Seeing blood in your vomit during pregnancy isn’t always an emergency, but it’s something you should bring up with your healthcare provider promptly.
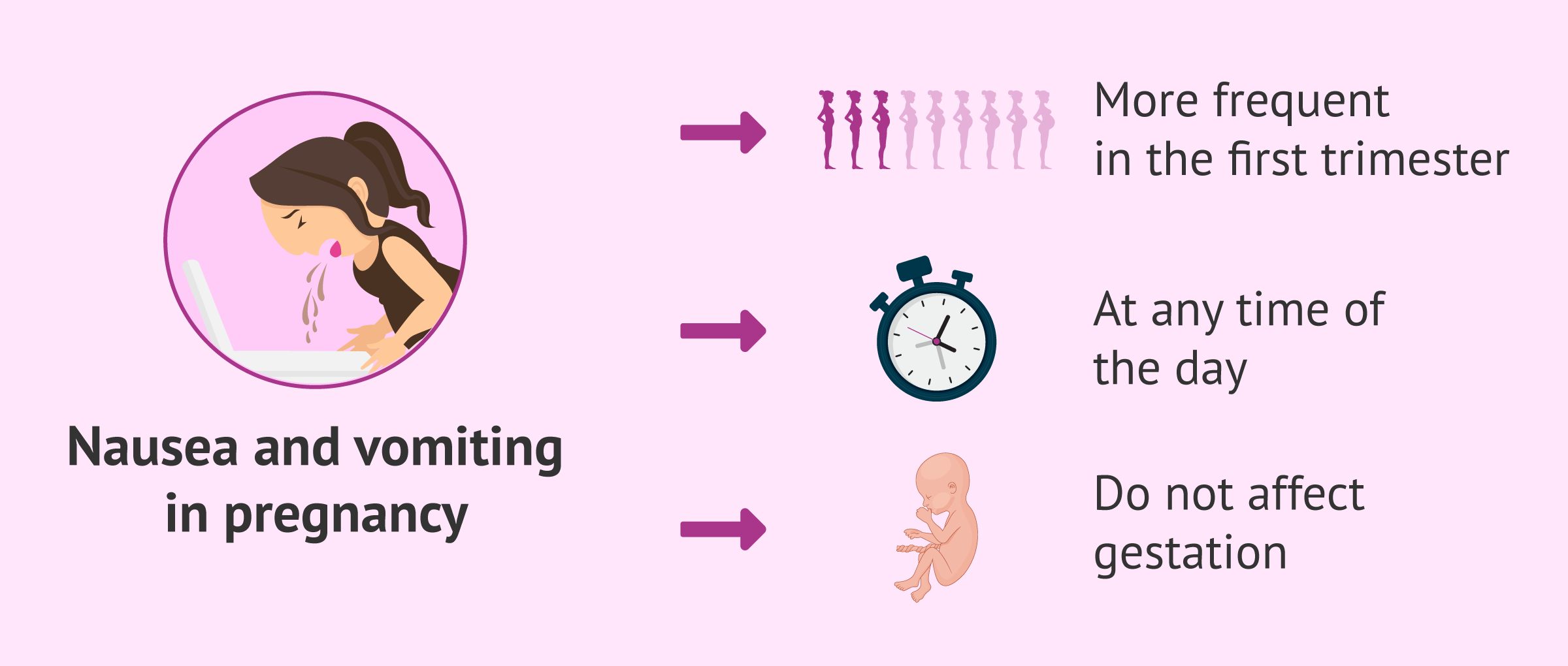
Nausea and vomiting are so frequent in pregnancy that some people first realize they’re expecting when they can’t keep down their breakfast anymore.
In fact, as many as 90 percent of pregnant people experience nausea and vomiting, typically in the first trimester. Fortunately, this so-called “morning sickness” (which can occur at any time of the day) usually improves by weeks 12 to 14.
You may be used to puking occasionally, but one day you notice a pinkish to brown tint in what you bring up — blood.
While vomiting blood during pregnancy (or at any time) isn’t ideal, it does occur. The medical term for it is hematemesis.
There are a number of common medical explanations for why you might vomit blood while pregnant. Many of these resolve on their own after the first trimester or after delivery, but all warrant discussion with your clinician.
Vomiting during pregnancy can be normal, but blood in vomit is not. Contact your doctor right away if you notice blood when you vomit.
When to contact your healthcare provider
The bottom line: contact your provider immediately if you observe blood in your vomit.
Some causes of blood in vomit originate in the upper digestive tract — the mouth, throat, esophagus (the tube connecting mouth to stomach), or stomach. Your clinician may examine your esophagus using an endoscopy.
Your provider may also order additional tests or imaging, such as:
- oxygen saturation checks
- bloodwork
- ultrasound
- MRI
- CT scan
- X-ray
Does vomiting blood indicate miscarriage?
