Several medical conditions can lead to an unpleasant odor inside your nose, including nasal polyps, sinus infection, and postnasal drip. In some cases, people describe the sensation as Smelling blood in nose and headache, which may be linked to sinus pressure, infection, or inflammation. A doctor can evaluate your symptoms, determine the cause, and suggest the most appropriate treatment plan.

Nearly every day, outside odors enter your nostrils. But what if the unpleasant smell seems to come from inside your nose instead?
Various health issues can create a rotten or metallic odor sensation in the nasal passages. While experiencing Smelling blood in nose and headache can feel alarming, most of these smells are temporary and typically do not signal a life-threatening condition.
That said, persistent symptoms, worsening pain, or associated concerns like facial pressure may require evaluation by a healthcare professional to properly assess your sinuses and throat.
Read on to explore the potential causes of a bad smell in the nose and what you can do about it.
Nasal polyps
Nasal polyps are soft, teardrop-shaped, noncancerous growths that can develop along the lining of your nasal cavity or sinuses. They often arise due to long-term inflammation.
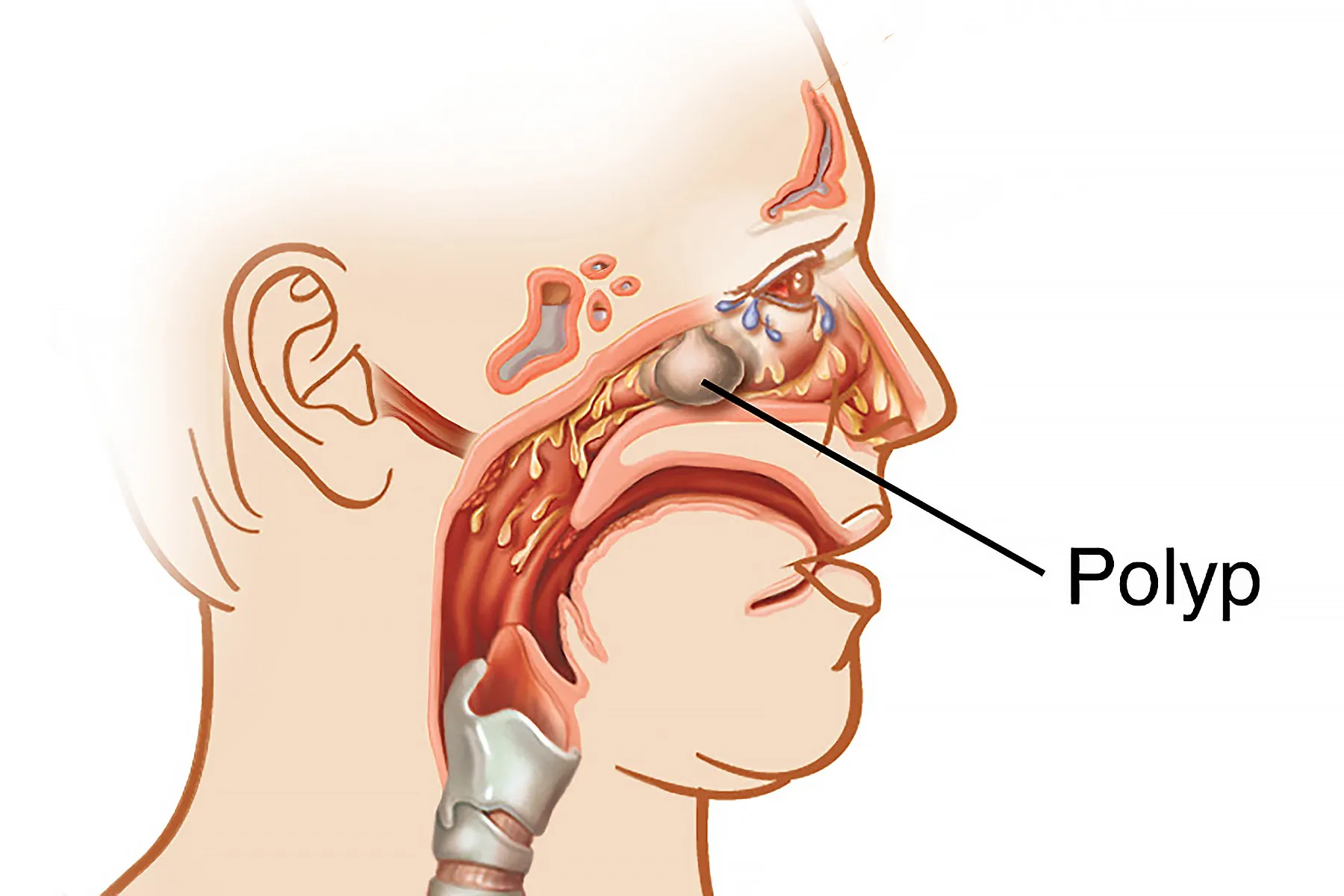
In some cases, fluid can accumulate within these growths, producing a foul or rotten smell. This fluid originates from the moist lining of your mucous membranes. The inflammation and blockage may also contribute to sinus pressure, which can be associated with Smelling blood in nose and headache in certain individuals.
