The amount you pay for Abecma can vary based on several considerations, including your prescribed dosage, your health insurance benefits, and the facility or pharmacy involved in your care. Understanding the overall cost picture—including factors tied to the Abecma approval date and its status as a newer cell therapy—can help you better prepare financially. Assistance programs may also be available to reduce out-of-pocket expenses associated with Abecma treatment.
Abecma cost and savings
A range of variables can influence how much you’ll ultimately spend on Abecma therapy. These may include:
- your individualized treatment plan
- your insurance policy and level of coverage
- the healthcare facility or pharmacy administering the treatment
- the cost of appointments with your healthcare professional for Abecma administration
- any financial support programs available for Abecma (refer to the “Financial and insurance assistance” section below)
Because Abecma is a personalized CAR T-cell therapy used in certain cases of multiple myeloma, pricing often reflects the complexity of manufacturing and delivering this advanced treatment. If you want a clearer estimate of your out-of-pocket responsibility, speak directly with your doctor, pharmacist, or insurance provider. You can also review potential savings opportunities, including discounts available through Optum Perks.
Coupons and savings
If you’re looking to lower your Abecma prescription costs, consider checking available Optum Perks coupons. These savings options may help reduce eligible expenses, depending on your circumstances and treatment setting.
Brand-name vs. generic or biosimilar drugs
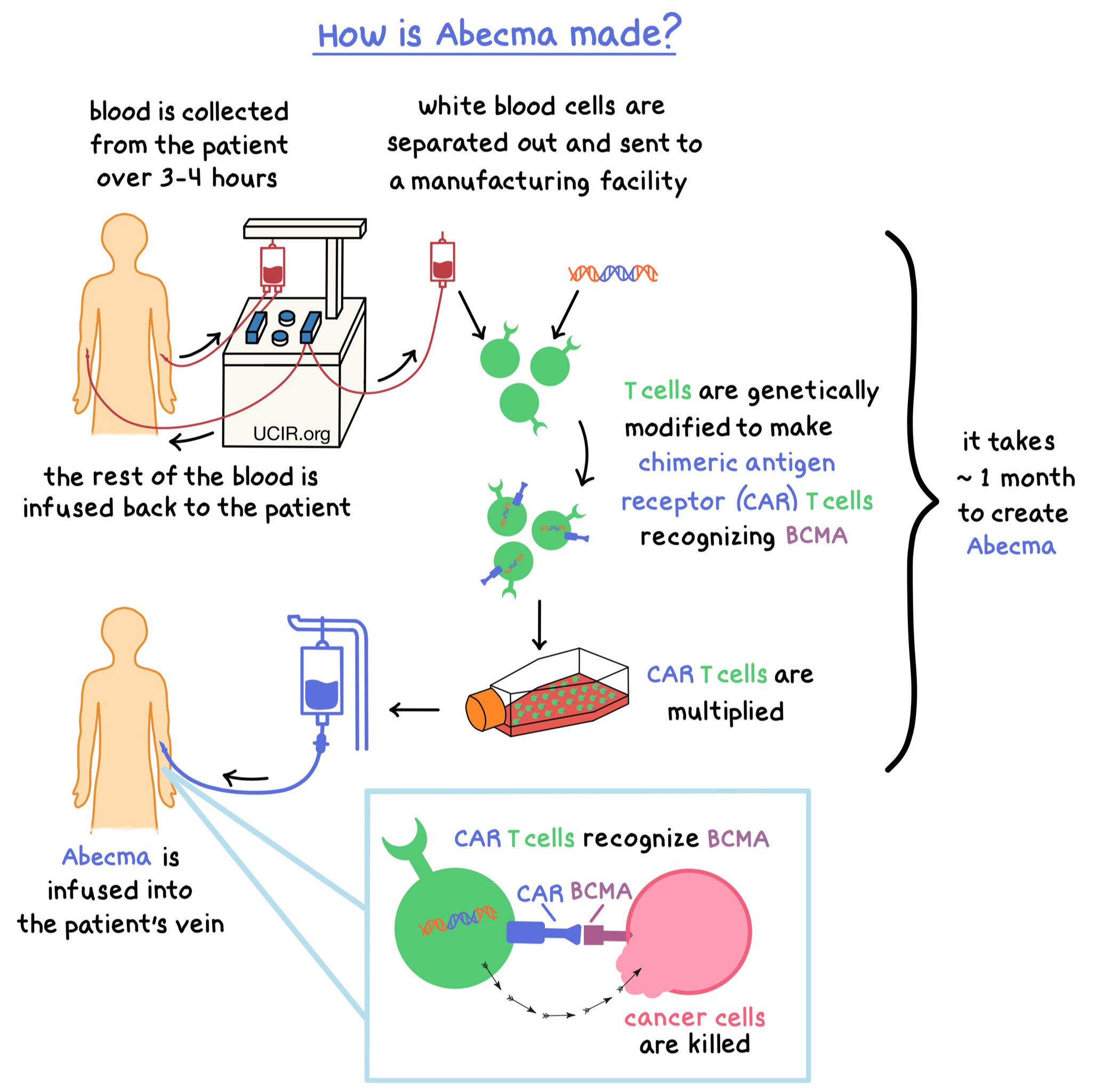
Abecma is an immunotherapy known as chimeric antigen receptor (CAR) T-cell therapy. Unlike traditional medications, CAR T-cell therapies are developed using your own immune cells. Because this process creates a highly individualized treatment, Abecma is not available as a biosimilar or generic product.
