Functional scoliosis, sometimes referred to as nonstructural scoliosis, describes an abnormal sideways curvature of the spine that does not meet the traditional criteria required for a formal scoliosis diagnosis.
To better understand this condition, it helps to review the Primary and secondary curves of the spine. The spine naturally forms front-to-back curves that support balance, flexibility, and shock absorption. However, when a lateral (side-to-side) curve develops, it can disrupt normal biomechanics and posture. In many instances of scoliosis, the precise underlying cause remains unknown.
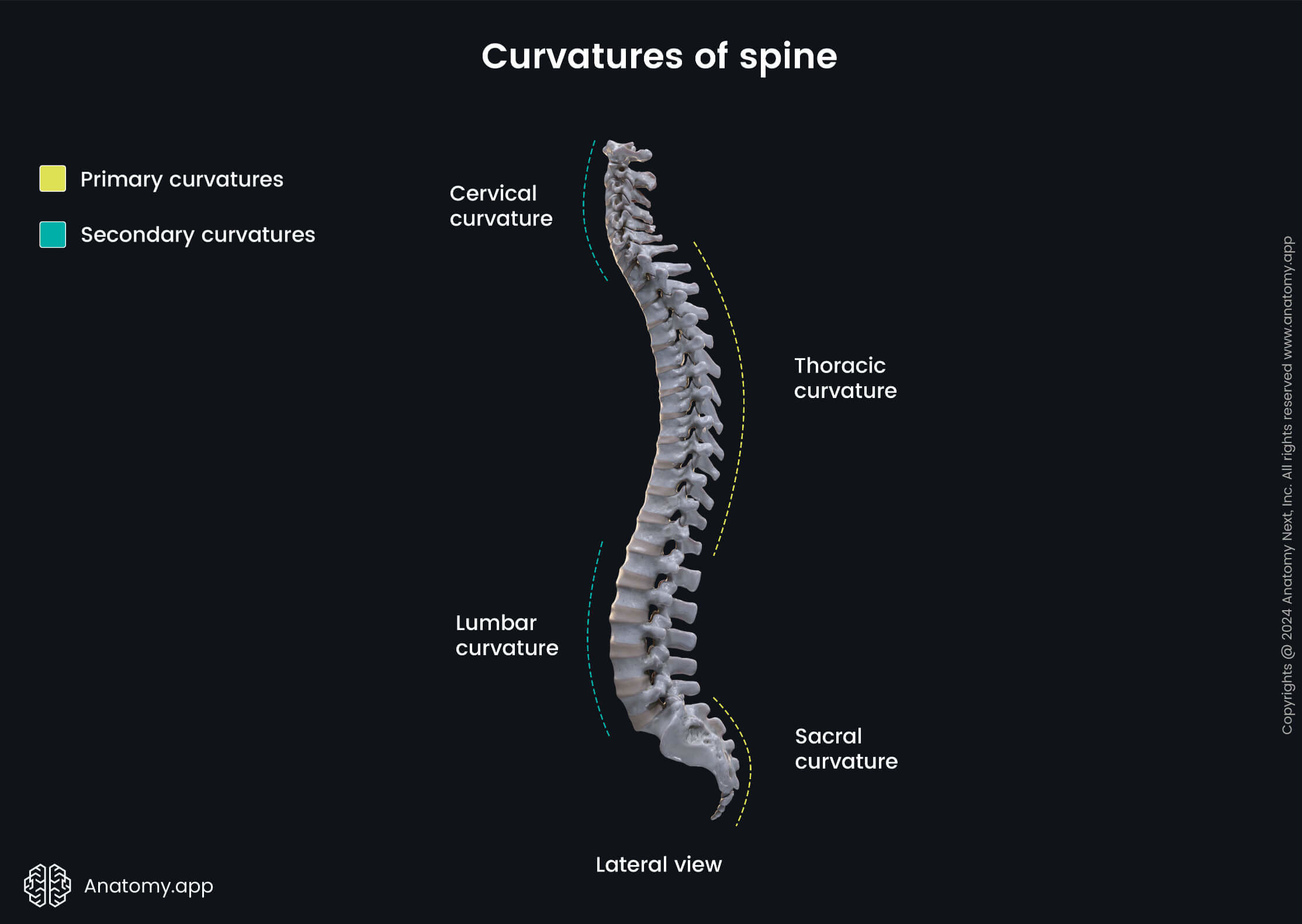
In functional scoliosis, there is no rotational deformity of the vertebrae, and the curve is usually temporary or correctable once the underlying issue is addressed.
A common finding among individuals with functional scoliosis is a difference in leg length, which can shift alignment and affect spinal positioning.
