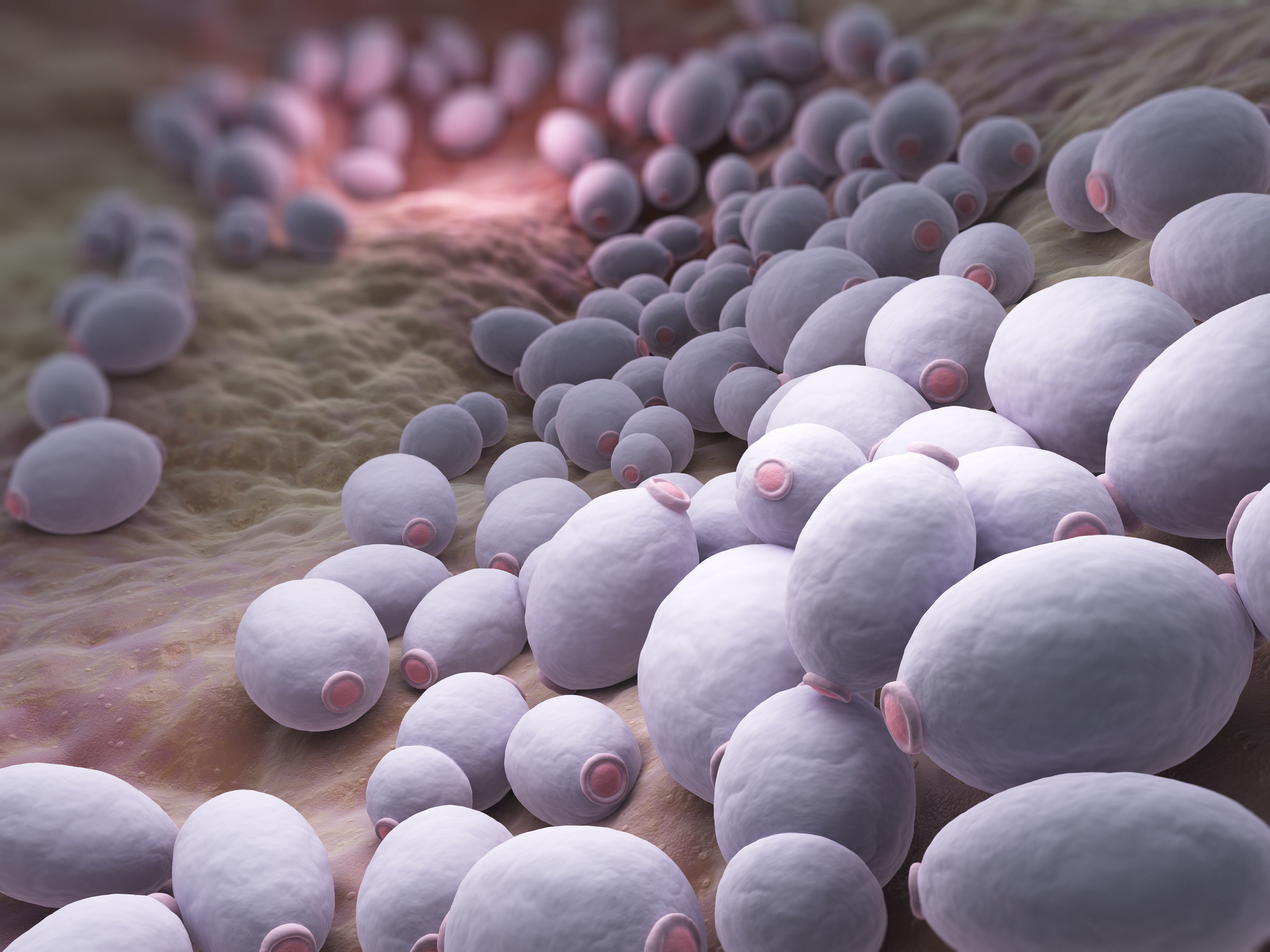
Candida is a group of yeasts that normally live in the intestines, on the skin, and on mucous membranes. Most people host some level of Candida throughout their bodies, and it is generally harmless.
When Candida multiplies excessively, it can cause an infection called candidiasis. The mouth and vagina are the most frequent sites for candidiasis. Overgrowth can also happen in the intestines, which may result in visible Candida in your stool.