Other, more common symptoms of nasal polyps may include:
- reduced sense of smell and taste
- runny nose
- nasal congestion
- headache
- pressure in the forehead and face
- snoring
Nasal polyps are frequently small, so you may not realize they are present. However, larger polyps or clusters of smaller ones can obstruct nasal airflow.
Treatment options for nasal polyps often involve corticosteroid nasal sprays or drops, such as fluticasone (Flonase) and mometasone (Nasonex).
If these treatments don’t provide relief, a doctor may prescribe oral corticosteroids like prednisone for up to 2 weeks. In more severe situations, endoscopic sinus surgery might be recommended.
Managing contributing factors—such as allergies, asthma, or chronic infections—is also essential to prevent recurrence.
Sinus infection
Sinus infections, also called sinusitis, may be caused by viruses, bacteria, or fungi. Inflammation of the sinus cavities can lead to thick mucus buildup and pressure.

Symptoms of sinusitis may include:
- yellow or green nasal discharge
- nasal congestion
- swelling, pain, and tenderness around your cheeks, forehead, and eyes
- headache
- fever
- tooth pain
- loss of smell
- bad breath
A buildup of mucus can sometimes produce a rotten or metallic odor. Some people interpret this as Smelling blood in nose and headache, especially when sinus pressure is significant. If you’re curious about odor perception, you can learn more about What does blood smell like in your nose and how sinus conditions may influence it.
Treatment depends on whether the sinusitis is acute or chronic and what organism is responsible.
Acute sinusitis may improve with OTC nasal sprays, saline irrigation, hydration, and rest. In some cases, antibiotics are prescribed for bacterial infections. Chronic sinusitis may require prescription steroid nasal sprays or antihistamines.
Occasionally, sinus surgery is necessary to restore proper drainage and ventilation.
Postnasal drip
Foul-smelling mucus in the nose—especially when it thickens and continually trickles down the back of the throat—may indicate postnasal drip.
Under normal circumstances, mucus helps:
- maintain healthy nasal membranes
- fight infections
- humidify inhaled air
- trap foreign particles
Typically, mucus blends with saliva and is swallowed without you noticing.
However, a cold, flu, allergies, or sinus infection may cause mucus to thicken, interfering with its usual drainage.
Postnasal drip may start gradually, with symptoms of coughing, sore throat, and frequent swallowing. Occasionally, one nostril may produce foul-smelling discharge. Some individuals describe this sensation as Smelling blood in nose and headache, particularly when congestion and sinus pressure are also present.
If postnasal drip continues longer than 3 weeks or the mucus becomes yellow, green, or grey, consult a healthcare professional.
Treatment strategies may include a combination of:
- increasing fluid intake
- sleeping with your head elevated
- using steam inhalation
- taking decongestants
- applying saline nasal spray
- running a humidifier
If these approaches are ineffective, a doctor may suggest additional therapies depending on the root cause, including:
- antihistamines for allergies
- cortisone steroid nasal spray to ease inflammation
- antibiotics for bacterial infection
Tooth decay
Tooth decay develops when bacteria accumulate on a tooth and gradually erode its surface. This bacterial growth can result in bad breath and odors that may seem to travel into the nasal passages.
Maintaining proper oral hygiene—brushing twice daily and flossing regularly—is one of the most effective ways to prevent cavities and gum disease.