Vomiting blood by itself is not an indicator of miscarriage. Your pregnancy is probably unaffected. However, if vomiting blood occurs together with other concerning signs, that could signal a problem.
Seek immediate medical care if you also experience:
- very severe nausea and vomiting
- intense abdominal cramping
- mild to severe lower back pain
- dizziness or lightheadedness
- a severe headache
- heavy vaginal spotting
- bleeding similar to a period
- vaginal fluid or tissue discharge
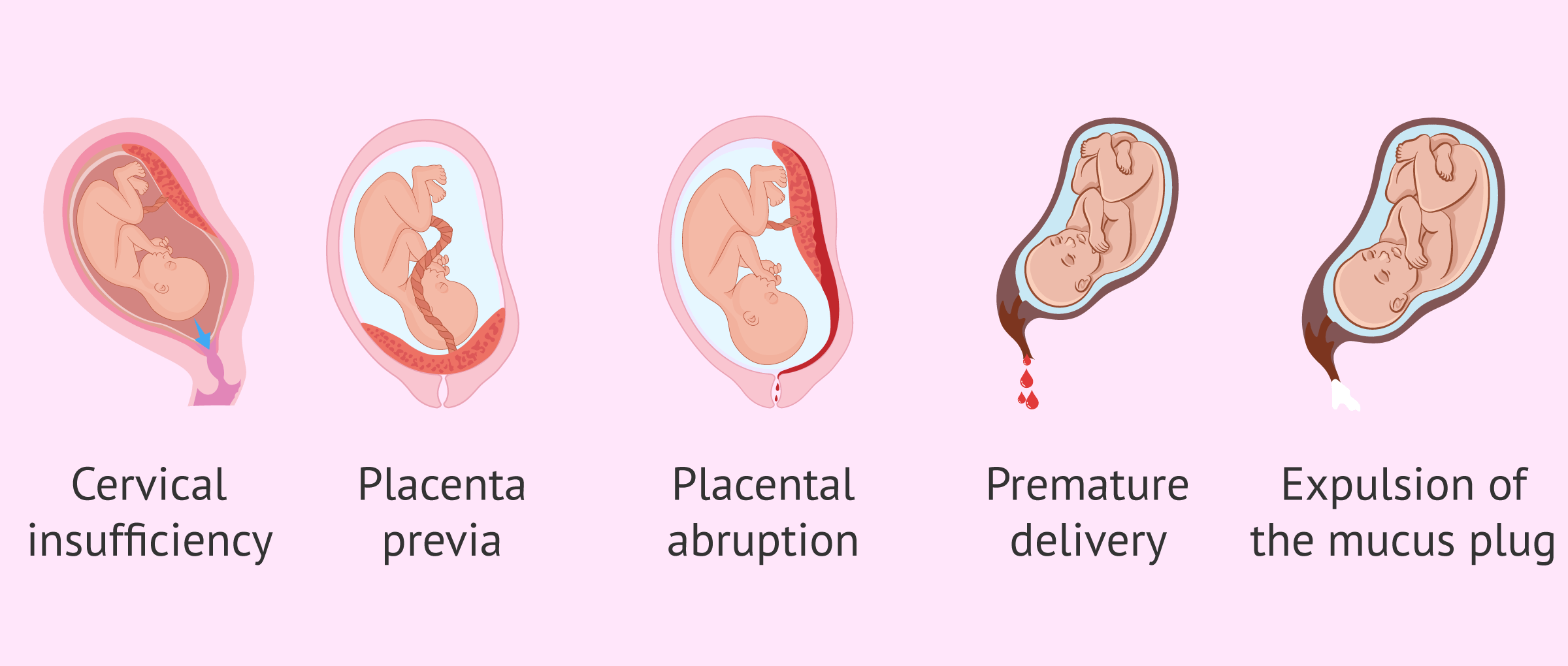
Common reasons for blood in vomit
Bleeding gums
Some pregnant people develop sore, swollen gums that bleed — often referred to as pregnancy gingivitis.
Hormonal changes in pregnancy increase blood flow to the gums, making them more prone to bleeding.
Other signs you might notice include:
- reddened gums
- puffy or swollen gums
- tender, inflamed gum tissue
- sensitivity when eating or drinking
- receding gums (teeth appear longer)
- bad breath

You might not always notice it, but frequent vomiting can further irritate already-sensitive gums, causing bleeding that then appears in vomit. Not an attractive combination.
Even with good dental hygiene, pregnancy gingivitis can occur. Brushing twice daily and flossing once a day can help protect your gums and reduce bleeding.
Nosebleeds
Pregnancy increases circulation throughout the body, including the nasal passages. This can cause tiny blood vessels in the nose to enlarge.
