Cellulitis can present with a range of symptoms depending on the specific bacteria responsible and the location on your body where the infection develops. These variables often guide a doctor’s decision about which antibiotic therapy will be most effective. Reviewing Pictures of cellulitis on foot can also help you recognize early warning signs, especially since the feet and legs are among the most commonly affected areas.

Cellulitis is a bacterial infection involving the deeper layers of the skin and the underlying soft tissues. Although it can occur anywhere, it most frequently appears on the lower leg or foot. Seeing Pictures of cellulitis may give you a clearer understanding of how this condition can look in different stages and body regions.
Healthcare professionals categorize cellulitis in several ways, including by the type of bacteria causing it and by its anatomical location. These classifications help determine the most appropriate treatment plan and whether oral or intravenous antibiotics are needed.
Continue reading to explore the different forms of cellulitis, their symptoms, and when to seek medical care for proper diagnosis and treatment.
Types of cellulitis by cause
Cellulitis develops as a result of bacterial infection. Identifying the specific organism involved can influence the course and duration of treatment.
While most cellulitis cases are linked to strains of Staphylococcus, many other bacteria can also trigger this skin and soft tissue infection.
- Staphylococcus: Staphylococcus aureus is a major cause of cellulitis. Infections from Staphylococcus (staph) are sometimes referred to as “purulent cellulitis” because symptoms often include pus, drainage, or abscess formation.
- Streptococcus: Streptococcus pyogenes is one of the most common causes of cellulitis. Infection with Streptococcus frequently follows a cut, burn, surgical incision, wound, or other skin trauma.
- Pasteurella multocida: Cellulitis caused by these bacteria typically develops within 1–2 days after an animal bite or scratch.
- Capnocytophaga: These organisms normally reside in the mouths of humans, cats, and dogs but may cause infection under certain conditions. Human infections are common following dog bites.
- Vibrio vulnificus: These bacteria can enter through open wounds exposed to salt water or contaminated seafood and may sometimes require hospitalization due to severity.
- Aeromonas: Various species of Aeromonas can cause wound and soft tissue infections such as cellulitis, as well as gastrointestinal illness.
- Haemophilus influenzae: These invasive bacteria are capable of causing cellulitis in addition to conditions like meningitis and infectious arthritis.
- Pseudomonas: These bacteria are associated with post-surgical infections, and Pseudomonas aeruginosa is most likely to result in cellulitis.
Types of cellulitis by location
Cellulitis can affect virtually any part of the body. Physicians often describe the infection according to the region involved, which can also influence symptoms and potential complications.
Lower limb (leg) cellulitis
Cellulitis most frequently involves the legs, often affecting just one side. Group A Streptococcus is a typical cause of lower limb cellulitis, though staph infections are also common contributors. If you are searching for Pictures of cellulitis on foot or examples affecting the calf or shin, you may also find Pictures of cellulitis on the leg helpful for comparison.
