- Individuals with POTS are more prone to migraines; research estimates that between 41% and 96% of people with POTS also suffer from chronic migraine.
- When managing migraine in people with POTS, it’s crucial to recognize that some commonly used migraine drugs may aggravate POTS symptoms.
- To reduce migraine occurrence, people with POTS should try to pinpoint and avoid triggers, keep a consistent sleep routine, and engage in regular physical activity if tolerated.
If you have postural orthostatic tachycardia syndrome (POTS), there’s a strong possibility you also deal with migraine. Several studies have linked POTS with chronic migraine at rates reported between 41% and 96% of affected individuals.
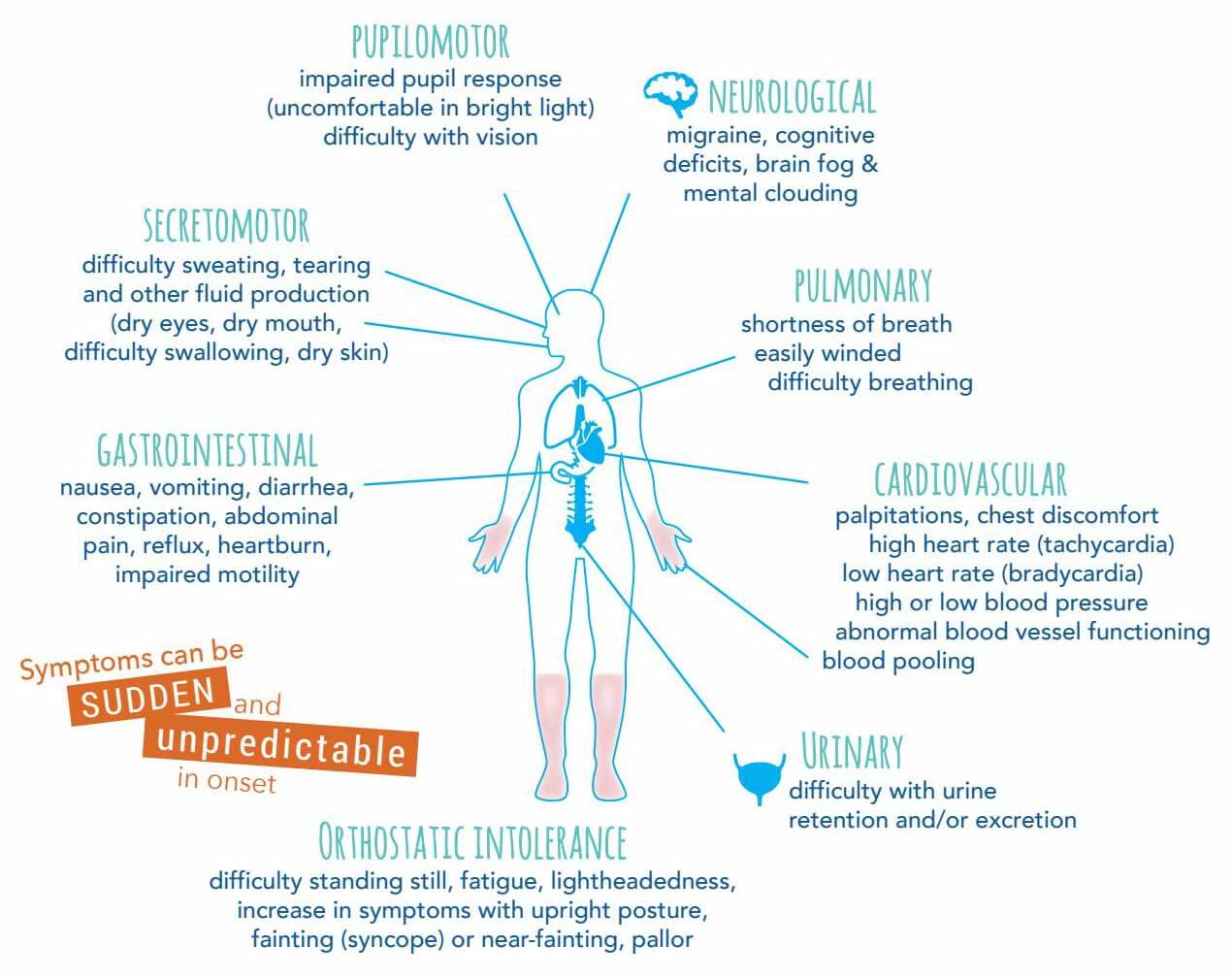
Both migraine and POTS can interrupt everyday life and produce pain and exhaustion. Read on to understand migraine symptoms and how clinicians approach migraine treatment in people who have POTS.
