Sacroiliac (SI) joint disorders may develop due to osteoarthritis, trauma, or other underlying medical conditions. These issues frequently result in either sharp, stabbing discomfort or a tingling sensation in the lower back and pelvis.
Sacroiliac joint pain is often described as a sudden, piercing ache that travels from the hips and pelvic region into the lower back and sometimes down the thighs. In certain cases, it may be accompanied by numbness, tingling, or a feeling as though the legs might give way. Because the SI joints connect the spine to the pelvis, irritation in this area can also mimic other types of lower back or hip pain.
Research indicates that the SI joints are responsible for 15 to 30 percent of chronic lower back pain cases. Given how common lower back discomfort is, this makes sacroiliac joint pain a significant yet sometimes overlooked contributor.
Approximately 80 percent of adults in the United States will experience lower back pain at some point in their lifetime. It remains one of the top reasons for missed work and is the most frequent cause of job-related disability. Understanding whether symptoms stem from the SI joint, lumbar spine, or hips is key to choosing the right treatment approach.
What is the SI joint?
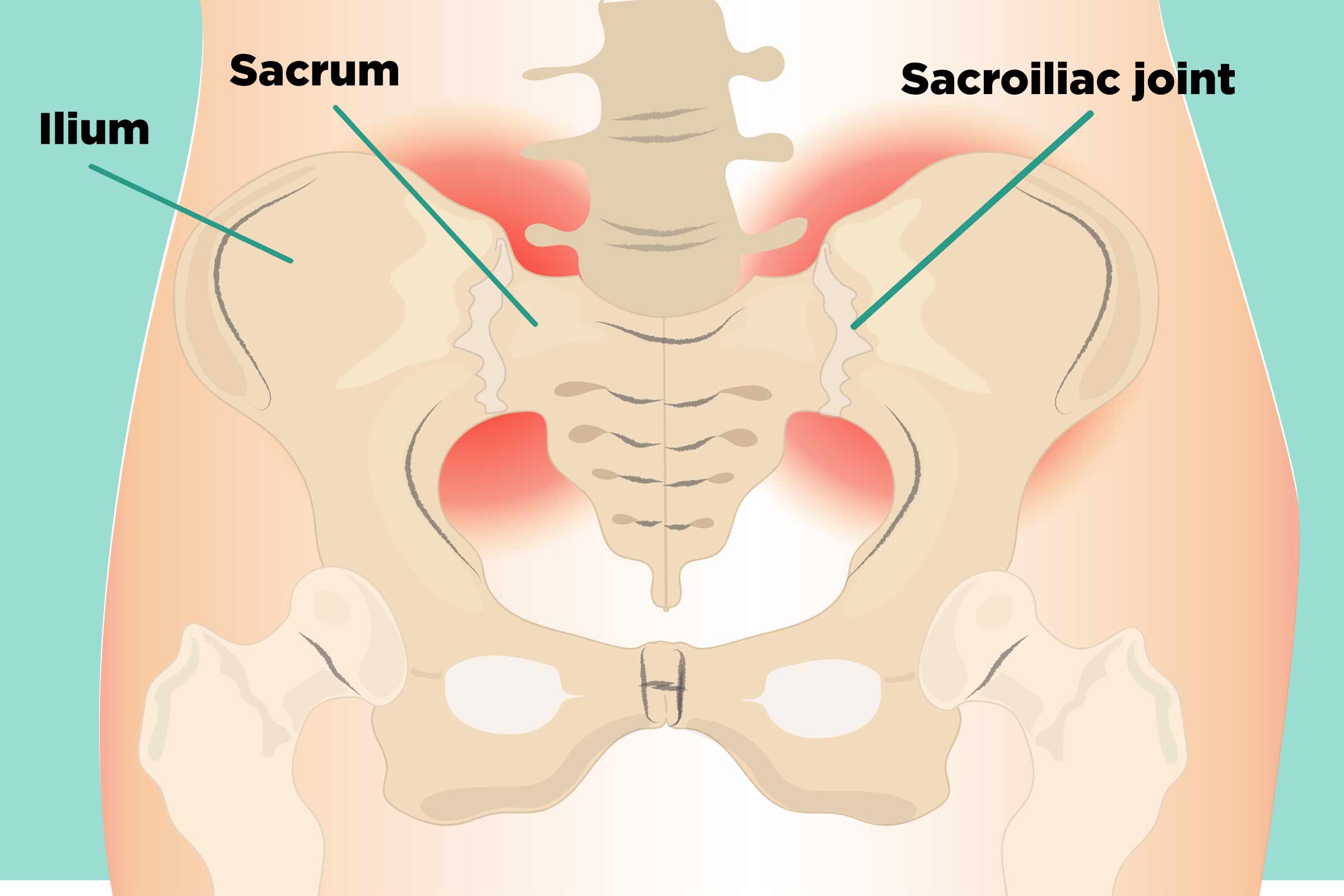
The sacroiliac joints are positioned in the lower back where the sacrum meets the ilium. The sacrum is the triangular bone at the base of the spine, located just above the coccyx (tailbone). The ilium is one of the three bones forming each hip bone and represents the uppermost portion of the pelvis.
