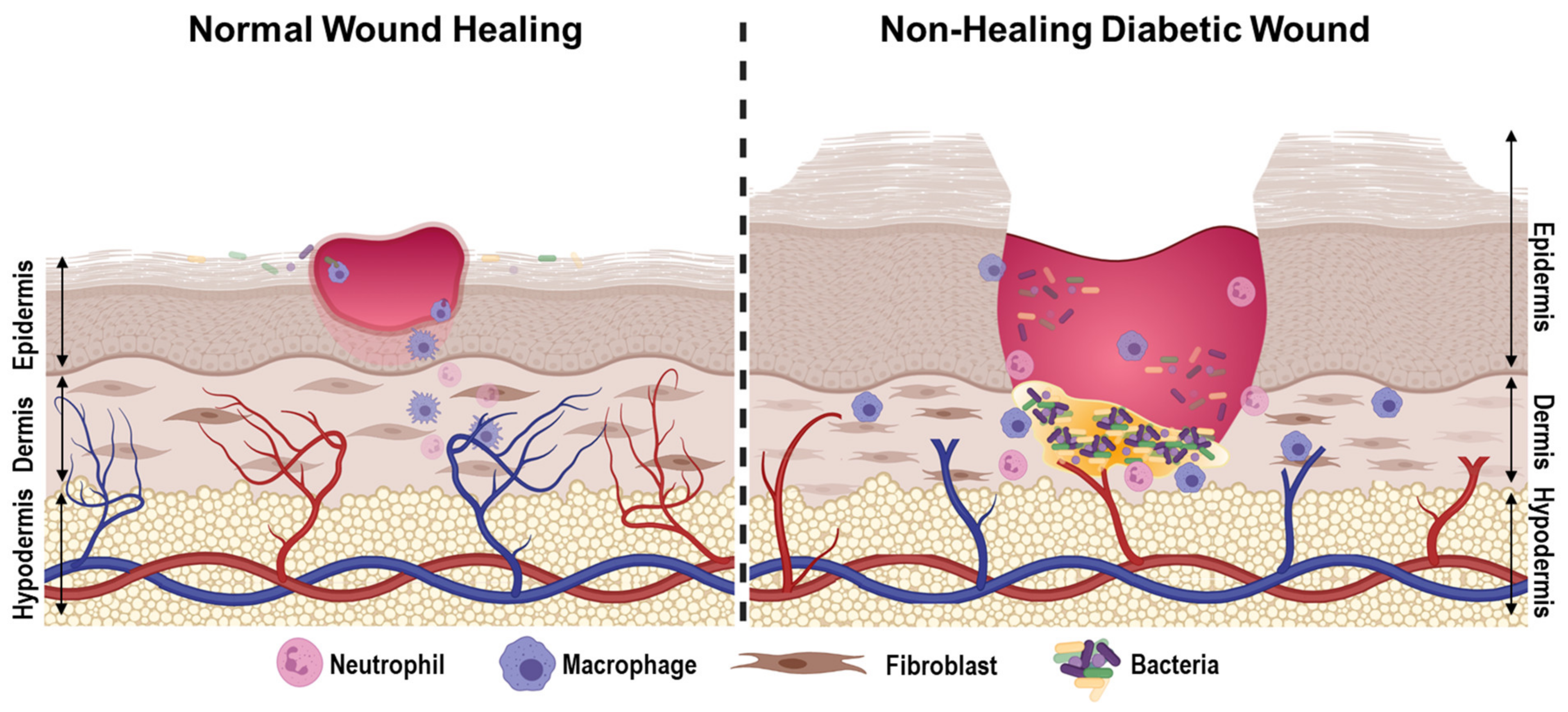
Why wounds take longer to heal in people with diabetes
Several factors related to diabetes can delay the wound repair process.
Decreased blood circulation
High blood glucose over time can damage blood vessels, causing them to thicken and stiffen. This often leads to poorer blood flow, especially to the extremities.
Reduced circulation means less delivery of oxygen and vital nutrients necessary for tissue repair.
Neuropathy
Persistently elevated blood sugar can also harm nerves, a condition known as neuropathy. Peripheral neuropathy, affecting the arms and legs, is common among people with diabetes.
Nerve damage reduces sensation, so you may not notice injuries as they occur or recognize when they are worsening. As a result, wounds can remain untreated for extended periods.
Weakened immune function
Diabetes can blunt the immune system’s responsiveness. If a wound becomes infected, the body may be less capable of mounting an effective defense.
Infection is a frequent complication of delayed healing.
High blood sugar also creates an environment that favors bacterial growth, which can make infections develop faster and become more severe.
Left unchecked, complicated infections can progress to gangrene or sepsis.
Higher levels of inflammation
Diabetes is linked with chronic inflammation and tissue damage from oxidative stress.
While short-term inflammation is a necessary part of healing, persistent inflammation can impair recovery. This is largely due to prolonged presence of inflammatory mediators (such as cytokines) and dysfunctional cellular activity that interferes with the repair process.
Possible consequences of untreated wounds
Open wounds that aren’t adequately observed can quickly escalate into more serious problems, including:
- Infections: Prolonged healing can allow bacteria to invade and multiply in the affected tissue.
- Ulcers: People with diabetes frequently develop foot ulcers, which may become infected and extend into deeper structures like muscle and bone.
- Amputation: If infections or ulcers advance, urgent surgery to remove the affected tissue may be necessary to stop further spread.
- Gangrene: Tissue can die (gangrene) when it lacks sufficient oxygen and nutrients. Dead tissue cannot repair itself and creates a favorable setting for infection and other complications, potentially leading to amputation.
- Sepsis: Slow-healing wounds in diabetes can allow a minor injury to become a large ulcer or severe infection. If superficial infections are not treated, they can evolve into more serious systemic infections, including bloodstream infection (sepsis), which is a medical emergency.
How to promote faster wound healing
The following measures may help lower the risk of complications associated with delayed wound healing in diabetes:
- Daily self-exams: Inspecting your body every day, especially your feet, can help you spot wounds early and prevent infections and complications. Remember to check between and under your toes.
- Control blood sugar: Monitoring and keeping your blood glucose within target ranges and adhering to your treatment plan is the best defense against problems related to slow healing.
- Appropriate wound care: If you discover a new wound, clean it and change dressings regularly. Seek medical attention if the wound does not improve within a few days, becomes swollen, produces pus, or causes pain.
- Avoid pressure on wounds: Tight clothing, restrictive bandages, or continued pressure on the injured area can hinder proper healing.
Takeaway
Slow wound healing is common in diabetes because chronic high blood sugar damages nerves and blood vessels. Untreated wounds can lead to infections, ulcers, and even amputation. Managing blood glucose, performing daily self-checks, and keeping wounds clean and properly cared for can help reduce the risks associated with delayed healing in diabetes.





















Leave a Reply
You must be logged in to post a comment.