Key takeaways
- HER2-positive breast cancer is a form of breast cancer in which cells produce excessive amounts of the HER2 protein. This overproduction leads to faster and more aggressive growth compared with HER2-negative breast cancer.
- You cannot diagnose HER2-positive breast cancer on your own. Early detection through routine screenings and timely medical evaluation of unusual breast changes is essential.
- Although HER2-positive breast cancer has historically been considered more aggressive, modern targeted therapies have greatly improved outcomes and overall prognosis.
Breast cancer is not a single condition but rather a collection of distinct diseases with different biological features.
When a diagnosis is made, one of the first and most important steps is determining the specific type of breast cancer. Identifying the subtype provides critical insight into how the cancer may grow, spread, and respond to treatment — all of which directly influence HER2 breast cancer life expectancy and long-term outlook.
According to the American Cancer Society (ACS), approximately 13 percent of women in the United States will develop invasive breast cancer during their lifetime. HER2-positive breast cancer can occur in anyone, regardless of sex.
However, it’s more likely to be diagnosed in younger women. Additionally, less than 20 percent of all breast cancer cases are classified as HER2-positive.
Below, we explore what HER2-positive breast cancer means, available treatment options, recurrence risk, and factors that influence survival rates and life expectancy.
Language matters
This article discusses HER2-positive breast cancer in people assigned female at birth. Not everyone assigned female at birth identifies as a woman. While we strive to create inclusive content for all HealthEH Readers, research studies referenced here did not include data on, or include, participants who were transgender, nonbinary, gender nonconforming, genderqueer, agender, or genderless.
What is HER2-positive breast cancer?
After a breast biopsy, the collected tissue is examined for hormone receptors (HR) and for human epidermal growth factor receptor 2 (HER2). These biological markers play a major role in breast cancer development and progression.
On pathology reports, HER2 may also be labeled as HER2/neu or ERBB2 (Erb-B2 receptor tyrosine kinase 2). Hormone receptors are identified as estrogen (ER) and progesterone (PR).
The HER2 gene produces HER2 proteins, which function as receptors on the surface of breast cells. These receptors help regulate normal cell growth and repair. When too much HER2 protein is present — a process known as overexpression — it can trigger uncontrolled cell division.
HER2-positive breast cancers generally grow and spread more rapidly than HER2-negative types. In addition to tumor grade and stage, both HR status and HER2 status guide treatment decisions and significantly affect HER2 breast cancer life expectancy.
What’s the difference between HER2-negative and HER2-positive breast cancer?
HER2 proteins influence how quickly cancer cells replicate. HER2-negative breast cancer, which is more common, means the tumor cells are not producing excessive HER2 protein.
In contrast, HER2-positive breast cancer involves a high number of HER2 receptors on cancer cells. This biological difference typically signals a more aggressive disease pattern, but it also makes the cancer eligible for HER2-targeted therapies that can dramatically improve outcomes.
What causes HER2-positive breast cancer and who’s at risk?
According to research published in 2019, HER2-positive breast cancer tends to be diagnosed more often in younger women compared with HER2-negative disease. Although the precise cause is unknown, several risk factors may increase the likelihood of developing breast cancer:
- being female
- having a first childbirth after age 30
- being overweight
- living a sedentary lifestyle
- a history of radiation therapy to the chest
- smoking or using tobacco products
While a family history of breast cancer can raise overall breast cancer risk, HER2-positive breast cancer itself is not hereditary.
What are the symptoms of HER2-positive breast cancer?
You cannot determine HER2 status based on symptoms alone. If breast cancer is suspected, laboratory testing will confirm whether the tumor is HER2-positive.
Seek medical attention promptly if you notice any of the following symptoms:
- a new or changing lump in the breast or underarm
- clear, colored, or bloody nipple discharge
- persistent or unexplained breast pain
- skin changes such as dimpling, redness, or scaling
- inverted nipples
- swelling or changes in breast size or shape

Routine mammograms and breast exams remain essential tools for early detection, which can positively influence treatment success and long-term survival.
How is HER2-positive breast cancer diagnosed?
Diagnosis typically begins with:
- a physical examination
- a review of medical history
- imaging tests such as mammography or ultrasound
If imaging raises concern, a breast biopsy is performed to analyze tissue samples.
To determine HER2 status, doctors commonly use immunohistochemistry (IHC) testing, which is the preferred method. Although all breast cells contain HER2 proteins, an abnormally high level may indicate HER2-positive breast cancer and a higher likelihood of metastasis.
IHC results are graded as:
- 0 to 1+ IHC: HER2-negative
- 2+: equivocal, requiring further testing
- 3+: HER2-positive
Breast cancer is also staged from 0 to IV based on tumor size, lymph node involvement, receptor status, and spread to distant organs. Stage at diagnosis plays a major role in determining prognosis and HER2 breast cancer life expectancy.
