Plantar flexion describes the motion when the top of your foot points away from your lower leg. You perform plantar flexion whenever you rise onto your toes or extend your toes downward.
Each person’s normal range for this movement varies. Multiple muscles coordinate plantar flexion. Damage to any of these muscles can reduce your range of motion and interfere with activities that require pointing the foot.
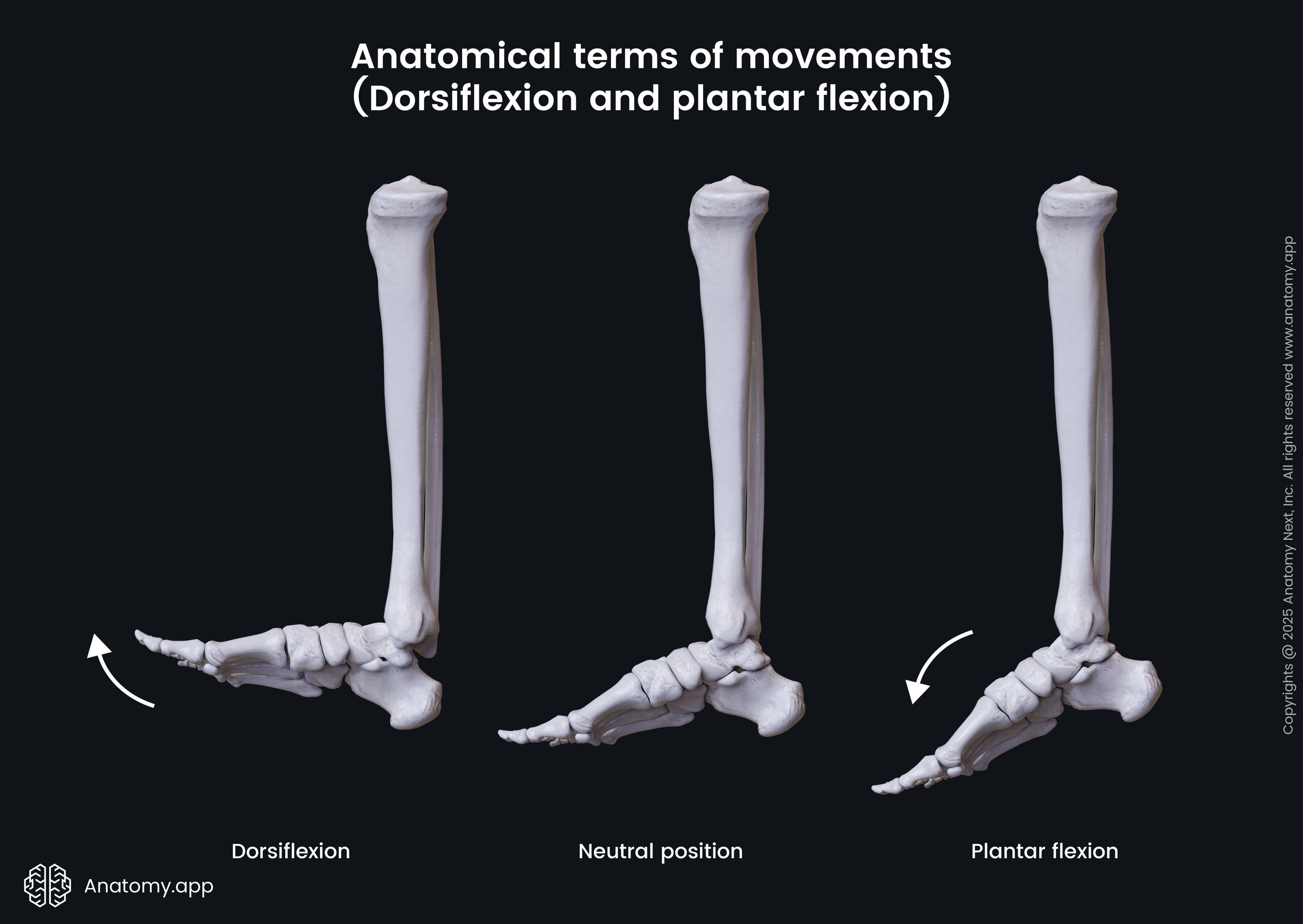
What activities involve this motion?