What are the symptoms?
Signs of candidiasis vary by the area affected. When it occurs in the mouth, it’s known as thrush and produces white, cottage-cheese-like patches on the tongue or inner cheeks. It can also cause soreness or a burning sensation and may spread to other regions of the mouth or throat.
Vaginal candidiasis, often referred to as a yeast infection, leads to itching, unusual discharge, and discomfort during intercourse or urination.
If Candida overgrows in the intestines, symptoms may include bloating and increased cravings for sweets.
Q:
A:
What causes it?
Inflammation in the gastrointestinal (GI) tract
Conditions that cause inflammation in the GI tract, like Crohn’s disease and ulcerative colitis (forms of inflammatory bowel disease, or IBD), can alter the intestinal environment and have been linked to elevated levels of Candida in the gut.
Other IBD symptoms may include:
- diarrhea
- fatigue
- fever
- unintentional weight loss
- abdominal cramping and pain
- blood in the stool
Proton pump inhibitor use
Proton pump inhibitors (PPIs), commonly prescribed for acid reflux, lower stomach acid. This shift in acidity can change the intestinal environment and create conditions that favor Candida growth.
Antibiotics
Use of antibiotics, particularly broad-spectrum types, can encourage fungal proliferation. Antibiotics may eradicate beneficial bacteria that normally compete with yeast for space and nutrients. While you’re taking antibiotics you might notice Candida in your stool, though your microbial balance usually recovers after the medication stops.
Conditions that result in a compromised immune system
A weakened immune system can allow Candida to grow unchecked because a healthy immune response typically keeps naturally occurring fungus under control. Candida is commonly seen in people living with advanced HIV (AIDS) who experience diarrhea.
A normal gut environment
Candida is a typical element of a healthy intestinal ecosystem. Most of the time you won’t notice it in your stool, though occasional presence can happen even without overgrowth.
How is it diagnosed?
To check for Candida in stool, a clinician will collect a stool sample and inspect it under a microscope for yeast. They may also culture a small portion of the sample for several days to allow any yeast to grow and then identify the specific organism.
Because many healthy individuals have Candida in their gut, stool testing isn’t always definitive. Based on your symptoms, your provider might sample other affected areas or draw blood to test for Candida. For mouth or genital infections, clinicians can often diagnose candidiasis by visual examination.
How is it treated?
Antifungal medications can treat Candida. Fluconazole is a commonly used antifungal that can be taken orally to address Candida in the stool.
If an underlying issue such as IBD is contributing to intestinal Candida, that condition will be managed as well. Discuss your symptoms with your doctor to determine the most appropriate therapy. Typical IBD treatments include anti-inflammatory and immunosuppressive medications.
If medicines like PPIs or antibiotics are causing Candida in your stool, consult your doctor about the safest approach to reduce or stop the medication.
Are there ways to prevent this?
Although genetics and medical conditions can influence gut health, there are steps you can take to support a healthy intestine. These include:
- Use antibiotics only when necessary. Antibiotics can harm beneficial gut bacteria and permit Candida to flourish. Take antibiotics only when prescribed and required.
- Maintain a nutritious diet. Eating whole grains and fiber-rich foods like beans and apples supports gut health. Increasing the diversity of gut bacteria by consuming a varied, healthy diet helps maintain a balanced intestinal environment. Consider also guidance on the candida diet when relevant.
- Consider probiotics.Probiotics are supplements that contain live microorganisms, usually beneficial bacteria. Evidence varies, but some studies indicate probiotics may help maintain bacterial balance in the gut. Talk with your clinician about whether a probiotic could be appropriate for you.
- Include fermented foods.Fermented foods like sauerkraut, kimchi, and yogurt are rich in microbes that can promote gut health.
- Choose prebiotic foods.Prebiotics feed beneficial gut bacteria. High-fiber and complex-carbohydrate foods—fruits, vegetables, and whole grains—are excellent prebiotic sources.
What’s the outlook?
Candida in stool is treatable with antifungals, so consult your healthcare provider if you notice symptoms. Underlying causes can also be addressed. In most cases, Candida overgrowth does not lead to long-term harmful effects when properly treated.























Leave a Reply
You must be logged in to post a comment.