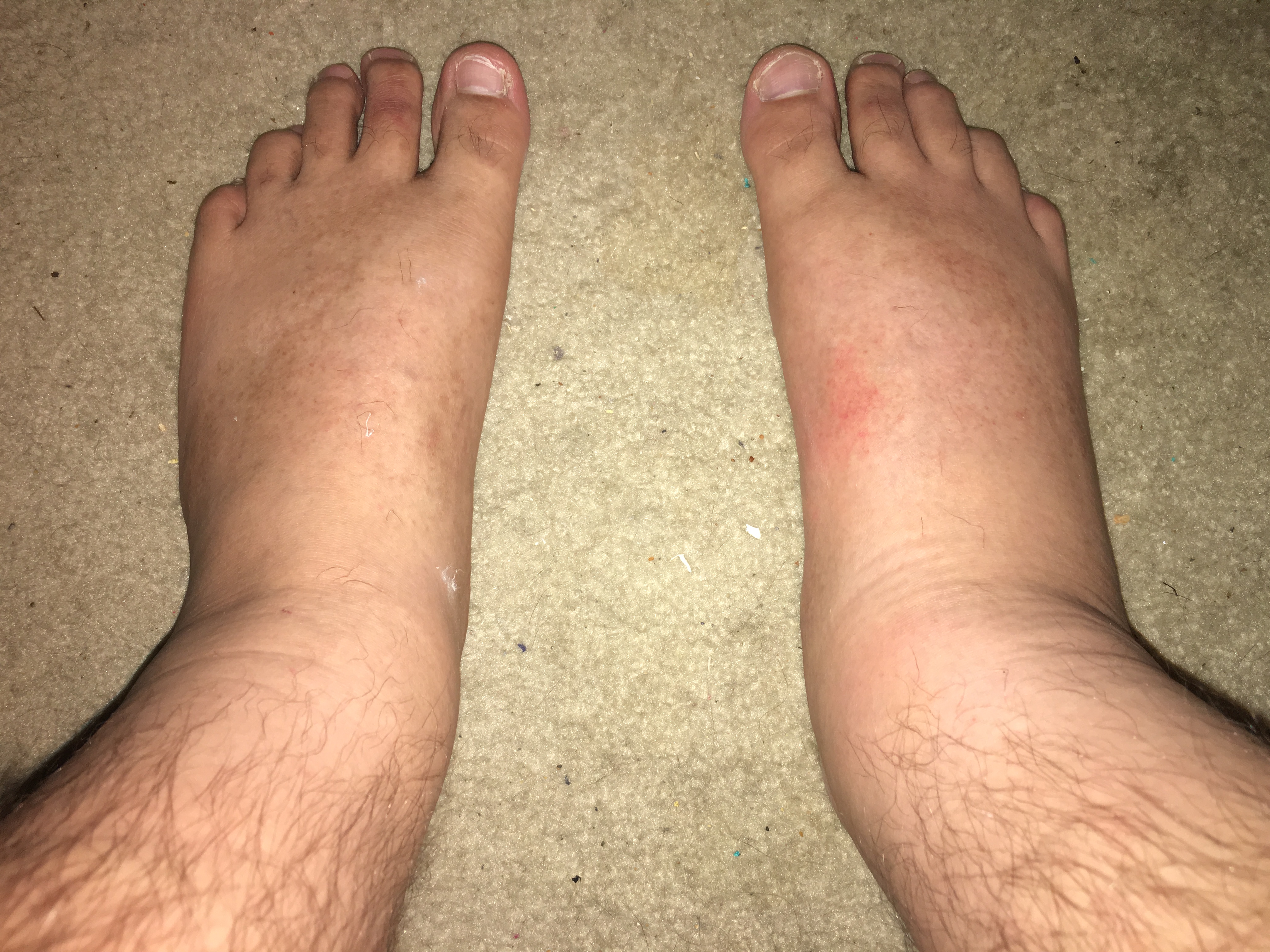
Risk factors for lower limb cellulitis include:
- wounds
- leg ulcers
- lymphedema or leg edema
- excoriation disorder
- athlete’s foot
- obesity
- previous cellulitis
Because the skin barrier is compromised in many of these conditions, bacteria can more easily penetrate into deeper tissues, leading to redness, swelling, warmth, and pain.
Perianal cellulitis
Perianal cellulitis occurs around the anal region and is most often caused by streptococcal infection. Also called perianal streptococcal dermatitis, this condition primarily affects children under 10 years old and is two to three times more frequent in boys.
Treatment generally includes a combination of oral antibiotics and topical medications to clear the infection and relieve discomfort.
Orbital cellulitis
Orbital cellulitis involves the fat and muscle tissues surrounding the eye. It usually results from a bacterial sinus infection that spreads behind the eye socket. Children are most commonly affected.
A course of antibiotics for 2–3 weeks typically resolves the infection, though severe or complicated cases may require surgical intervention to prevent vision loss or other complications.
