Key takeaways
- Foods high in calcium, magnesium, and selenium may help promote bone strength and overall well-being with Graves’ disease, in addition to standard medical care.
- Excess iodine may aggravate hyperthyroidism symptoms in Graves’ disease, so it may be helpful to monitor iodized salt, seafood, seaweed, and iodine-containing supplements with your clinician.
- If you also have celiac disease, eliminating gluten may reduce autoimmune reactions, and using a food diary can help pinpoint individual dietary triggers.
Graves’ disease is an autoimmune condition that leads to hyperthyroidism, a disorder in which your thyroid gland produces excessive thyroid hormones.
When people share stories such as “I cured my Graves’ disease,” they often describe a combination of medical treatment and meaningful lifestyle adjustments. While antithyroid medications and radioactive iodine (RAI) ablation remain the cornerstone of care, targeted nutrition strategies may also help maintain remission and enhance overall health.
Diet alone is not considered a cure. However, optimizing nutrient intake, identifying food sensitivities, and supporting bone and thyroid health can be valuable parts of a comprehensive plan. If you’ve ever thought, “I cured my Graves’ disease by changing my diet,” it’s important to understand how dietary measures complement — rather than replace — evidence-based treatment.
Continue reading to explore which foods may be beneficial and which may need to be limited if you’re living with Graves’ disease.

A note on diet and Graves’ disease
Certain nutrient-dense foods may assist in managing symptoms associated with Graves’ disease, particularly those affecting bone density, inflammation, and immune balance.
That said, research specifically evaluating diet as a primary therapy for Graves’ disease remains limited. Most current recommendations focus on supportive nutrition rather than dietary cures.
Before making major dietary changes, consider consulting a healthcare professional or a registered dietitian experienced in autoimmune thyroid conditions. Personalized guidance is especially important if you are adjusting medications, monitoring thyroid hormone levels, or managing related concerns such as thyroid eye disease.
Foods to eat
The following foods may support symptom management and overall wellness in Graves’ disease.
Calcium-rich foods
Hyperthyroidism may increase bone resorption and osteoclastic activity. These are normal components of bone remodeling, but when overactive, they can raise the risk of reduced bone mineral density, brittle bones, and osteoporosis.
Ensuring adequate calcium intake is essential for protecting skeletal health. However, some dairy products rich in calcium may also contain iodine, and excessive iodine intake may lead to worsening symptoms in people with hyperthyroidism.
For this reason, you may consider incorporating non-dairy calcium sources such as:
- broccoli
- kale
- okra
- chia seeds
- sardines
- salmon
- soybeans and tofu
A physician or dietitian can help you determine which dairy options are appropriate and whether fortified alternatives are suitable for your needs. Monitoring bone health is particularly important for those who have experienced prolonged hyperthyroidism.
Foods high in magnesium
Magnesium plays a key role in cellular function. If your magnesium levels are insufficient, it can affect its ability to regulate calcium and potassium transport across cell membranes. These minerals are crucial for maintaining bone integrity, muscle function, and cardiovascular stability.
Magnesium-rich foods include:
- pumpkin seeds
- chia seeds
- spinach
- almonds
- dark chocolate
- brazil nuts
- cashews
- legumes
- avocados
- chicken breast
Including a variety of whole foods that supply magnesium may help counteract mineral imbalances sometimes seen in hyperthyroidism.
Foods containing selenium
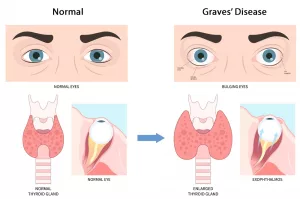
Some researchers hypothesize that selenium deficiency may be linked to thyroid eye disease in individuals with Graves’ disease. Thyroid eye disease can lead to symptoms such as bulging eyes and double vision.
Selenium is both an antioxidant and an essential mineral involved in thyroid hormone metabolism. It can be found in:
- brazil nuts
- brown rice
- sunflower seeds
- sardines
- tuna
- shrimp
- turkey
Adequate selenium intake may support thyroid function and immune regulation. However, supplementation should only be considered under medical supervision, as excessive selenium can be harmful.
Foods to avoid or limit
Although certain nutrients may worsen symptoms of Graves’ disease, it’s essential to speak with a healthcare professional before removing entire food groups. Unnecessary restrictions can increase the risk of nutrient deficiencies, especially in autoimmune conditions.
Keeping a detailed food diary can help you track what you eat, portion sizes, and any symptoms that follow. This approach may assist in identifying personal triggers and patterns. Some individuals who once believed “I cured my Graves’ disease” later recognized that symptom improvement came from careful monitoring, medical treatment, and dietary awareness combined.
You may consider evaluating the following categories with your clinician:
Gluten
According to a 2022 study, autoimmune thyroid disease occurs more frequently in people with celiac disease compared to the general population. This association may partly reflect a shared genetic predisposition.
In celiac disease, consuming gluten triggers an autoimmune response that damages the intestinal lining and interferes with nutrient absorption.
If you have both Graves’ disease and celiac disease, a doctor may advise avoiding gluten-containing foods such as:
- wheat and wheat products
- rye
- barley
- malt
- triticale
- brewer’s yeast
- grains, such as spelt, kamut, farro, and durum
Eliminating gluten without a confirmed diagnosis is generally not recommended unless directed by a healthcare professional.
Dietary iodine
The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) explains that excessive iodine intake may trigger hyperthyroidism in individuals with Graves’ disease.
At the same time, iodine is an essential micronutrient required for normal thyroid hormone production and overall health. The goal is balance — not complete elimination.
Iodine-fortified products include:
- salt
- foods made with iodine-fortified salt
Naturally iodine-rich foods may include:
- fish, particularly white fish such as haddock and cod
- oysters
- seaweed and kelp
Certain medications and multivitamins may also contain iodine. Your doctor can help determine whether your iodine intake requires adjustment based on your thyroid function tests and treatment plan.
Meat and animal products
An older 2014 study reported that vegetarians had lower rates of hyperthyroidism than non-vegetarians. The greatest difference was observed among those who avoided animal products such as:
- beef
- chicken
- pork
- fish
However, a 2024 review indicates that strict plant-based diets may elevate the risk of deficiencies in nutrients relevant to Graves’ disease, including selenium, which is commonly found in animal-derived foods.
For some individuals, a Mediterranean diet may offer a balanced approach. A 2023 review suggests that this dietary pattern may provide protective effects against autoimmune hyperthyroidism, though further research is necessary.
This style of eating emphasizes:
- vegetables
- whole grains
- fruit
- moderate amounts of fish and seafood
- olive oil
- limited intake of meat, processed foods, and alcohol
If you’re navigating significant symptoms or emotional challenges, you may relate to stories like Graves’ disease ruined my life. Learning about the Life expectancy of someone with Graves’ disease and understanding modern treatment outcomes can also provide reassurance and perspective.
The bottom line
Graves’ disease is one of the most common causes of hyperthyroidism. Healthcare professionals may suggest dietary adjustments to help support overall wellness if you are living with this autoimmune thyroid condition.
A nutrient-dense eating pattern rich in colorful fruits and vegetables, adequate minerals such as calcium, magnesium, and selenium, and mindful iodine intake may complement medical treatment.
Collaborating with a doctor or registered dietitian — and maintaining a detailed food diary — can help you identify which foods to prioritize and which to limit, ensuring your nutrition plan supports both thyroid health and long-term well-being.

















Leave a Reply
You must be logged in to post a comment.