Purpura develops when tiny blood vessels rupture beneath the skin. It tends to appear more frequently in individuals who have low platelet levels in their blood, often as a result of an underlying medical issue. Reviewing Pictures of senile purpura and related skin changes can help you recognize the condition early and understand when medical evaluation is necessary.
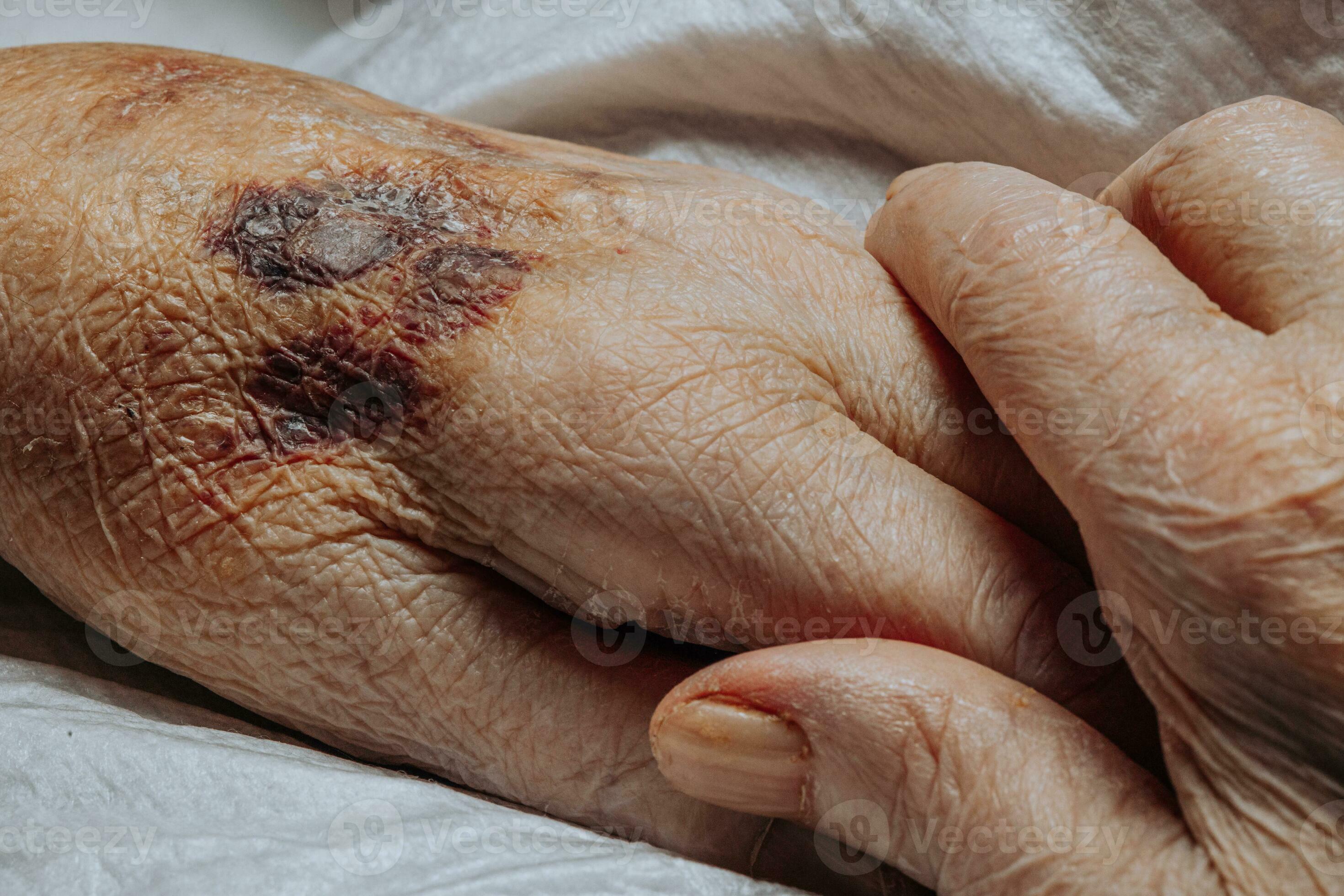
What is purpura?
