You might notice mucus in your bowel movement after eating certain foods. However, poop that appears persistently frothy can signal that your body is not absorbing fat properly. In some cases, this may also present as Hard poop With white mucus, which can point to irritation or an underlying digestive concern.
From time to time, experiencing foam or bubbles in your stool is harmless and often linked to something you recently consumed. Once that food is eliminated, the issue typically resolves. But if foamy stool or Hard poop With white mucus happens frequently or is accompanied by other digestive symptoms, it may indicate a more significant gastrointestinal condition that needs evaluation.
Doctors often rely on tools like the Bristol Stool Chart to classify stool types and better understand what variations may reveal about digestive health.

Below, we explore the potential reasons for foamy bowel movements, what excessive mucus could mean, and when to consult a healthcare professional.
What causes foamy poop?
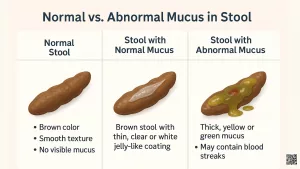
Stool may look foamy when there is an excess of fat or mucus present.
Mucus sometimes resembles foam or appears mixed within it. A small amount of mucus is completely normal—it lubricates the intestines and supports smooth passage of feces. However, increased mucus production, particularly alongside Hard poop With white mucus, may occur in certain digestive disorders. If you’re unsure what abnormal mucus looks like, reviewing examples such as White mucus in stool photos can provide helpful visual guidance.
When fat is not absorbed correctly, a condition called steatorrhea—also known as fatty stool—can develop. Instead of being properly digested and absorbed in the intestines, fats remain in the stool. Other signs of fat malabsorption include:
- oily stool
- pale or clay-colored stool
- bulky, foul-smelling stool
- floating stool
Steatorrhea may result from digestive conditions such as:
- certain diet medications
- cystic fibrosis
- pancreatitis
If your symptoms stem from a specific dietary trigger, they often improve after removing that item from your meals. Persistent or recurring symptoms, however, may suggest an underlying medical issue.
Conditions linked to foamy stool include the following:
1. Celiac disease
Celiac disease is a digestive disorder triggered by an immune reaction. When individuals with celiac disease consume gluten, their immune system attacks and damages the lining of the small intestine. This damage interferes with nutrient absorption and can lead to fat malabsorption and foamy stool.
What is gluten?
Gluten refers to a group of proteins found in wheat, rye, and barley. It is also added to some processed foods to enhance texture and retain moisture.
Celiac disease often runs in families. According to the Celiac Disease Foundation, 1 in 100 people worldwide are affected, though many remain undiagnosed.
There are more than 250 symptoms associated with celiac disease. Manifestations vary significantly between adults and children.
Common symptoms in adults include:
- abdominal pain
- bloating, gas, constipation, and diarrhea
- nausea and vomiting
- depression and anxiety
- brain fog
- fatigue
- headaches or migraine
- iron-deficiency anemia
- itchy skin rash
- joint pain
- missed periods
- mouth sores
- osteoporosis
- tingling in the hands and feet
- weight loss
Common symptoms in children include:
- abdominal pain
- bloating, gas, constipation, and diarrhea
- nausea and vomiting
- depression and anxiety
- attention deficit hyperactivity disorder (ADHD)
- learning disabilities
- tooth enamel erosion
- delayed puberty
- being undernourished
- fatigue
- headaches
- iron-deficiency anemia
- irritability
- pale, foul-smelling stools
- seizures and lack of muscle coordination
- short height
- weight loss
Diagnosis typically involves blood testing followed by a biopsy of the small intestine.
Treatment requires strict, lifelong elimination of gluten. Without management, celiac disease can contribute to long-term complications, including persistent digestive symptoms such as Hard poop With white mucus.
2. Irritable bowel syndrome
Irritable bowel syndrome (IBS) is a functional gastrointestinal disorder. Although no structural abnormalities are present, bowel function is altered. IBS is categorized into four subtypes based on stool consistency.
