Calcium in more than your bones
Calcium is the most plentiful mineral in your body and circulates continuously in your blood. It plays vital roles in muscle function, the nervous system, blood flow, and digestion. Yet when calcium accumulates in soft tissues where it doesn’t belong, it can cause pain and might indicate an underlying issue.
Some people try dietary or lifestyle adjustments to ease symptoms. Others turn to supplements hoping they will directly dissolve the calcium deposits. There is limited research supporting the efficacy of such supplements.
To help you weigh options, read on to learn about common types of calcium deposits in the body and the treatments that may be considered.
Achilles tendon ossification symptoms and treatments
Achilles tendon ossification (ATO) is a uncommon disorder in which calcium accumulates in the tendon that links your heel to the lower leg. The principal signs are pain and swelling around the heel and ankle, often accompanied by a lump near the heel. It can affect one or both sides.
Although ATO’s exact cause is unclear, trauma from surgery or injury is a frequent contributor. Systemic illnesses, metabolic disorders, and infection may also play roles. One case report even suggests a possible genetic predisposition.
ATO treatments
If pain is intense or the tendon has fractured, surgical intervention may be advised.
Surgery for ATO aims to excise the tendon portion where ossification has occurred while maintaining its function. This sometimes necessitates reconstructing the tendon.
A recent account describes a case in which a dermal regenerative matrix—a product designed to support tissue repair—was used to encourage Achilles tendon regeneration. After the operation, the individual wore a cast on the foot and ankle for six weeks, with changes every two weeks.
They were then allowed to use a controlled-weight walking boot to partially bear weight. By about 14 weeks, they could walk without the boot.
Calcinosis cutis symptoms and treatments
Calcinosis cutis describes calcium deposits beneath the skin. This can appear anywhere on the body. A rare variant can develop on the face or upper torso after acne.
These deposits typically show up as whitish nodules on the skin. They may be asymptomatic or can become tender and discharge a chalky, cream-like substance that is largely calcium.
Causes of calcinosis cutis
Causes of calcinosis cutis fall into four main categories:
- Dystrophic calcinosis cutis refers to deposits arising from local damage such as trauma, acne, varicose veins, infections, or connective tissue disease.
- Metastatic calcinosis cutis can stem from overactive parathyroid, internal malignancy, bone-destructive disease, excessive vitamin D intake, sarcoidosis, or chronic kidney failure.
- Iatrogenic calcinosis denotes calcium deposits that result from medical interventions like calcium injections or repeated heel pricks in newborns.
- Idiopathic calcinosis is labeled when no cause can be identified; it’s usually localized to a single area.
Calcinosis cutis treatments
Treatment hinges on uncovering and addressing the root cause. After that, your physician may prescribe medications to ease symptoms. Options include corticosteroids, magnesium supplements, and aluminum-containing antacids, though these often have limited effect.
Surgical excision may be recommended if the calcinosis repeatedly becomes infected, causes severe pain, or limits movement.
Your doctor might refer you to other specialists such as a nephrologist (kidney expert), rheumatologist (connective tissue specialist), or hematologist (blood disorders specialist).
Learn more about conventional and complementary approaches to managing calcinosis cutis.
Diagnosing calcinosis cutis
Because calcinosis cutis usually signals another condition, your physician will review your medical history and run tests to identify potential causes. Blood tests can reveal metabolic irregularities that might generate excess calcium.
A biopsy may be performed to confirm calcinosis cutis. During a biopsy, a local anesthetic is used and a small piece of skin and underlying tissue is removed.
In the uncommon event the deposit is on the face, the clinician will assess whether you previously had acne.
If acne scarring is present, a punch biopsy may be used to evaluate deeper skin layers for calcium and to exclude more serious connective tissue disease.
A punch biopsy is typically done in the clinic with a small cylindrical cutter. After numbing the area, the clinician removes lower skin layers. One or two stitches may be required. The procedure usually takes about 15 minutes.
Calcific tendonitis symptoms and treatments
Calcific tendonitis is the pathological accumulation of calcium within muscles or tendons. Although it can occur throughout the body, it most commonly affects the rotator cuff in the shoulder. This condition is often referred to as calcium deposits in the shoulder.