Purpura, sometimes referred to as blood spots or skin hemorrhages, describes purple-colored marks that are most noticeable on the skin’s surface. These spots can also form on internal organs or mucous membranes, including the lining inside the mouth.
This condition occurs when small blood vessels break open, allowing blood to collect under the skin. The result can range from pinpoint-sized purple dots to larger, more visible patches. In many cases, purpura spots are harmless. However, they may signal a more significant health concern, such as a blood clotting disorder or platelet abnormality.
Low platelet levels may contribute to increased bruising and bleeding. Platelets are essential blood components that assist with clot formation. A reduced platelet count may be inherited or genetic, but it can also be linked to recent:
- bone marrow transplants
- cancer
- chemotherapy
- stem cell transplants
- HIV infections
- hormone replacement
- estrogen therapies
- use of certain medications
Any new or unusual skin changes, especially unexplained purple bruises or patches, should prompt a consultation with your doctor for proper assessment.
Pictures of purpura
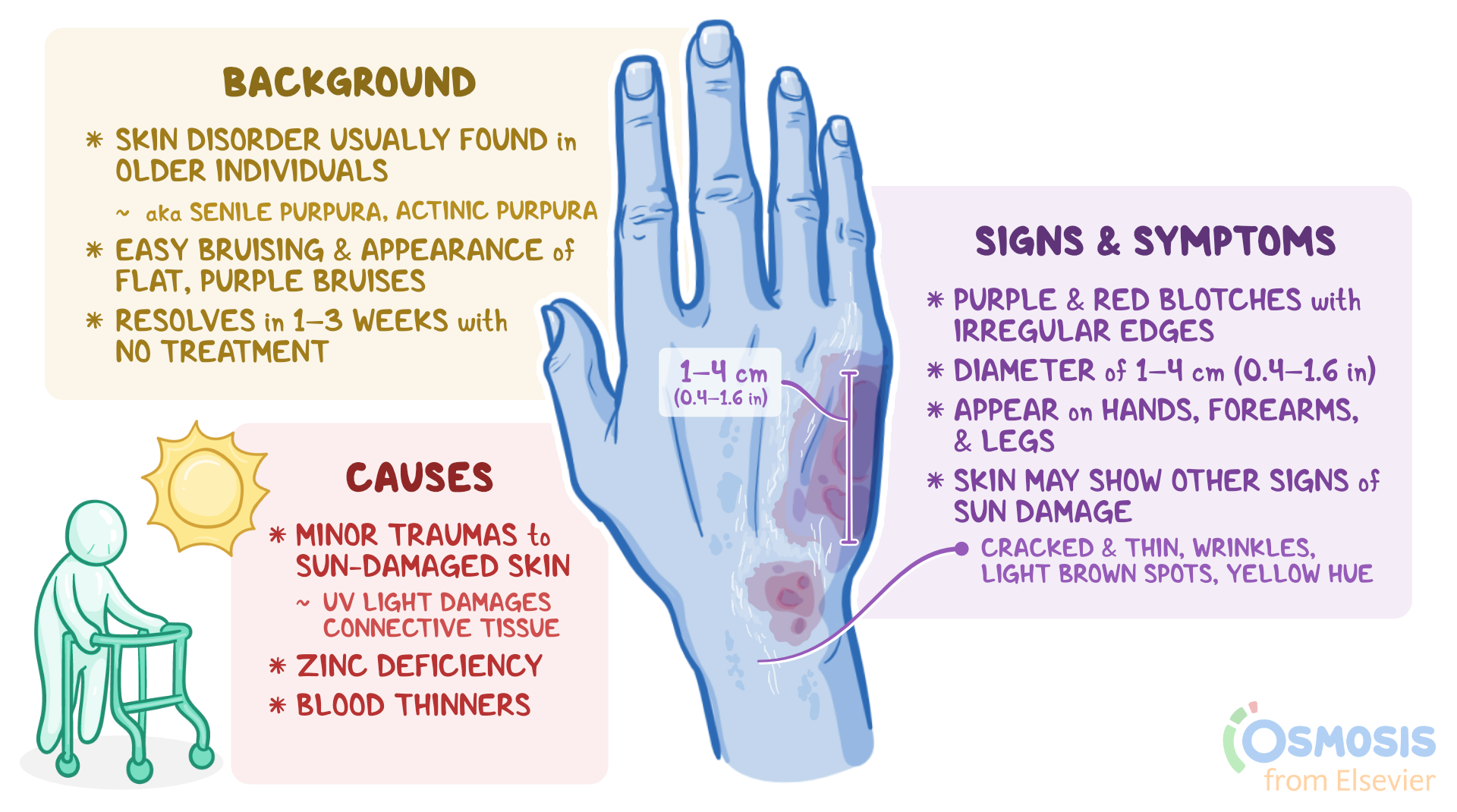
What causes purpura?
Purpura is categorized into two primary types: nonthrombocytopenic and thrombocytopenic. Nonthrombocytopenic indicates that platelet levels are within the normal range. Thrombocytopenic means the platelet count is below normal.
Potential causes of nonthrombocytopenic purpura include:
- disorders that affect blood clotting
- certain congenital disorders, present at or before birth, such as telangiectasia (fragile skin and connective tissue) or Ehlers-Danlos syndrome
- certain medications, including steroids and those that affect platelet function
- weak blood vessels
- inflammation in the blood vessels
- scurvy, or a severe lack of vitamin C
Possible causes of thrombocytopenic purpura include:
- medications that prevent platelets from forming or that interfere with normal clotting
- drugs that cause the body to launch an immune reaction against platelets
- recent blood transfusions
- immune disorders such as idiopathic thrombocytopenic purpura
- an infection in the bloodstream
- infection by HIV or Hepatitis C, or some viral infections (Epstein-Barr, rubella, cytomegalovirus)