Approximately 10% to 15% of people are affected by IBS, and it occurs more frequently in people assigned female at birth than in people assigned male at birth.
The precise cause remains unclear, but experts believe genetic predisposition and environmental influences both play roles. These factors may impact how quickly stool moves through the digestive tract and how the brain and gut communicate.
IBS symptoms may include:
- abdominal cramping and pain
- diarrhea or constipation
- bloating
- gas and belching
- fatigue
- white mucus in the stool
- an urgent need to have a bowel movement
Some individuals with IBS report Hard poop With white mucus, particularly in constipation-predominant cases. While mucus alone does not confirm a serious condition, persistent changes should be evaluated. In rare cases, mucus may also be associated with more serious illnesses—educational resources such as Colon cancer pictures of mucus in stool can help patients understand warning signs, though a medical diagnosis is essential.
Management strategies for IBS often focus on diet and lifestyle adjustments, including:
- increasing fiber intake gradually
- following a low FODMAP diet
- avoiding gluten if sensitive
- limiting gas-producing foods such as cabbage, carbonated beverages, and beans
A doctor may also recommend:
- medications for constipation or diarrhea
- laxatives
- antispasmodic drugs, antidepressants, or peppermint oil capsules for abdominal discomfort
3. Giardiasis
Giardia lamblia is a microscopic parasite responsible for infecting the small intestine, leading to giardiasis.
Infection occurs by drinking contaminated water, consuming uncooked contaminated food, swimming in infected water, or through person-to-person (or pet-to-person) transmission via contact with infected feces.
Symptoms of giardiasis include:
- abdominal cramps
- foul-smelling diarrhea or greasy stool
- nausea
- fever
- headache
- loss of appetite
Most cases resolve without treatment within approximately 4 weeks. Staying well hydrated is important to avoid dehydration.
If symptoms persist, a stool test can confirm the infection, and an antibiotic may be prescribed.
4. Pancreatitis
Pancreatitis refers to inflammation of the pancreas. The pancreas produces enzymes necessary for digestion and regulates blood sugar levels. In pancreatitis, digestive enzymes activate prematurely and begin damaging pancreatic tissue.
The condition may be acute, resolving within days, or chronic, requiring long-term management.
Both forms often necessitate hospitalization. Treatment may involve fasting under medical supervision or surgery. Chronic pancreatitis frequently leads to fat malabsorption and steatorrhea.
People between the ages of 30 and 40 face a higher risk of developing acute or chronic pancreatitis, and it is more common in people assigned male at birth.
According to Most cases, acute pancreatitis typically results from gallstones. Chronic pancreatitis may develop due to:
- heavy alcohol use
- smoking cigarettes
- genetic disorders of the pancreas
Symptoms may include:
- nausea
- vomiting
- diarrhea
- steatorrhea or fatty stool
- upper abdominal pain radiating to the back or worsening after meals
- weight loss
Getting help
If foamy stool continues for more than a few days, consider consulting a doctor.
Diagnostic tests will depend on your medical history and specific symptoms.
Seek prompt medical attention if you experience:
- mucus or blood in your stool
- diarrhea lasting more than 2 days (or 24 hours in a child)
- a fever of 101.5˚F (38.6˚C) or higher, or 100.4˚F (3˚C) in a child
- sudden or ongoing abdominal pain
Outlook for foamy poop
In many instances, foamy stool improves within several days, especially when related to diet.
If symptoms persist or you notice warning signs such as blood or excessive mucus—particularly Hard poop With white mucus—medical evaluation is important. An underlying digestive disorder may require treatment to prevent complications.
Takeaway
Foamy stool can occasionally result from dietary choices and resolve on its own. However, frequent episodes, especially when combined with pain, persistent digestive changes, or Hard poop With white mucus, may signal an underlying condition that warrants professional assessment.





















Leave a Reply
You must be logged in to post a comment.