What is a coronary artery spasm?
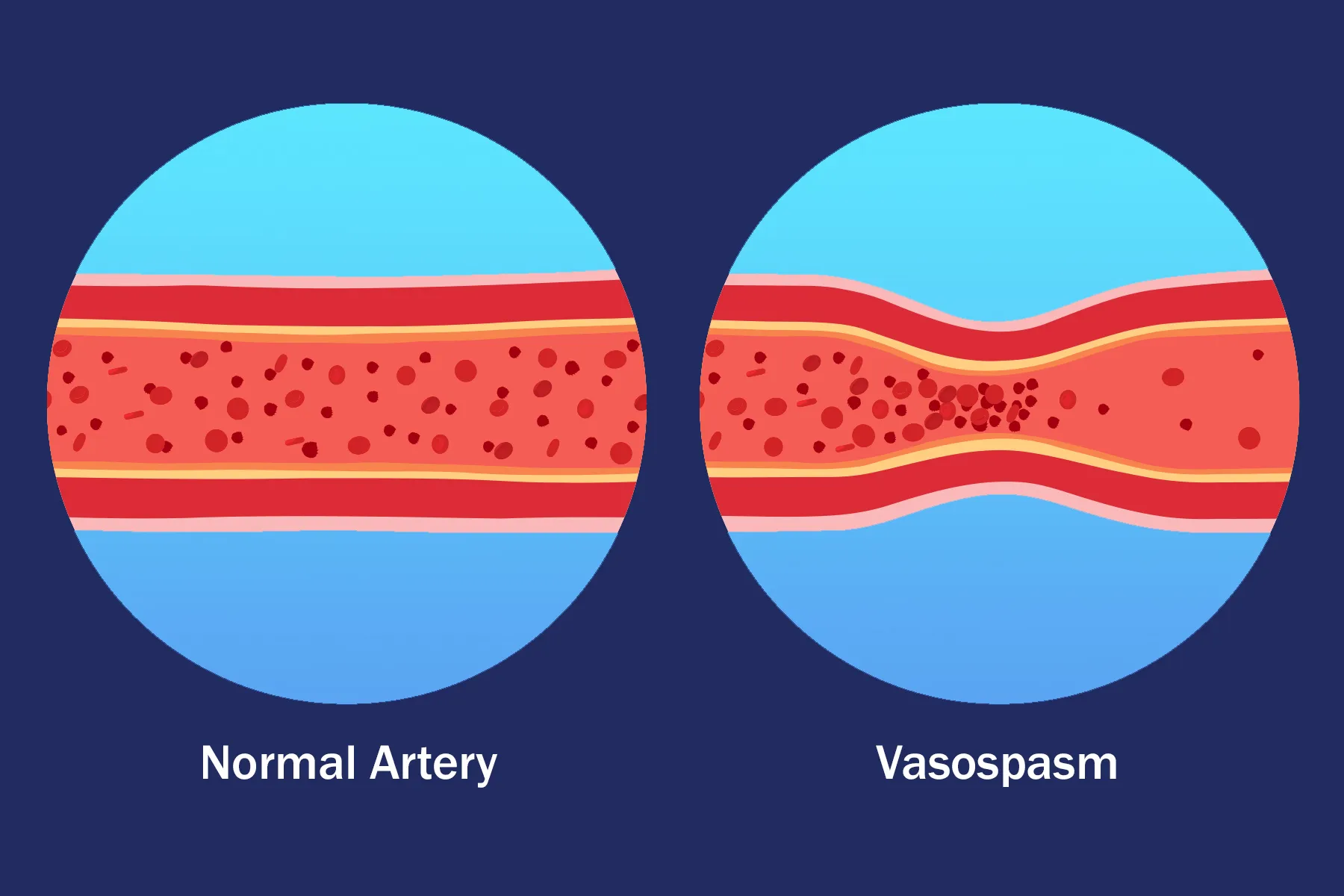
A Coronary artery spasm occurs when the muscular wall of a heart artery suddenly tightens. This abrupt contraction causes the artery to narrow, temporarily limiting or blocking blood flow to the heart muscle.
Although these episodes are usually short-lived, a coronary artery spasm can sometimes result in serious heart-related complications, including a heart attack. Individuals who already have cardiovascular risk factors—such as high cholesterol or high blood pressure—may be more prone to experiencing these spasms.
Coronary artery spasms are also referred to as coronary artery contractions or coronary artery vasospasm. Understanding this condition is essential for recognizing warning signs and reducing the risk of long-term heart damage.
What are the symptoms of a coronary artery spasm?
Many cases of coronary artery spasm remain undetected because symptoms may be mild or inconsistent. However, even when symptoms are subtle, the condition can still pose significant risks, as repeated spasms may eventually contribute to a heart attack.
You might experience intermittent, mild chest discomfort. In other situations, symptoms may be more noticeable. Common signs include:
- chest pain or angina
- pain on the left side of your chest
- chest tightness
- a feeling of constriction
The discomfort may also radiate from the chest to the arms, neck, shoulders, or jaw. Because these symptoms can overlap with other causes of chest pain—including issues like a Weird muscle spasm near heart—it’s important not to ignore persistent or recurring pain.
You may suspect coronary artery spasms if your chest pain:
- occurs during rest
- lasts from five minutes to as long as 30 minutes at a time
- occurs most often at night or early in the morning
These patterns are characteristic of vasospastic episodes and should prompt medical evaluation, especially if you have underlying cardiovascular risk factors.
What causes a coronary artery spasm?
The precise cause of a coronary artery spasm is not fully understood. Researchers believe several factors may contribute to its development.