With greater blood flow and swollen vessels, you may be more likely to have nosebleeds while pregnant — even if you usually don’t get them.
If the bleed is toward the back of the nose or if you’re lying down, blood may run down the throat instead of out the nostrils and emerge when you vomit soon after.
Blood from a nosebleed may range from bright to dark red. A congested, stuffy nose is another common pregnancy symptom that may accompany it.
Irritation of the mouth or throat
If you notice small specks of blood or dark, dried blood in your vomit, the source may be your mouth or throat.
Frequent vomiting can inflame and irritate the lining at the back of the throat because vomit contains acidic stomach contents.
You’ve likely felt acid burn in your throat during bad heartburn episodes. That irritation can cause bleeding or crusting that’s expelled when you vomit again.
Your throat and mouth may also feel sore, raw, or swollen.
Esophageal irritation or tear
The esophagus runs from the throat to the stomach. Repeated vomiting can irritate the esophageal lining, producing small amounts of fresh or dried blood in vomit.
A more severe source is an esophageal tear. This is uncommon but serious and can occur during pregnancy. It’s a less frequent cause of bleeding with vomiting in the first trimester.
An esophageal tear results from excessive pressure within the stomach or esophagus. In rare instances it can occur in late pregnancy, possibly related to increased abdominal pressure and other health issues.
Other common causes of an esophageal tear include:
- heavy alcohol use
- bulimia
- a hiatal hernia
- high blood pressure
- preeclampsia
- intense coughing
- stomach infections
If you have an esophageal tear, you’ll likely see a lot of bright red blood in your vomit. Additional worrisome symptoms may include:
- dizziness or faintness
- difficulty breathing
- severe heartburn
- intense abdominal pain
- back pain
- excessive fatigue
- dark, tarry stools
Stomach ulcer
Stomach ulcers are open sores in the stomach lining. These can occasionally bleed, producing bright red or dark blood in vomit.
If you’ve had ulcers in the past, they might flare during pregnancy.
Ulcers often result from:
- infection with the bacterium H. pylori
- use of medications like aspirin or ibuprofen
- high stress levels
A stomach ulcer may worsen nausea and vomiting during pregnancy. You may also notice:
- abdominal discomfort
- heartburn
- frequent belching
- bloating
- feeling full quickly
- weight loss
Treatment options for vomiting blood in pregnancy
Treatment depends on the underlying cause of blood in your vomit.
If an ulcer is responsible, your clinician may prescribe antibiotics to eliminate an infection. Dietary changes and avoiding over-the-counter pain relievers like aspirin (unless advised by your OB-GYN) can also help.
Your provider might suggest medication to ease nausea and vomiting. Always check with your clinician before taking OTC remedies, as some anti-nausea drugs aren’t suitable during pregnancy.
More severe causes — for instance, an esophageal tear — may require medications and sometimes surgical repair.
Home approaches for nausea
Until your provider identifies the reason for blood in your vomit — which should be done immediately — avoid trying home remedies specifically for vomiting blood.
If you receive treatment for the cause but still suffer from significant morning sickness, talk to your clinician about safe options.
Keep in mind that “natural” remedies and herbs are active substances and can have strong effects. Some may increase heartburn or further irritate the stomach, potentially making the issue worse.
One well-studied home remedy for nausea is ginger. A 2016 review found ginger improved nausea and vomiting in pregnant people taking 250 mg four times daily.
Consider adding fresh ginger to tea, water, or juice. Ginger powder, syrup, juice, capsules, candied ginger, or dried ginger are other options.
Other natural strategies that may help nausea and vomiting include:
- vitamin B6 (often included in prenatal vitamins)
- peppermint
- certain fruit juices, such as cranberry or raspberry
Potential complications of vomiting blood while pregnant
Blood in vomit during pregnancy is usually more a concern for the pregnant person than the fetus, but it can pose risks to both. Tell your clinician about any amount of blood in vomit — don’t ignore it.
You may need no treatment, but when treatment is required, appropriate care can prevent complications.
Serious internal bleeding can lead to problems like excessive blood loss and shock. Warning signs that warrant immediate attention include:
- very severe nausea and vomiting
- rapid, shallow breathing
- dizziness or fainting
- blurred vision
- confusion
- cold, clammy skin
- reduced urine output
- dark stools or blood in stool
Key points
Finding blood in your vomit is unsettling, but several straightforward explanations exist.
Often, the act of retching and vomiting itself causes the bleeding. Other pregnancy-related changes can contribute as well.
Tell your provider if you vomit blood. A prompt evaluation is important to rule out other causes and to make sure you get appropriate care.
Treatment, when needed, can protect both your health and your baby’s. Addressing the underlying cause quickly helps keep you both safer and healthier.




















Leave a Reply
You must be logged in to post a comment.