What does a POTS flare-up feel like?
POTS is a condition that causes orthostatic intolerance — meaning you may feel dizzy or faint when you stand. POTS typically triggers a heart rate rise of more than 30 beats per minute.
Although orthostatic intolerance is the hallmark sign, other symptoms can occur, such as:
- dizziness
- fainting episodes
- profound tiredness
- sleep disturbances
- chest discomfort
- shortness of breath
These complaints generally improve when you lie down.
What causes migraine in people with POTS?
The exact reason why people with POTS often also have migraine isn’t fully understood. It’s clear, however, that women are more likely to experience both disorders.
A 2020 review found that women with POTS report migraine at higher frequencies than women without POTS.
POTS can alter autonomic nervous system function. Migraine represents an atypical processing of nervous system signals. Both disorders may reflect underlying changes in how the nervous system “communicates.”
How do I know if I have migraine?
It can sometimes be tricky to distinguish migraine from other headache types. Clinicians often use the mnemonic POUND to help identify migraine headaches:
- Pulsating quality
- One-day duration (though attacks can last up to 72 hours)
- Unilateral pain (one-sided)
- Nausea or vomiting
- Disabling severity
If your head pain includes four to five of these characteristics, migraine is likely. Some migraine attacks, however, may show only two or three features. Speak with your healthcare provider if you have frequent headaches.
How do doctors treat migraine in people with POTS?
There are limited clinical trials or formal guidelines specifically addressing the best migraine treatments in POTS. For that reason, clinicians typically manage migraine episodes similarly to how they treat migraine in the general population.
Still, it’s essential to inform your clinician that you have POTS. As discussed below, some medications commonly used for migraine may influence POTS-related symptoms.
That doesn’t mean migraine medications are off-limits, but it does mean being mindful of potential adverse effects.
How can people with POTS manage migraine?
Managing migraine usually involves trigger avoidance and medications to relieve or reduce attacks. However, several drugs commonly used to prevent or treat migraine have side effects that could be particularly problematic for people with POTS.
For instance, tricyclic antidepressants (TCAs) such as amitriptyline are sometimes prescribed. TCAs can produce side effects like dry mouth, fatigue, and constipation that may worsen POTS symptoms. Clinicians may opt for nortriptyline, a TCA with a milder side effect profile, instead.
Venlafaxine is another preventive option, but it can sometimes exacerbate rapid heart rate or palpitations in susceptible people.
Topiramate, used for migraine prevention, may increase brain fog or slow cognitive processing in those with POTS.
Some migraine preventive therapies that people with POTS may tolerate better include:
- beta-blockers such as metoprolol, propranolol, or atenolol
- botulinum toxin (BOTOX) injections
- cyproheptadine
- magnesium supplements
A 2018 review noted that people with POTS who have menstrual-related migraine may benefit from short-term naproxen or triptan therapy, such as zolmitriptan.
It’s also important to recognize that opioids are generally not effective for migraine. Over-the-counter analgesics like acetaminophen can be used for occasional migraine, but if you’re relying on them daily or weekly, discuss alternative strategies with your clinician.
How can people with POTS prevent migraine?
Migraine attacks often have identifiable triggers. These can include:
- consuming certain foods or drinks, such as wine, aspartame, or items with chemical preservatives — see more about foods that trigger migraines
- skipping meals or fasting
- hormonal changes, like menstruation
- stress
- intense visual stimuli, for example flashing lights
- changes in weather
Finding and avoiding your personal triggers may reduce the likelihood of an attack. Getting adequate sleep is also protective.

Exercise can lower migraine frequency, but it may be challenging for those with POTS. If you can tolerate physical activity, maintaining a regular exercise routine may improve symptoms.
Can migraine be a sign of POTS?
POTS can be challenging for clinicians to diagnose; on average it takes about 6 years for patients to receive a confirmed diagnosis. POTS often affects young women and commonly coexists with other conditions like chronic fatigue syndrome and fibromyalgia.
Although people with POTS experience migraine more frequently, most individuals first notice orthostatic intolerance. Symptoms often begin in the teenage years and include episodes of lightheadedness or fainting on standing, which tend to worsen over time.
Takeaway
POTS frequently involves headaches, including migraine. Managing and preventing migraine in POTS can be challenging, but identifying triggers and discussing tailored treatment options with your clinician can help reduce headache days.
If you have POTS and recurrent headaches, speak with your healthcare provider about strategies to lower the frequency and severity of your migraines.




















Leave a Reply
You must be logged in to post a comment.