How is HER2-positive breast cancer treated?
Although HER2-positive breast cancer is biologically aggressive, treatment options have expanded significantly. Therapy usually combines multiple approaches, including:
- surgery
- radiation therapy
- chemotherapy
- targeted treatments
If the cancer is also HR-positive, hormone therapy may be recommended.
Because targeted therapies specifically attack HER2 protein pathways, they have substantially improved survival rates. Many people newly diagnosed understandably ask whether this condition is fatal. For more insight, see Is HER2-positive breast cancer: a death sentence, which explores prognosis in detail.
Targeted treatments
Targeted drugs focus on HER2-expressing cancer cells while sparing most healthy tissue. This precision often results in fewer side effects compared with traditional chemotherapy.
Trastuzumab (Herceptin)
Trastuzumab binds directly to the HER2 protein, blocking signals that stimulate tumor growth. It was the first therapy approved to specifically target HER2-positive breast cancer and marked a major advancement in care.
According to research, combining trastuzumab with chemotherapy is associated with longer survival, lower 1-year death rates, prolonged disease-free progression, and higher response rates.
Pertuzumab (Perjeta)
Pertuzumab attaches to a different region of the HER2 protein and is frequently administered intravenously alongside trastuzumab to enhance effectiveness.
Ado-trastuzumab emtansine (Kadcyla)
This intravenous therapy links trastuzumab with the chemotherapy agent emtansine, delivering treatment directly into HER2-positive cells. It may be used in metastatic disease or when residual disease remains after initial therapy.
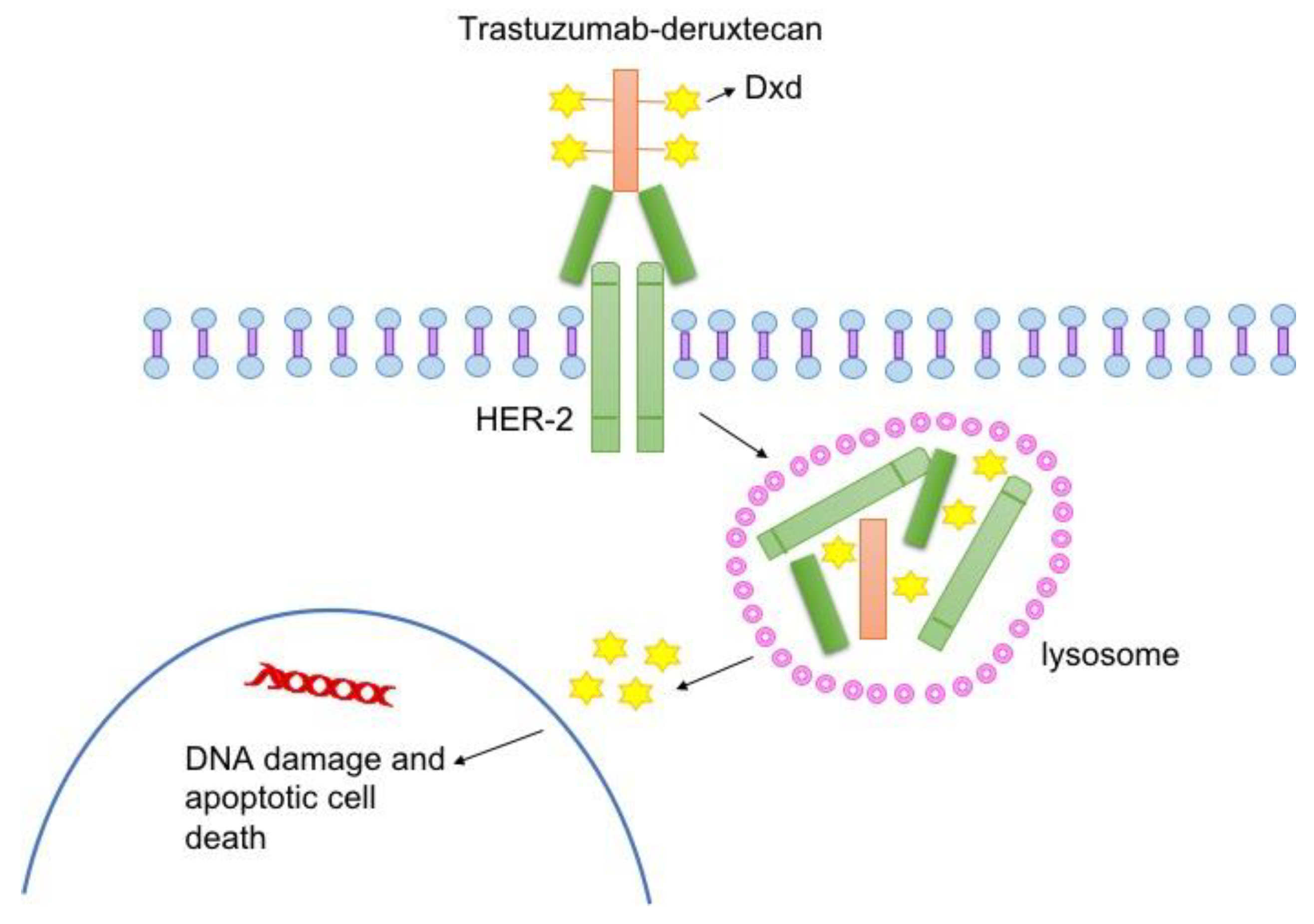
Fam-trastuzumab deruxtecan (Enhertu)
Approved by the FDA in 2019, fam-trastuzumab deruxtecan combines trastuzumab with deruxtecan. It is used when cancer has spread or progressed despite previous HER2-targeted therapies.