Autonomic nervous system. This system regulates involuntary bodily functions such as heart rate and blood pressure. Evidence suggests it plays a role in coronary artery spasm, particularly since episodes frequently occur at night. The neurotransmitter acetylcholine and the hormone catecholamine may trigger artery constriction. Still, the interaction between these elements remains complex and not completely defined.
Endothelial cells. These cells line the interior of blood vessels, including those in the heart. In some individuals with coronary artery spasm, endothelial cells may not produce adequate nitric oxide, a substance that helps blood vessels relax. A deficiency in nitric oxide can promote abnormal constriction of the arteries.
Oxidative stress. Oxidative stress can lead to inflammation and damage to endothelial cells, contributing to narrowing of the vascular walls. Smoking is a significant source of oxidative stress and is strongly linked to vasospastic activity.
Smooth muscle function. The coronary arteries contain smooth muscle tissue. Variations in how this muscle contracts and relaxes may increase susceptibility to sudden arterial tightening.
Genetics. Although there is no specific genetic screening test for coronary artery spasm, certain genetic differences have been observed in affected individuals. For instance, some people have gene variations that influence how endothelial cells release nitric oxide, potentially increasing their risk.
Additionally, inflammation—often identified by a high-sensitivity C-reactive protein test—and insulin resistance are associated with coronary artery vasospasm, although they may not be direct causes. These associations highlight the broader link between metabolic health and coronary artery function.
What are the risk factors for a coronary artery spasm?
Your likelihood of developing a coronary artery spasm rises if you also carry risk factors for heart disease. Conditions such as high cholesterol and high blood pressure can directly increase the risk of arterial narrowing and dysfunction.
Other factors that may elevate your risk include:
- smoking
- excess use of stimulants, such as cocaine and amphetamines
- extreme stress
- extreme cold
- alcohol withdrawal
Managing these triggers is essential, particularly if you have previously experienced a coronary artery spasm. Continued exposure can heighten the chance of recurrent episodes. For individuals who are unsure whether their discomfort is heart-related or muscular, learning about How to stop muscle spasms in chest may help differentiate symptoms—but any persistent chest pain should always be evaluated by a healthcare professional.
How is a coronary artery spasm diagnosed?
A coronary artery spasm often signals an underlying heart issue. For this reason, your doctor may recommend several imaging and diagnostic tests to assess your cardiovascular health and rule out other serious conditions.

Common diagnostic tools include:
- electrocardiogram (EKG), which records the electrical activity of your heart and can detect abnormal rhythms or signs of ischemia
- echocardiogram, an ultrasound examination that uses sound waves to create detailed images of your heart’s structure and function
- coronary angiography: a procedure involving insertion of a small tube (catheter) into an artery in the arm or groin, guiding it to the heart, injecting contrast dye, and capturing multiple x-ray images to visualize blood flow
These evaluations allow your doctor to determine whether narrowed arteries, blockages, or functional abnormalities are present. An accurate diagnosis is critical for creating an effective treatment strategy and reducing the risk of complications.
How is a coronary artery spasm treated?
Treatment for coronary artery spasm centers on easing chest pain and preventing future episodes. Prescription medications commonly include:
- Nitrates, which help widen the arteries and relax arterial walls. They may be prescribed for ongoing use or taken as needed when symptoms arise.
- Calcium channel blockers, which reduce chest tightness by relaxing the smooth muscles within the arteries. These are often used as long-term therapy to decrease the frequency of spasms.
Your doctor may also prescribe medications to control high cholesterol or high blood pressure. Proper management of these conditions can significantly reduce the risk of another coronary artery spasm or a heart attack.
Lifestyle adjustments play a vital role in treatment. A heart-healthy diet that is low in saturated fat and sodium can support vascular health. Regular physical activity—approved by your healthcare provider—improves circulation and endothelial function. If you smoke, quitting is one of the most important steps you can take to decrease oxidative stress and protect your arteries.
What are the potential complications of a coronary artery spasm?
Although coronary artery spasms are typically brief, they can lead to serious and lasting consequences if not properly managed. Repeated or prolonged spasms may reduce oxygen supply to the heart muscle and increase the risk of:
- heart arrhythmias, which occur when your heart beats irregularly or too fast or too slow
- heart attacks, which occur when there’s a complete blockage of blood flow to your heart
- cardiac arrest, which occurs when your heart stops beating suddenly because blood stops flowing to your brain
- death
Prompt diagnosis and consistent treatment are essential to minimize these risks and protect overall cardiovascular health.
What is the outlook for people with coronary artery spasms?
Coronary artery spasms are generally considered chronic conditions, meaning they may recur over time rather than resolve completely. However, with appropriate medical therapy, trigger avoidance, and ongoing monitoring, many people achieve good symptom control.
Adhering to your prescribed treatment plan and maintaining regular follow-up appointments can significantly improve long-term outcomes. Early intervention and proactive lifestyle management play key roles in reducing future complications.
How can I prevent a coronary artery spasm?
Lowering your risk of coronary artery spasm involves preventing atherosclerosis and supporting overall heart health. This includes following a low-fat, balanced diet, engaging in regular exercise, maintaining healthy blood pressure levels, and quitting smoking.
Stress management techniques—such as relaxation exercises, adequate sleep, and mindfulness practices—may also help reduce episodes triggered by emotional strain. Avoiding extreme cold and stimulant substances is equally important.
Most importantly, follow your doctor’s recommendations carefully. Consistent medical care, healthy lifestyle choices, and awareness of symptoms can greatly decrease the likelihood of further coronary artery spasms and serious heart-related complications.





















Leave a Reply
You must be logged in to post a comment.