These joints play a critical role in supporting body weight by transferring loads from the upper body to the pelvis and legs. They function as shock absorbers, minimizing the impact and stress placed on the spine during activities such as walking, bending, and lifting.

The surfaces of the SI joint bones are irregular and interlock similarly to puzzle pieces, which helps maintain proper alignment. Strong ligaments and surrounding muscles reinforce these joints, offering stability while still permitting a small but essential range of motion. Although movement is limited, it is crucial for maintaining balance, upright posture, and facilitating childbirth.
The joint surfaces are coated with cartilage, a smooth protective tissue that reduces friction. The space within the SI joints contains fluid that provides lubrication for smoother motion. Numerous nerve endings in this region transmit pain signals to the brain when inflammation, misalignment, or cartilage breakdown occurs.
If the bones of the SI joint shift out of alignment or if cartilage deteriorates to the point that bone rubs against bone, significant discomfort can result.
What causes SI joint pain?
Inflammation affecting one or both SI joints is known as sacroiliac joint dysfunction or sacroiliitis. Several medical conditions and mechanical factors can contribute to sacroiliac joint pain.
Osteoarthritis
Over time, repeated stress and wear on the joints can erode cartilage, leading to osteoarthritis. Commonly associated with aging, osteoarthritis may impact the SI joints, spine, hips, and other joints throughout the body. As cartilage thins, stiffness and pain often become more noticeable during movement.
Ankylosing spondylitis
Ankylosing spondylitis (AS) is an autoimmune disease that triggers a form of inflammatory arthritis primarily affecting the vertebrae and spinal joints. Beyond pain and stiffness, advanced AS may stimulate new bone formation that causes spinal joints to fuse.
Although AS most frequently targets the SI joints in its early stages, it can also inflame other joints and, in rare instances, organs and eyes. AS is a chronic condition characterized by flare-ups of mild to severe pain. It is diagnosed most frequently in young men.
Gout
Gout, or gouty arthritis, develops when uric acid accumulates in the body. This condition is marked by sudden, intense joint pain. While gout typically begins in the big toe, it can affect any joint, including the SI joint, leading to episodes of severe inflammation.
Injury
Traumatic events such as falls, sports injuries, or motor vehicle accidents can damage the SI joints. Even minor repetitive strain over time may destabilize the joint and provoke ongoing pain.
Pregnancy
During pregnancy, the hormone relaxin is released, increasing ligament flexibility and making the SI joints more elastic. This natural change allows the pelvis to widen for childbirth but can also reduce joint stability.
Additional weight gain and altered posture during pregnancy place extra strain on the pelvis and lower back. As a result, some pregnant individuals develop sacroiliac joint pain. Repeated pregnancies may elevate the risk of arthritis in the SI joints.
Walking patterns
Abnormal gait patterns can contribute to SI joint dysfunction. Causes may include leg length discrepancy, fused knee joints, or problems involving the hip or ankle. Favoring one leg due to pain can also disrupt normal biomechanics. Identifying and correcting these mechanical issues often improves symptoms. Reviewing resources such as a Hip pain location diagram female can help individuals better understand how pelvic and hip alignment influences discomfort.
