Many people do not encounter the dangerous complications of atherosclerosis — the stiffening and narrowing of arteries — until middle age, although the earliest changes can begin in childhood.
The condition is usually progressive and worsens over time. Gradually, plaque — composed of fatty deposits (cholesterol), calcium, and other cellular debris — accumulates within a major artery. As the artery narrows, blood flow to downstream tissues is reduced.
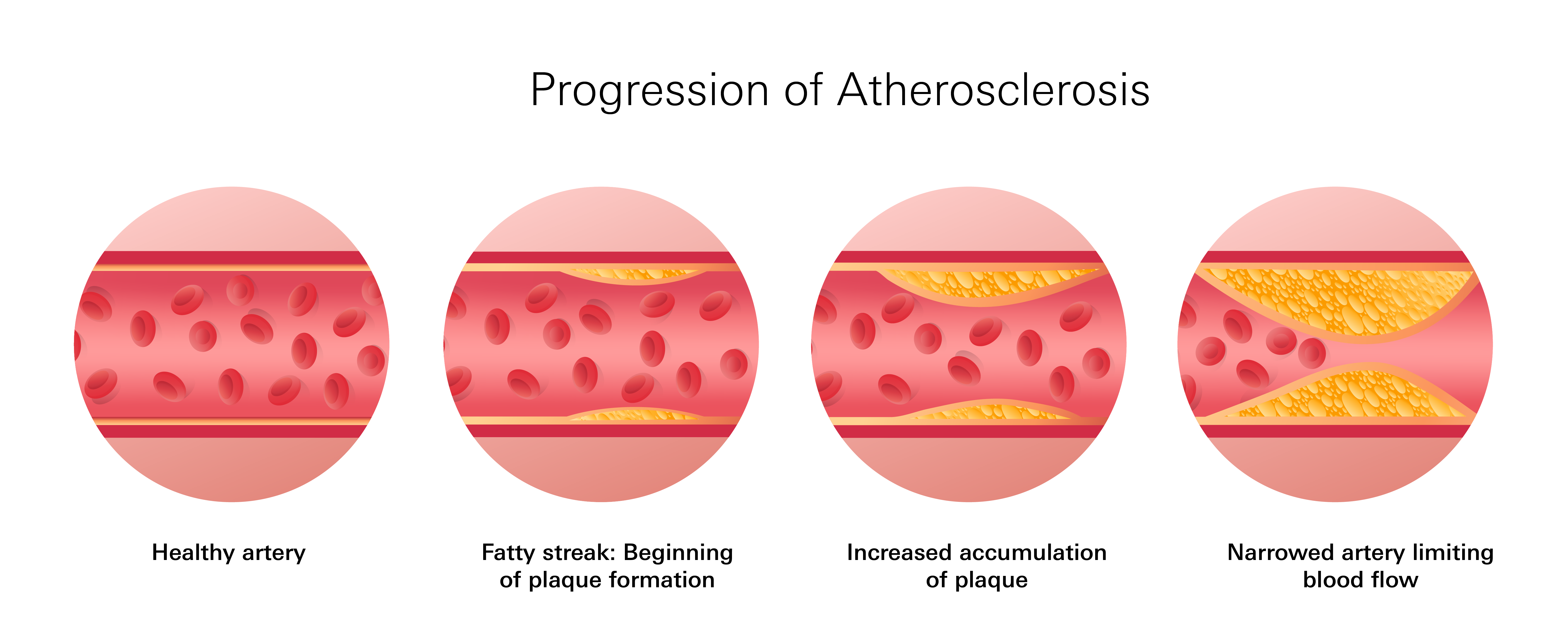
There’s also an increased chance that a clot forming elsewhere could dislodge, travel to the narrowed artery, and obstruct blood flow entirely, triggering a heart attack or stroke.
What causes it?
Atherosclerosis is a multifactorial process that often begins early in life and advances with age. Research indicates that children as young as 10 to 14 may display early signs of atherosclerotic change.