Calcific tendonitis symptoms
The hallmark is intense, sometimes incapacitating, pain. It can arise without an obvious trigger, frequently in the morning, and may be accompanied by stiffness or frozen shoulder.
Possible contributors include genetic susceptibility, thyroid dysfunction, and diabetes.
Calcific tendonitis treatments
Most cases are managed without surgery. Physicians typically recommend physical therapy and over-the-counter pain relievers. For severe pain and swelling, an in-office corticosteroid injection may be offered.
Other nonoperative options include:
- Extracorporeal shock wave therapy (EWST). A handheld device delivers focused mechanical pulses to the shoulder. This may be repeated weekly for three sessions.
- Radial shock wave therapy (RSWT). Similar to EWST, this uses a device to provide medium-energy mechanical impulses.
- Therapeutic ultrasound. A small device emits high-frequency sound waves to help fragment the calcium deposit.
- Percutaneous needling. With local anesthesia and ultrasound guidance, a needle is used to aspirate or break up the deposit beneath the skin.
If surgery becomes necessary, two approaches are available:
- In open surgery, the surgeon makes an incision and manually removes the calcium buildup.
- In arthroscopic surgery, a tiny incision allows insertion of a camera to guide small instruments to excise the deposit.
Recovery varies with the amount and size of deposits. Some patients regain normal motion within a week; others may experience post-operative discomfort for a longer period.
Breast calcification symptoms and treatment
Breast calcifications are detected in roughly half of women over 50 and in about 10 percent of younger women, according to Harvard Medical School. Most are benign, although they can sometimes be associated with breast cancer. They are usually found incidentally on mammograms since they typically don’t cause symptoms.
Calcifications in the breast can form as a response to tissue injury.
There doesn’t seem to be a link between taking calcium supplements and developing these deposits.
Diagnosing breast calcification
If calcifications are seen on a mammogram, the radiologist and your physician will assess whether they seem benign or suspicious for cancer.
Calcifications can form in the lobules and ducts where milk is produced and transported to the nipple. Deposits in the lobules are almost always noncancerous, whereas those in the ducts may occasionally indicate ductal carcinoma in situ (DCIS), an early-stage breast cancer.
If there’s any concern about malignancy, your doctor will recommend a biopsy.
Biopsy types
There are several biopsy methods:
A core biopsy uses a hollow needle under local anesthesia to obtain a tissue sample for microscopic analysis.
Stereotactic biopsy is a core biopsy guided by stereoscopic X-ray to precisely target the area. It’s minimally invasive and done with local anesthesia.
A vacuum-assisted biopsy employs mammography or ultrasound guidance and a hollow probe inserted through a small incision to collect samples after numbing the area.
Wire localization helps identify the exact portion to be surgically removed for examination. It’s more invasive and considered a surgical procedure.
With wire localization, a radiologist inserts a fine wire into the breast under imaging guidance after local anesthesia. The wire remains until the targeted tissue is surgically excised, usually the same day or the next day. You might experience some discomfort while the wire is in place.
The follow-up excision is performed under general or local anesthesia, and some soreness afterward is common.
Breast calcification treatment
Most evaluations and biopsies reveal benign findings. However, if a biopsy identifies early cancerous changes, your medical team will discuss what that means and your treatment choices.
Any breast lump should be assessed by a physician irrespective of your assumptions about its cause. If benign calcifications bother you—interfering with clothing or causing concern—ask your doctor about removal, which is often done in an office or outpatient setting.
Benign breast calcifications do not raise your risk of breast cancer. About 95 percent of women with mammographic abnormalities do not have breast cancer.
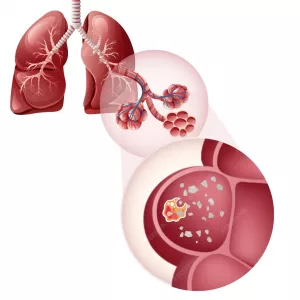
Cardiovascular calcification symptoms and treatments
Cardiovascular calcification refers to calcium build-up within plaque that can form after damage to the artery or vein wall. These are known as calcified plaques.