Some pregnant individuals temporarily adopt an altered walking pattern. After delivery, once normal gait mechanics return, sacroiliac joint pain may subside.
Preventing SI joint pain
Not all instances of sacroiliac joint pain can be prevented, particularly when linked to chronic inflammatory diseases.
However, maintaining flexibility, engaging in regular low-impact physical activity, and supporting joint health through strength training may help slow symptom progression. Core stabilization exercises and proper posture are especially important for reducing stress on the lower back and pelvis.
Keeping body weight within a comfortable and healthy range can significantly reduce strain on the SI joints and lower spine, lowering the risk of degenerative changes over time.
Symptoms of SI joint pain
Symptoms vary from person to person, but common signs of sacroiliac joint disorders include:
- lower back pain
- pain in the buttocks, hips, or pelvis
- groin discomfort
- pain localized to one SI joint
- worsening pain when standing from a seated position
- pelvic stiffness or a burning sensation
- numbness
- weakness
- pain radiating into the thighs or upper legs
- a sensation that the legs may buckle
Because these symptoms overlap with conditions such as sciatica or hip arthritis, a thorough medical evaluation is important for accurate diagnosis.
Diagnosing SI joint problems
Diagnosing SI joint dysfunction can be challenging because the joints lie deep within the body, making physical examination and motion testing more difficult. Additionally, joint abnormalities may not always appear clearly on imaging studies like X-rays, MRIs, or CT scans.
The symptoms of an inflamed SI joint closely resemble those seen in sciatica, bulging discs, or hip arthritis, which can complicate diagnosis.
To identify the source of pain, your doctor may use several methods:
- Physical examination. You may be asked to perform specific movements or stretches to determine which positions reproduce pain.
- Numbing drugs. If injecting a numbing medication such as lidocaine into the SI joint temporarily relieves pain, this strongly suggests the SI joint as the source.
- Imaging tests. X-rays, MRIs, and CT scans may help rule out other causes of lower back or pelvic pain.
Optum Now is operated by RVO Health. By clicking on this link, we may receive a commission. Learn more.
Treatment
Therapy, exercise, and self-care
Physical therapy is often a first-line treatment for sacroiliac joint pain. Targeted exercises strengthen supporting muscles, enhance joint stability, and improve mobility. Low-impact activities such as yoga can increase flexibility without placing excessive strain on the joints.
Massage therapy may also reduce muscle tension surrounding the pelvis and lower back. Applying cold packs during acute flare-ups can help decrease inflammation, while heat therapy—using a heating pad, heat wrap, or warm bath—can relax tight muscles and relieve stiffness.
A sacroiliac belt may provide additional external support, limiting excessive motion and reducing discomfort during daily activities.
Medication and nonsurgical therapies
If conservative approaches do not adequately control symptoms, or if pain stems from chronic conditions like AS, your doctor may suggest medications or minimally invasive procedures, including:
- anti-inflammatory medications, including nonsteroidal, anti-inflammatory drugs (NSAIDs) such as aspirin, ibuprofen, and naproxen
- muscle relaxants
- oral steroids, for short-term use only
- tumor necrosis factor inhibitors (TNF inhibitors) to treat AS
- corticosteroid injections into the joint
- radiofrequency ablation, which uses energy to deactivate the nerves responsible for transmitting pain
Surgery
Surgery is generally considered a last option when other treatments fail. Sacroiliac joint fusion surgery involves placing small plates and screws to stabilize the joint, encouraging the bones to fuse together.
This procedure may be recommended for persistent, severe pain that does not improve with physical therapy, medications, or other minimally invasive interventions. While SI joint fusion can effectively reduce pain, it slightly limits joint mobility.
Outlook
Sacroiliac joint pain may be temporary, particularly when associated with pregnancy, minor injury, or short-term strain. In chronic conditions such as AS or osteoarthritis, symptoms may fluctuate with periods of improvement and flare-ups.
With appropriate diagnosis and a comprehensive treatment plan, most individuals experience substantial pain relief and improved function, allowing them to return to daily activities with greater comfort and stability.






















Leave a Reply
You must be logged in to post a comment.