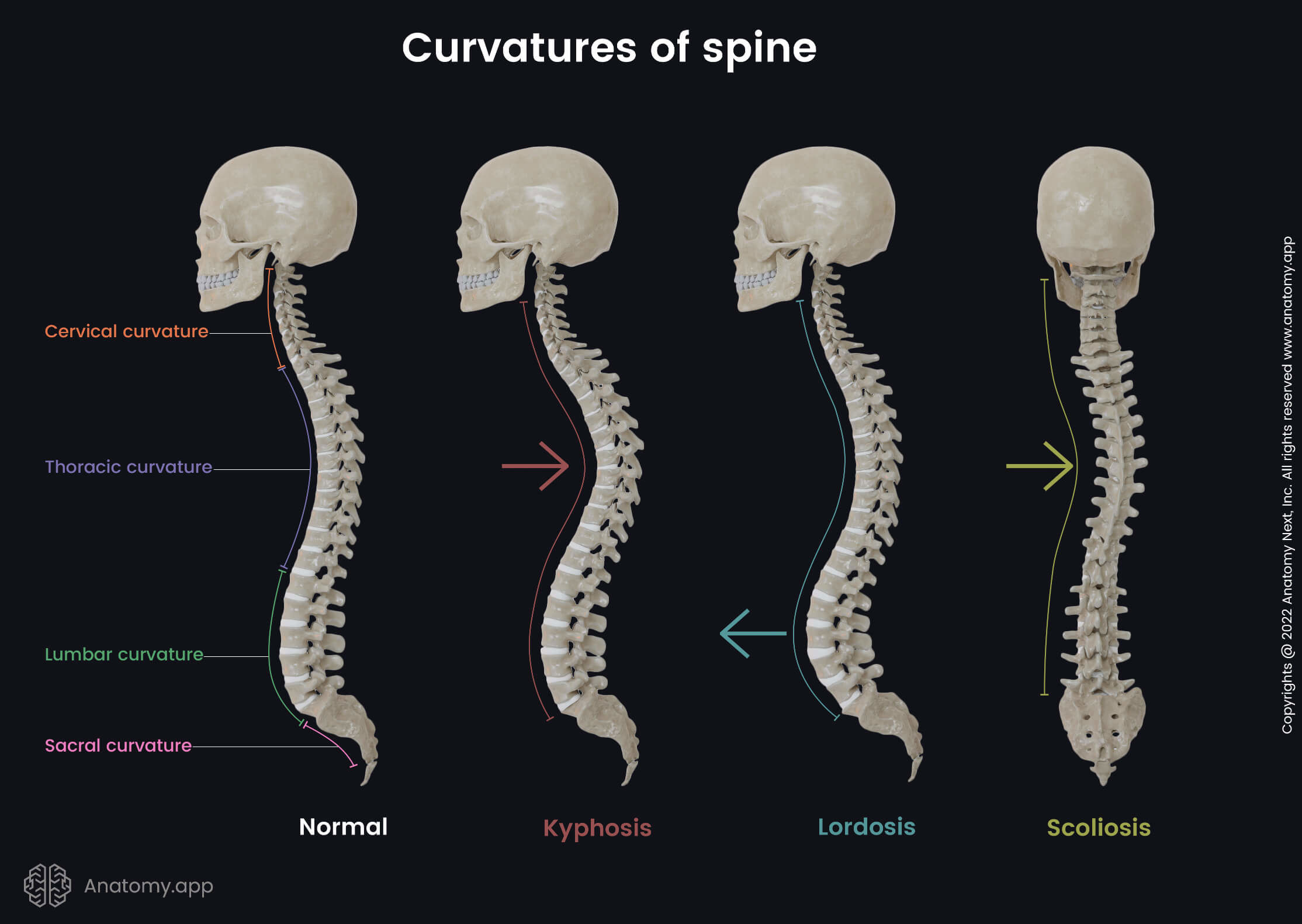
Continue reading to explore the causes, symptoms, diagnostic process, and available treatment options for functional scoliosis.
Functional scoliosis causes
A discrepancy in leg lengths is frequently the primary contributor to functional scoliosis. When one leg is shorter than the other, even slightly, the pelvis may tilt, prompting the spine to curve sideways to compensate. Other possible causes include:
- hip dysplasia (improper development of the hip socket)
- tightening of paraspinal muscles on one side
- herniated disk
- torticollis, a painfully twisted and tilted neck
- asymmetry of your upper extremities
Each of these factors can temporarily alter spinal alignment without producing a fixed structural deformity.
Who gets functional scoliosis?
Functional scoliosis is most often observed in people with unequal leg lengths. When one leg measures shorter, the pelvis may angle downward on that side, leading the spine to form a compensatory curve. This adaptation is the body’s way of maintaining upright balance.