If a dentist diagnoses a cavity or another condition such as periodontitis (gum disease), seeking timely treatment can help eliminate odor and prevent complications.
Tonsil stones
Your tonsils contain small crevices where debris such as:
- saliva
- mucus
- food particles
- dead cells
can become trapped.
Over time, this material may harden into small formations known as tonsil stones. Bacteria can feed on these stones, sometimes generating unpleasant odors in both the mouth and nose.
Risk factors include poor oral hygiene and enlarged tonsils, though tonsil stones can occur even in individuals with good dental care habits.
Treatment options include:
- gargling with salt water
- gently flushing the tonsils using a water pick
- tonsillectomy
Phantosmia
Phantosmia is an olfactory hallucination in which you detect smells that are not actually present. You may believe the odor originates in your nose or nearby environment.
This condition can develop after a respiratory infection or head injury. Disorders such as Parkinson’s disease, brain tumors, or inflamed sinuses may also trigger phantom smells. Some people experiencing phantosmia report metallic odors and may wonder, Why do I smell blood in my nose when there is none.
For certain individuals, phantosmia resolves without intervention. In others, addressing the underlying cause may reduce or eliminate the abnormal smell perception.
Chronic kidney disease
Chronic kidney disease (CKD) involves a gradual decline in kidney function over time.
Your kidneys filter waste from the bloodstream, which is then removed through urine. When kidney function decreases significantly, waste products can accumulate.
This buildup may produce an ammonia-like smell noticeable on the breath and in the mouth. Some individuals also detect a similar odor in the back of the nose.
This typically occurs only when CKD has progressed to stage 4 or stage 5.
At that stage, additional symptoms such as kidney pain, changes in urine color, and fatigue are usually present. A new ammonia-like odor is unlikely to be the first indication of kidney disease.
COVID-19-related parosmia
Loss of smell is a recognized symptom of COVID-19.
However, authors of a 2022 article report that some individuals experience distorted smell perception, known as parosmia.
Examples include food smelling rotten or sensing cigarette smoke when no one has been smoking. In some instances, these altered smells may be described as metallic or similar to Smelling blood in nose and headache.
This condition can progressively worsen and significantly affect appetite and nutrition. For example, perceiving food as spoiled may cause someone to eat far less than usual.
COVID-19-related parosmia may appear 3 months after the initial infection. It may result from changes occurring as damaged olfactory receptors regenerate.
There is no single established treatment, but a healthcare professional may recommend olfactory training therapy to help retrain the sense of smell.
When to see a doctor
Consult a healthcare professional if:
- the unpleasant smell inside your nose persists for more than 1 week
- you repeatedly experience foul nasal odors
- you notice additional symptoms such as facial swelling, nasal blockage, blurred vision, or headache
If you do not have a primary care doctor, the HealthEH FindCare tool at healtheh.com can help you locate physicians in your area.
Frequently asked questions
How do I get rid of the rotten smell in my nose?
Managing a rotten odor in the nose depends on the underlying cause. Treatment may involve home remedies such as steam inhalation, OTC nasal sprays, prescription medications, or, in uncommon cases, surgery.
Why do I smell something dead in my nose?
An unpleasant smell inside the nose can result from conditions like sinusitis, nasal polyps, or tooth decay. A healthcare professional can provide an accurate diagnosis and appropriate treatment recommendations.
Can a sinus infection smell like poop?
A sinus infection may cause mucus accumulation that blocks the nasal passages. Without proper treatment, bacterial growth may lead to a foul odor that some people describe as resembling poop.
What does a nose infection smell like?
A nose infection may not always produce a noticeable odor because congestion can reduce your sense of smell. However, mucus buildup can sometimes create an unpleasant scent.
Takeaway
An unpleasant smell within your nose can have many possible causes, ranging from sinus inflammation to dental issues. While experiencing Smelling blood in nose and headache can be concerning, most causes are manageable with home care or appropriate medical treatment.
If you frequently experience sinus infections or recurring nasal symptoms, these episodes may happen more than once.
Discuss preventive strategies with a healthcare professional to reduce your risk of ongoing nasal and throat problems in the future.

















Leave a Reply
You must be logged in to post a comment.