Periorbital cellulitis
Periorbital cellulitis, also known as preseptal cellulitis, affects the eyelid and the skin surrounding the eye. Like orbital cellulitis, it may arise from a sinus infection or from a skin injury. Staph and strep bacteria are common causes, particularly in children.
This form is generally less severe and more prevalent than orbital cellulitis, but it can progress without timely treatment. Most cases improve within 5–7 days of appropriate antibiotics.
Facial cellulitis
In the past, Haemophilus influenzae was a frequent cause of facial cellulitis, especially in children younger than 5 years. However, increased vaccination rates have significantly reduced its occurrence.
Other bacteria, including bacteria in your mouth associated with dental cavities, can also lead to facial cellulitis. In such instances, dental treatment, including possible tooth extraction, may be necessary in addition to antibiotics.
Breast cellulitis
Breast cellulitis may develop after a skin injury, but it more commonly follows breast cancer surgery, breast augmentation, or breast reduction.
A 2018 research review found that 3–8% of individuals develop cellulitis after breast cancer surgery, though the true number may be higher due to underreporting. While many cases occur within weeks of surgery, symptoms can also appear months later.
What are the most common locations of cellulitis on the body?
Adults usually experience cellulitis on one leg or foot. This is why many people search for Pictures of cellulitis on foot to compare early redness or swelling with their own symptoms. In contrast, children more often develop cellulitis on the face or neck.
Pictures of different cellulitis types
Purulent vs. nonpurulent cellulitis
Doctors also describe cellulitis as either purulent or nonpurulent, depending on whether pus is present.
Purulent cellulitis involves pus, abscess, or phlegmon. A phlegmon resembles an abscess but spreads more diffusely through tissue. This type is usually caused by Staphylococcus aureus, including MRSA.
Nonpurulent cellulitis, on the other hand, is typically linked to group A, B, C, or G Streptococcus infections and does not produce visible pus.
Erysipelas
Erysipelas is a superficial bacterial skin infection that does not extend into the deeper dermis. It generally appears in a well-demarcated, clearly outlined area.
Compared with erysipelas, cellulitis tends to cause more intense skin discoloration and deeper tissue involvement.
Both conditions may lead to swelling and tenderness. However, feeling generally unwell or systemically ill is more commonly associated with erysipelas.
Staphylococcus and Streptococcus bacteria can both cause these infections. Cellulitis is most often due to Staphylococcus, whereas erysipelas is usually caused by Streptococcus.
What is the treatment for cellulitis?
Antibiotics are the typical treatment for cellulitis. The selected antibiotic depends on the suspected or confirmed bacterial source.
Standard therapy generally lasts at least 5 days. If there is limited improvement, a doctor may extend the duration of treatment.
Mild cases are commonly managed with oral antibiotics. More serious infections, especially those accompanied by systemic symptoms, may require intravenous (IV) antibiotic therapy in a hospital setting.
Elevating the affected limb, particularly in lower leg or foot infections, can help reduce swelling and promote healing. In cases of purulent cellulitis, a healthcare professional may need to drain an abscess or address a phlegmon to fully resolve the infection.
When to contact a doctor
Contact a doctor if you notice symptoms of cellulitis such as:
- swelling
- warm and tender skin
- painful area of skin
- color changes
Seek urgent medical care if:
- skin discoloration spreads rapidly
- you develop a fever or chills
- the infection involves the area around your eye
Takeaway
Cellulitis is a bacterial infection that affects the deeper layers of the skin and underlying tissues. The type of bacteria involved, the location of the infection, and the presence of pus or systemic symptoms all play a role in determining the best treatment approach.
For most mild cases, several days of oral antibiotic therapy are sufficient. In more severe situations, intravenous antibiotics and closer medical monitoring may be necessary to prevent complications and ensure full recovery.




















Leave a Reply
You must be logged in to post a comment.