Mild differences in leg length are relatively common. A discrepancy greater than 1 centimeter (0.45 inches) may be present in up to a third of individuals. In many cases, small variations do not result in symptoms or functional problems.
Understanding how the 4 curves of the spine interact can clarify why even subtle imbalances may influence posture and alignment over time.
Functional scoliosis symptoms
Many people with functional scoliosis experience no noticeable symptoms. The condition is often identified during a routine physical examination by a doctor or physiotherapist.
The lateral curve associated with functional scoliosis is milder than in structural forms of scoliosis. By definition, scoliosis requires a spinal curve exceeding 10 degrees for diagnosis. Functional scoliosis involves a curve measuring less than 10 degrees.
Possible visible or physical signs may include:
- a noticeable sideways curvature of the spine
- leaning more toward one side while standing
- uneven shoulder height
- ribs that protrude more on one side
In some individuals, mild back discomfort or muscle fatigue may occur, especially after prolonged standing or activity.
Potential complications of functional scoliosis
Because functional scoliosis involves asymmetry in the spine and often the pelvis, it can increase the likelihood of certain musculoskeletal concerns. These may include:
- altered biomechanics
- muscular imbalances
- joint laxity
- excessive strain on spinal joints
- excessive strain on muscles, tendons, and bones
Over time, uneven stress distribution may contribute to localized discomfort or reduced mobility if not addressed.
When to get medical help
If you suspect that you or your child may have scoliosis, consulting a healthcare professional is advisable. A doctor can measure the spinal curve to determine whether it falls outside normal limits and whether intervention is necessary.
For mild curves, monitoring alone may be recommended. Imaging such as a Normal spine curve x ray can help compare spinal alignment to typical anatomical standards.
How is functional scoliosis diagnosed?
Diagnosis typically begins with a comprehensive physical examination followed by imaging studies when appropriate.
During the physical exam, a healthcare provider will assess posture, check for leg length differences, and evaluate any visible asymmetry in the shoulders, hips, or rib cage.
A commonly used screening tool is the Adam’s forward bend test. In this assessment, you bend forward at the waist with your feet together while the clinician observes and measures any spinal deviation.
If needed, imaging tests may be ordered to confirm findings and rule out structural abnormalities. These tests can include:
- X-rays
- computed tomography (CT) scan
- magnetic resonance imaging (MRI) scan
Functional scoliosis treatment
Scoliosis management may involve conservative approaches or surgery. Since functional scoliosis does not stem from a structural defect in the vertebrae, treatment is almost always conservative and aimed at correcting the underlying cause.
Treatment strategies may include:
- observation alone
- wearing back braces
- exercises
- orthotics to correct leg length difference
Addressing leg length discrepancy with shoe lifts or custom orthotics often improves pelvic alignment and reduces the compensatory spinal curve.
Functional scoliosis exercises
Targeted exercises focusing on trunk stability and posture correction can play a significant role in managing functional scoliosis.
A healthcare provider may suggest strengthening your core and back muscles to decrease mechanical stress on the spine. Improving flexibility and muscle balance can also enhance overall spinal support. Referral to a physiotherapist is common, as they can design a personalized exercise program tailored to your specific alignment needs.
Learn more about exercises for scoliosis.
Living with functional scoliosis
Most individuals with functional scoliosis lead normal, active lives without long-term complications. The condition is typically nonprogressive and often correctable once the underlying imbalance is managed.
Maintaining strong core musculature, practicing good posture, and addressing musculoskeletal imbalances early can help preserve spinal health.
Can you prevent functional scoliosis?
The precise cause of scoliosis is frequently unclear, making prevention challenging. However, when functional scoliosis arises from modifiable factors such as muscle imbalance or leg length discrepancy, early evaluation may help reduce progression.
Adopting healthy lifestyle habits — including regular physical activity, strength training, flexibility exercises, and proper ergonomic practices — may reduce spinal stress over time. Paying attention to posture during daily activities can also support optimal alignment.
Takeaway
Functional scoliosis is a mild sideways curvature of the spine that is not caused by a structural abnormality. A discrepancy in leg lengths is often the primary trigger.
In most cases, functional scoliosis can be effectively managed with conservative treatments such as bracing, corrective exercises, and orthotics. Many people benefit from working with a physiotherapist to develop an individualized plan focused on stretching tight muscles and strengthening supportive structures around the spine.
Early assessment and appropriate intervention can help restore alignment and minimize potential musculoskeletal strain.


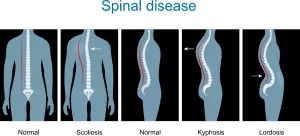



















Leave a Reply
You must be logged in to post a comment.