You rely on plantar flexion most often when:
- You stretch and direct your foot away from you.
- You stand on tiptoe, for example when reaching for an item on a high shelf.
- You press the accelerator pedal while driving.
- You perform ballet en pointe, dancing on the tips of your toes.
To a lesser extent, plantar flexion is also involved in walking, running, swimming, dancing, and cycling.
Which muscles are used?
Plantar flexion is produced by a coordinated action of several muscles in the ankle, foot, and lower leg. These include:
Gastrocnemius: This muscle constitutes a major portion of the calf. It travels down the back of the lower leg from behind the knee to the Achilles tendon at the heel and is a prime contributor to plantar flexion.
Soleus: The soleus is another key calf muscle that assists in plantar flexion. Like the gastrocnemius, it inserts into the Achilles tendon. This muscle is essential for pushing the foot away from the ground.
Plantaris: A long, thin muscle that extends along the rear of the leg from the distal femur to the Achilles tendon. The plantaris works with the Achilles complex to flex both the ankle and knee and is active when you rise onto your toes.
Flexor hallucis longus: Located deep within the lower leg, this muscle runs down to the big toe. It helps flex the big toe, enabling walking and maintaining balance when you are on tiptoe.
Flexor digitorum longus: Another deep muscle of the lower leg, it begins narrow and broadens as it descends. It flexes the toes other than the big toe.
Tibialis posterior: A smaller deep muscle in the lower leg that contributes to both plantar flexion and inversion — turning the sole inward toward the opposite foot.
Peroneus longus: Also called fibularis longus, this muscle runs along the outside of the lower leg toward the big toe. It cooperates with the tibialis posterior to stabilize the ankle when you stand on tiptoe and participates in plantar flexion and eversion — turning the sole outward.
Peroneus brevis: Situated beneath the peroneus longus, the peroneus brevis (fibularis brevis) is shorter in length. It helps maintain foot stability during plantar flexion.
What happens if these muscles are injured?
An injury to any of the muscles that facilitate plantar flexion can restrict your ability to point the foot or stand on tiptoe. Ankle injuries — including sprains and fractures — are among the most frequent causes of plantar flexion impairment.
Such injuries commonly occur in sports requiring rapid direction changes — like basketball — or in activities involving jumping.
When the muscles or bones of the ankle are hurt, the area becomes swollen and inflamed. Swelling limits movement, and depending on the injury’s severity you may be unable to point your toe or rise onto your toes until recovery.
What treatment options are available?
Mild ankle sprains are generally managed with the RICE approach:
- Rest the ankle. Avoid weight-bearing on the injured side. Use crutches or a brace to assist walking until healing occurs.
- Ice. Wrap an ice pack in a cloth and apply it to the injured area for about 20 minutes at a time, several times daily. Cold helps reduce swelling. Use ice for the first 48 hours after injury.
- Compression. Apply an elastic bandage around the injured ankle to help control swelling.
- Elevate. Raise the injured ankle on a pillow so it sits above heart level. Elevation helps minimize swelling.
Sprains typically resolve within days to weeks. If the ankle is fractured, a cast may be necessary. More complex fractures can require surgical intervention to realign the bone; surgeons may use plates or screws to stabilize the bone during healing.
How to prevent injury
Building strength in the ankle, leg, and foot muscles that support plantar flexion helps preserve flexibility, safeguard the ankle, and reduce the chance of future injury. A physical therapist can instruct you in proper exercise technique.

Choosing appropriate footwear also reduces injury risk. Have your feet measured when purchasing new shoes and avoid high heels — particularly tall, narrow styles that provide poor ankle support. For targeted support during activity or recovery consider techniques like plantar fasciitis taping when recommended by a professional.
Consult a podiatrist or orthopedic specialist for guidance on maintaining foot and ankle health and preventing plantar flexion-related problems before they begin.





















Leave a Reply
You must be logged in to post a comment.