- Rocky Mountain spotted fever (from a tick bite)
- systemic lupus erythematous
In older adults, a common variant known as senile purpura appears due to age-related thinning of the skin and fragile blood vessels. If you are specifically concerned about purple discoloration in seniors, you may find this resource helpful: What causes purple bruising in elderly. Comparing your symptoms with reliable Pictures of senile purpura can also offer visual guidance, though a clinical diagnosis is always essential.

How is purpura diagnosed?
To diagnose purpura, your doctor will conduct a physical examination of your skin and review your personal and family medical history, including when the spots first appeared. Blood tests, including a platelet count, are commonly performed. In some situations, a skin biopsy may also be recommended.
These diagnostic steps help determine whether the purpura is associated with a more serious issue, such as a platelet disorder or another blood-related condition. Measuring platelet levels plays a key role in identifying the underlying cause and guiding treatment decisions.
Purpura can affect both children and adults. In children, it often develops after a viral infection and may resolve completely without treatment. Most children with thrombocytopenic purpura recover within several months. In adults, however, purpura is more likely to have chronic causes and may require ongoing management to control symptoms and maintain healthy platelet counts.
When evaluating cases in older adults, doctors may compare findings with Pictures of senile purpura to distinguish age-related skin fragility from other bleeding disorders, ensuring that serious conditions are not overlooked.
How is purpura treated?
Treatment depends largely on the underlying cause of purpura. Adults with mild thrombocytopenic purpura may recover without medical intervention.
If the condition responsible for purpura does not resolve spontaneously, medical therapy may be necessary. Treatment options include medications and, in some cases, a splenectomy, which is surgical removal of the spleen. Your doctor may also advise discontinuing medications that interfere with platelet function, such as aspirin, blood thinners, and ibuprofen.