Abecma is a brand-name cell therapy. Its active ingredient, idecabtagene vicleucel, is manufactured from cells collected from your own immune system. Given its personalized design and regulatory pathway following the Abecma approval date, it remains exclusively available under its brand name. For patients comparing treatment options for relapsed or refractory multiple myeloma, you may also find it helpful to review Abecma vs Carvykti to better understand similarities and differences between CAR T-cell therapies.

Why is there such a cost difference between biologic drugs and biosimilar drugs?Biologic drugs are often costly due to the extensive research, development, and rigorous clinical testing required to confirm their safety and effectiveness. A manufacturer can market a biologic drug exclusively for up to 12 years. After the patent expires, other manufacturers may produce biosimilar versions. Increased competition in the marketplace can contribute to reduced pricing for biosimilars. Additionally, because biosimilars are highly similar to the original biologic drug, they do not require the same level of repeated clinical trials, which may further lower development costs.
For more context on regulatory milestones and how they influence access and coverage decisions, you can explore the ABECMA FDA approval history, which outlines key developments since its initial authorization.
Financial and insurance assistance
If you need help paying for Abecma or navigating your insurance benefits, support resources are available. For example:
- A support program called Cell Therapy 360 is offered for individuals receiving Abecma. To learn more and determine eligibility, call 888-805-4555 or visit the program website.
- Some organizations provide information about medication assistance programs, strategies for maximizing insurance benefits, and access to savings cards or related services. Two examples include: Medicine Assistance Tool NeedyMeds
These programs may offer guidance on coverage verification, financial counseling, travel support for treatment appointments, or help understanding benefits related to advanced oncology therapies such as CAR T-cell therapy.
Insurance considerations
If you have insurance and use Abecma, the following details may be important to review with your provider.
Prior authorization: Many insurance plans require prior authorization before covering Abecma. This process involves your doctor submitting information about your diagnosis and treatment plan to the insurance company. The insurer then determines whether the therapy meets its coverage criteria. If prior authorization is required and treatment begins before approval is granted, you may be responsible for the full cost. Contact your insurance provider to confirm whether Abecma requires prior authorization under your plan.
Type of insurance coverage: Abecma is administered by a doctor or other qualified healthcare professional, typically in a specialized treatment center. Depending on your insurance policy, the cost of Abecma may be billed under your medical benefit rather than your prescription drug benefit. This can vary based on your specific plan and the setting in which you receive treatment, such as a hospital, infusion center, or physician’s office. If you are unsure how your plan processes claims for cell therapies, speak with your healthcare team or insurance representative for clarification.
Disclaimer: HealthEH has made every effort to ensure that all information presented is accurate, thorough, and current. However, this article should not replace the advice and clinical judgment of a licensed healthcare professional. Always consult your doctor or another qualified healthcare provider before starting any medication. The drug information provided here may change and is not intended to include all possible uses, instructions, precautions, warnings, drug interactions, allergic reactions, or side effects. The absence of specific warnings does not mean that a medication or drug combination is safe, effective, or appropriate for every patient or every particular use.
















Leave a Reply
You must be logged in to post a comment.