What is diabetic peripheral neuropathy (DPN)?
The Foundation for Peripheral Neuropathy estimates that approximately 40 million Americans live with some type of peripheral neuropathy. Among them, about 20 million cases are attributed to diabetic peripheral neuropathy (DPN), making it the most prevalent form of peripheral neuropathy.
DPN primarily damages the nerves in the hands and feet and is closely associated with the early changes often seen in Diabetic feet pictures beginning stages. In these early stages, individuals may begin noticing subtle sensory differences before visible skin complications appear. Common sensations linked to DPN include:

- numbness
- tingling
- pain
Beyond the extremities, nerve dysfunction may also develop in your:
- digestive tract
- heart
- eyes
- other organ systems
Possible contributors to nerve injury include:
- high blood sugar levels
- having had diabetes for a long time
- low levels of insulin or treatment with insulin
- inflammation in the nerves
- lifestyle factors, like smoking or alcohol use
Tingling and numbness
Researchers do not fully understand the precise mechanism by which diabetes harms nerves. One leading theory suggests that persistently elevated blood sugar levels interfere with the protective coating that surrounds nerve fibers.
Another explanation points to reduced blood flow to the nerves, which may deprive them of essential oxygen and nutrients, ultimately resulting in damage.
As DPN advances, you may detect tingling or numbness in your extremities. These early sensory changes often appear in areas highlighted in Diabetic feet pictures beginning stages, particularly affecting the:
- fingers
- toes
- hands
- feet
Some individuals also report a “pins-and-needles” sensation or a persistent burning feeling. Recognizing these early warning signs—similar to those described in Woman early signs of diabetic feet—can help prompt earlier medical evaluation and better long-term outcomes.
Shooting pain
When a nerve becomes compressed or damaged, it may transmit abnormal signals that result in shooting pain. Many people compare this sensation to an electric shock or a sharp, stabbing discomfort.
This pain can occur because injured nerves misfire, sending incorrect or exaggerated signals to the brain.
Symptoms may fluctuate, appearing intermittently, or they may persist continuously. Shooting or electric-like pain is frequently worse at night and can significantly interfere with restful sleep, which in turn may impact blood sugar control and overall well-being.
Extreme sensitivity
Consider how sensitive an open wound feels when touched. Diabetic neuropathy can trigger a similar response, even without visible injury.
If the protective covering of a nerve deteriorates, the affected area may become extremely sensitive.
In more advanced cases, even light contact—such as a gentle brush against your foot or bedsheets touching your skin—can provoke intense pain. For individuals with severe neuropathy, tolerating normal daily contact may become challenging. This heightened sensitivity is another feature sometimes observed in early Diabetic feet pictures beginning stages, even before ulcers develop.
Muscle weakness
Your muscles rely on healthy nerves to function properly. When nerves sustain damage, muscle control may decline.
Diabetes can also impair blood vessels, reducing circulation to muscle tissue. Over time, this combination may cause muscles to weaken gradually.
According to the National Institute of Neurological Disorders and Stroke, muscle weakness is a frequent manifestation of nerve damage. As the condition progresses, some individuals may experience muscle twitching or even noticeable muscle loss, further affecting balance and coordination.
Inability to feel hot and cold
Nerves enable you to interpret environmental sensations, including temperature changes and pain. They alert you when something is hot, cold, or potentially harmful.
When nerves are severely damaged, they may cease functioning altogether. In such cases, you might not realize you have stepped on a tack or developed a blister. Minor injuries can therefore go unnoticed and untreated, increasing the likelihood of infection or other complications. Issues such as Red soles of feet diabetes may also develop without immediate awareness if sensation is diminished.
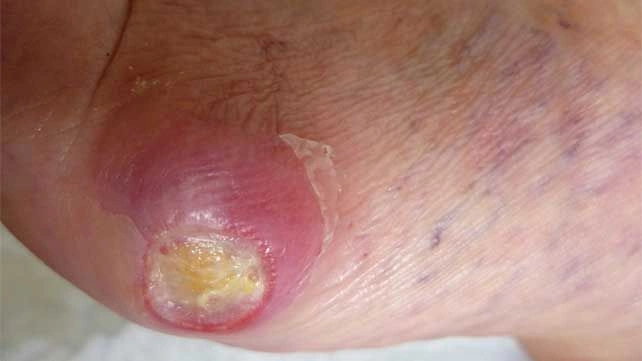
Foot problems
If nerve function decreases in your feet, early skin abnormalities may not be immediately apparent. These can include:
- blister
- ulcer
- wound
Without prompt detection, these issues may only become noticeable once they are:
- infected
- swollen
- inflamed
Healthcare professionals strongly advise that people with diabetes perform daily inspections of their feet and hands. This is especially critical if you have already experienced nerve damage or reduced sensation in your fingers or toes. Careful monitoring can help identify subtle changes often depicted in Diabetic feet pictures beginning stages before they escalate into serious diabetic foot complications.

In addition to daily checks, maintaining proper foot hygiene, trimming nails carefully, and wearing well-fitted footwear can significantly lower the risk of ulcers and infections.
Difficulty walking and performing other daily tasks
Nerves play a crucial role in allowing you to carry out routine activities, including:
- buttoning up a shirt
- walking
- opening a door
When nerve damage affects the hands and feet, these everyday tasks may become more difficult or, in severe cases, impossible.
Supportive devices and adaptive tools are available to improve function and independence, such as:
- specialized orthotic inserts
- diabetic shoes
- gripping tools
Structural changes in the foot can also occur due to muscle imbalance and nerve damage, sometimes requiring customized shoe fittings to prevent pressure points and further injury.
Autonomic symptoms
Nerves are responsible not only for movement and sensation but also for regulating many automatic body functions. The autonomic nervous system influences:
- perspiration
- sexual function
- heart rate
- urinary function
- temperature regulation
If diabetes impacts these autonomic nerves, a range of symptoms may develop, including:
- stomach upset, including constipation, diarrhea, nausea, vomiting
- urinary problems, such as incontinence or urinary tract infections
- erectile dysfunction or vaginal dryness
- inability to stay warm or cool
- difficulty focusing your eyes
- dry, cracked skin
- inability to feel low blood sugar
Because these symptoms may develop gradually, discussing new or worsening changes with your healthcare provider is essential for comprehensive diabetes management.
Coping with nerve damage
Preventing or slowing the progression of DPN begins with effective blood sugar management. Keeping glucose levels within the target range can significantly delay further nerve deterioration and reduce symptom severity.
Additional strategies that may help include:
- exercising regularly
- managing your weight
- reducing stress
Regular physical activity can enhance circulation, support nerve health, and improve balance, which may reduce fall risk. Stress management techniques—such as mindfulness, adequate sleep, and structured routines—can also contribute to more stable blood sugar levels.
If nerve damage has already occurred, consult your doctor about lifestyle adjustments, protective footwear, and symptom-relieving treatments. Certain medications are available to help manage pain and other complications, allowing you to maintain a higher quality of life while minimizing the risk of advanced diabetic foot problems.



















Leave a Reply
You must be logged in to post a comment.