Neratinib (Nerlynx)
Neratinib is taken for one year in early-stage HER2-positive breast cancer after completing trastuzumab. It works inside cancer cells to disrupt growth signals and reduce recurrence risk.
Lapatinib (Tykerb)
Lapatinib blocks proteins responsible for uncontrolled cell growth and may be combined with chemotherapy or hormonal therapy for metastatic disease.
Tucatinib (Tukysa)
FDA approved in 2020, tucatinib is used with trastuzumab and capecitabine for advanced or metastatic HER2-positive breast cancer.
Is HER2-positive breast cancer curable?
In oncology, the term “remission” is more commonly used than “cure.” Complete remission means no detectable signs of cancer remain. If complete remission lasts 5 years or more, a physician may consider the cancer cured.
However, microscopic cancer cells can sometimes persist, which is why long-term monitoring is essential. Some individuals with metastatic HER2-positive breast cancer have even achieved complete remission, demonstrating how significantly therapies have evolved.
What’s the life expectancy and outlook for HER2-positive breast cancer?
Understanding HER2 breast cancer life expectancy involves evaluating stage at diagnosis, response to treatment, overall health, and access to targeted therapies.
In 2022, the ACS estimated that more than 43,250 women in the United States would die from breast cancer. Yet survival outcomes continue to improve, particularly for HER2-positive disease due to modern treatment advances.
HER2-positive breast cancers may grow quickly, but they are also highly responsive to HER2-targeted medications, which has transformed prognosis over the past two decades. Stories like the Longest HER2 breast cancer survivor highlight how dramatically survival expectations have shifted.
5-year survival rates for all breast cancers
Survival statistics are typically reported over a 5-year timeframe. While no data isolate HER2-positive cases alone, the following 5-year relative survival rates (2011–2017) from the NCI apply to breast cancer overall:
| Stage at diagnosis | 5-year relative survival rate |
| Localized | 99 percent |
| Regional | 85.8 percent |
| Distant (or metastatic) | 29 percent |
| All stages combined | 90.3 percent |
These figures are population-based and cannot predict an individual’s outcome. Additionally, treatment strategies continue to evolve, meaning current HER2 breast cancer life expectancy may be better than historical statistics suggest.
Can HER2-positive breast cancer recur after treatment?
HER2-positive breast cancer has a higher recurrence risk than HER2-negative disease, particularly within the first 5 years after treatment. Fortunately, recurrence rates have declined due to effective targeted therapies.
If the cancer is also HR-positive, hormone therapy can further decrease recurrence risk. Should recurrence occur, the tumor is retested because HR and HER2 status can change, influencing future treatment decisions.
Finding support for those with HER2-positive breast cancer
Emotional and practical support is vital. In addition to family and friends, connecting with support groups — online or in person — can provide encouragement and shared understanding.

- Cancer Care
- Cancer Survivors Network
- HER 2 Positive Breast Cancer Support and Awareness Group
- Breast Cancer Helpline
- Young Survival Coalition
Takeaway
More than 3.8 million women in the United States are living with a history of breast cancer.
The outlook for HER2-positive breast cancer continues to improve as targeted therapies advance. HER2 breast cancer life expectancy depends heavily on stage, tumor biology, and response to treatment, but many people experience long-term remission.
After completing treatment for nonmetastatic disease, ongoing monitoring is essential to detect recurrence early. For metastatic breast cancer, treatment focuses on symptom management and disease control, often with multiple lines of therapy available over time.
With continuous medical innovation and personalized treatment strategies, the prognosis for HER2-positive breast cancer is more hopeful than ever before.

















Leave a Reply
You must be logged in to post a comment.