Calcified plaques increase the likelihood of coronary artery disease, which can cause chest discomfort. Calcification in the carotid arteries of the neck or vertebral arteries of the spine may raise stroke risk.
Cardiovascular calcification treatments
If you have arterial calcification, your risk for heart disease is elevated.
When chest pain arises, your physician may order a coronary artery scan (also called a heart or calcium scan) to detect excess arterial calcium. The test uses a CT scanner to produce a three-dimensional image.
Calcium in the arteries is not always alarming. A cardiologist can evaluate your overall risk of heart attack, advise whether a coronary calcium scan is appropriate, and recommend optimal treatment.
There is some evidence that supplemental vitamin K-2 might reduce calcium-related cardiovascular risks. Check with your doctor for current guidance on taking this supplement.
Meanwhile, there are immediate heart-healthy steps you can take at home before seeing a physician.
Kidney stone symptoms and treatments
Kidney stones are most commonly composed mainly of calcium. Your kidneys filter roughly 10 grams of calcium daily. Passing a kidney stone from the kidney through the urinary tract to the bladder can be extremely painful.
Symptoms include reduced urine flow, intense flank pain, and pain during urination.
Diagnosing kidney stones
Your doctor will analyze blood and urine and review your diet. Kidney stones with elevated urinary calcium can signal bone calcium loss.
Research suggests that reducing dietary calcium might paradoxically raise kidney stone risk. In contrast, Harvard researchers found women who consumed calcium-rich diets had a 40 percent lower risk of kidney stones.
High calcium levels in both blood and urine may point to an overactive parathyroid. Hyperparathyroidism is linked to kidney stones, cardiovascular disease, and osteoporosis.
Kidney stones treatment
If you have kidney stones along with high urinary calcium, your doctor may prescribe a thiazide diuretic. This medication helps retain calcium in bones rather than allowing it to be lost in urine.
For more on related issues, including how to manage gallstones naturally, see how to get rid of gallstones.
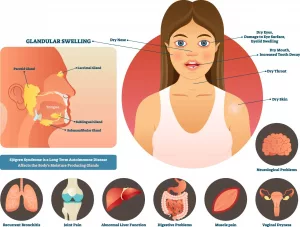
What is dermatomyositis?
Dermatomyositis, sometimes referred to within the CREST spectrum, is not solely a calcium-deposit disorder. It’s an inflammatory condition that causes a violet or deep red rash, usually on the face or upper torso. Firm calcium deposits beneath the skin can occur as part of this syndrome.
Although uncommon, dermatomyositis can affect both adults and children.
Warnings about dimethyl sulfoxide
Some claim dimethyl sulfoxide (DMSO) dissolves calcium deposits, but DMSO is not approved for that use.
The U.S. Food and Drug Administration has approved DMSO only for treating interstitial cystitis, a chronic inflammatory bladder condition.
Read about potential risks and benefits before considering DMSO.
Q&A
Q:
What is DMSO? And is it safe for use at home?
A:
DMSO is a byproduct of wood pulp and paper manufacturing. It’s a solvent that penetrates skin and cells readily, so it appears in topical formulations. It has anti-inflammatory properties, acts as an antioxidant by neutralizing free radicals, and is sometimes used to protect tissues during chemotherapy or freezing. Nevertheless, the FDA’s only approved application is as a bladder instillation for urinary tract issues.
DMSO can interact with other medicines, even when applied topically. Avoid DMSO if you are pregnant, trying to conceive, or breastfeeding. Allergic reactions are possible.
There’s limited research supporting at-home use, though additional applications may emerge over time. DMSO is often used in sports first aid for sprains and strains and as a vehicle to boost absorption of other topicals. If you try DMSO, follow label warnings, avoid applying it to open wounds, and never ingest it. Choose a reputable product, and perform a patch test to check for allergy. It may be a useful adjunct for chronic pain management for some people.
The bottom line
Calcium is an essential mineral that can deposit in diverse organs throughout the body. Most resulting conditions are benign and manageable, though some require surgery or signal more serious underlying disease.

















Leave a Reply
You must be logged in to post a comment.