For some, the disease speeds up during their 20s and 30s; for others, significant problems may not appear until their 50s or 60s.
The exact trigger isn’t fully understood, but plaque formation is thought to start after injury to the arterial lining. Common factors that damage this lining include elevated cholesterol, high blood pressure, and tobacco use.
What are the risks?
Your arteries deliver oxygen-rich blood to critical organs like the heart, brain, and kidneys. When these vessels become obstructed, the affected organs cannot perform properly. The specific effects depend on which arteries are involved.
Conditions associated with atherosclerosis include:
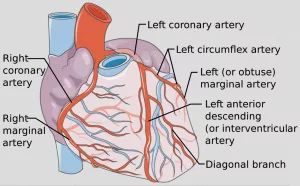
- Heart disease. Plaque in the coronary arteries (the vessels supplying the heart) raises the chance of a heart attack.
- Carotid artery disease. Plaque in the carotid arteries — the large vessels on each side of the neck that supply the brain — increases stroke risk.
- Peripheral artery disease. Plaque in the arteries supplying the arms and legs can cause pain, numbness, and serious infections.
- Kidney disease. Plaque in arteries supplying the kidneys impairs their function. When kidneys fail to work well, they cannot eliminate wastes properly, leading to severe complications.
How do you get tested?
During a routine exam, your doctor may detect signs such as a weak pulse near a major artery, lower blood pressure in an arm or leg, or indications of an aneurysm. Blood tests can reveal elevated cholesterol levels.
More detailed evaluations include:
- Imaging tests. Ultrasound, computed tomography (CT) scans, or magnetic resonance angiography (MRA) let clinicians visualize arteries and assess the extent of blockages.
- Ankle-brachial index. Comparing blood pressure in the ankle with that in the arm can reveal disparities suggestive of peripheral artery disease.
- Stress test. Monitoring heart and respiratory function during exercise (such as using a stationary bike or treadmill) can unmask problems that appear only when the heart is working harder.
Can it be treated?
When lifestyle adjustments are insufficient, medications and surgical options exist. These aim to halt disease progression and relieve symptoms, particularly chest or leg pain.
Drug therapy typically addresses high blood pressure and high cholesterol. Examples include:
- statins
- beta-blockers
- angiotensin-converting enzyme (ACE) inhibitors
- antiplatelet agents
- calcium channel blockers
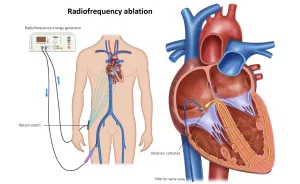
Surgical intervention is reserved for severe, potentially life-threatening blockages. Surgeons may remove plaque directly from an artery or create a bypass to reroute blood around the obstruction.
What lifestyle changes can help?
Adopting a healthier diet, quitting smoking, and exercising are potent measures to lower high blood pressure and cholesterol — two principal drivers of atherosclerosis.
Exercise
Regular physical activity supports weight loss, helps maintain normal blood pressure, and raises “good” HDL cholesterol. Aim for 30 to 60 minutes daily of moderate aerobic exercise.
Diet
- Maintain a healthy weight by increasing fiber intake. One approach is replacing refined breads and pastas with whole-grain alternatives.
- Eat plenty of fruits and vegetables and include healthy fats. Olive oil, avocado, and nuts provide fats that do not raise “bad” LDL cholesterol.
- Limit your cholesterol intake by cutting back on high-cholesterol foods such as cheese, whole milk, and eggs. Avoid trans fats and reduce saturated fats (commonly found in processed foods), since both prompt your body to produce more cholesterol.
- Reduce sodium consumption, as excess salt contributes to high blood pressure.
- Limit alcohol use. Regular drinking can elevate blood pressure and contribute to weight gain because of its high caloric content.
These practices are most effective when started early, but they benefit individuals at any age.


















Leave a Reply
You must be logged in to post a comment.