Corticosteroids
Your doctor may prescribe a corticosteroid medication to help raise your platelet count by suppressing immune system activity. Platelet levels typically return to a safer range within two to six weeks. Once stabilized, the medication is generally tapered and discontinued.
Long-term use of corticosteroids carries potential risks, including weight gain, cataracts, and bone loss. It’s important to review these risks with your healthcare provider before extended treatment.
Intravenous immunoglobulin
If your purpura results in significant bleeding, your doctor may administer intravenous immunoglobulin (IVIG). IVIG may also be used when a rapid increase in platelet count is required before surgery. Although IVIG is often effective, its benefits are usually temporary. Possible side effects include headache, nausea, and fever.
Other drug therapies
Newer medications for chronic immune (idiopathic) thrombocytopenic purpura (ITP) include romiplostim (Nplate) and eltrombopag (Promacta). These drugs stimulate the bone marrow to produce more platelets, lowering the risk of bruising and bleeding. Potential side effects include:
- headaches
- dizziness
- nausea
- joint or muscle pain
- vomiting
- increased risk of blood clots
- acute respiratory distress syndrome
- pregnancy
Biologic therapy, such as rituximad (Rituxan), may help reduce immune system activity. It is typically reserved for patients with severe thrombocytopenic purpura or for those who do not respond to corticosteroid therapy. Side effects can include:
- low blood pressure
- sore throat
- rash
- fever
Splenectomy
If medications do not effectively manage thrombocytopenic purpura, your doctor may recommend a splenectomy. Because the spleen plays a central role in removing platelets from circulation, its removal can quickly elevate platelet counts.
However, splenectomy is not successful in all patients and carries risks, including a lifelong increased susceptibility to infection. In emergency situations involving severe bleeding, hospitals may administer platelet concentrates, corticosteroids, and immunoglobulin.
After treatment begins, your doctor will routinely monitor platelet counts to evaluate effectiveness and adjust therapy as needed.
What is the outlook for purpura?
The prognosis for purpura depends on its underlying cause. Once a diagnosis is confirmed, your doctor will discuss treatment strategies and the expected long-term outlook.
In rare instances, untreated thrombocytopenic purpura can lead to excessive bleeding in certain parts of the body. Severe bleeding in the brain may result in a fatal brain hemorrhage.
Individuals who receive prompt treatment or who have mild cases often achieve full recovery. However, in more severe cases or when therapy is delayed, purpura may become chronic. If you notice persistent or unexplained purple spots—especially after reviewing Pictures of senile purpura or other examples—seek medical advice without delay.
Living with purpura
In some cases, purpura spots may not disappear entirely. Certain medications and activities can worsen bruising. To minimize the formation of new spots or prevent existing ones from worsening, avoid medications that reduce platelet count, including aspirin and ibuprofen, unless directed otherwise by your physician.
Opting for low-impact physical activities instead of high-impact sports can also lower your risk of injury, bruising, and bleeding. Protective measures, such as wearing long sleeves to shield fragile skin in older adults with senile purpura, may further reduce trauma-related discoloration.
Managing a chronic condition can be emotionally challenging. Connecting with others who have purpura through support groups or online communities may provide reassurance and practical coping strategies.
Q:
Are there any natural or herbal remedies that are effective for purpura?
A:
Because purpura can arise from multiple underlying causes, there is no universal treatment that works for every case. Identifying the root cause is essential before choosing a management strategy. At present, there are no natural or herbal remedies proven to reliably treat this condition.
If you are considering complementary or alternative therapies, consult an integrative medicine physician. These professionals are trained in both conventional and complementary medicine, emphasizing a holistic mind-body-spirit approach. You can locate qualified integrative health specialists here: http://integrativemedicine.arizona.edu/alumni.html



















Leave a Reply
You must be logged in to post a comment.