Mouth sores can develop for many reasons, including infections, minor injuries, and tobacco use. In some cases, reviewing Viral infection in mouth pictures can help you recognize patterns or symptoms. It’s important to seek medical care for certain sores, especially those with white patches or lesions that appear after starting a new medication.
Oral sores are very common and affect most individuals at some point in life. These lesions may form on any of the soft tissues inside the mouth, such as the lips, inner cheeks, gums, tongue, and the floor or roof of the mouth. Examining Viral infection in mouth pictures and other oral lesion images can support early identification, but a professional evaluation is still essential for diagnosis.
In many situations, mouth sores are minor irritations that resolve within 1 to 2 weeks. However, persistent or recurring lesions may signal a more serious issue, including infection or oral cancer. Understanding the different types and causes can help guide appropriate treatment and prevention.
This article explains the various forms of mouth sores, what causes them, and how they appear. Images are included to assist with visual identification, along with guidance on management and when to seek medical advice.
What do mouth sores look like?
The appearance of mouth sores varies depending on the underlying cause. They may differ in color from the surrounding tissue and can look white, yellow, red, or purple. Some lesions are flat, while others are raised, blistered, or ulcerated.
The images below illustrate several common types of mouth sores. These pictures are for educational purposes only and are not intended to provide a diagnosis. If you experience unexplained sores, frequent recurrences, or lesions that persist for an extended period, consult a healthcare professional for proper assessment and treatment.
Warning: Images of mouth sores ahead.
Canker sores
Canker sores often appear as small, oval ulcers inside the mouth. They are typically white, gray, or yellow with a red border or “halo.” Sometimes, they may present as a painful red patch before the ulcer fully develops.

Canker sores, also known as aphthous stomatitis or aphthous ulcers, are widespread and affect approximately 25% of the general population.
They are generally harmless and tend to resolve within a couple of weeks. Recurrent ulcers may be due toother conditions, such as Crohn’s disease, celiac disease, vitamin deficiency, or HIV.
Subgroups of canker sores include:
- Mild: Less than 1 centimeter in diameter and heal within 1 to 2 weeks
- Major: Deeper, larger ulcers — 2 to 3 centimeters wide — that may take weeks or months to heal
- Herpetiform: Tiny (1 to 2 millimeters) sores appearing in clusters of 10 to 100 that can require several weeks to resolve
What causes canker sores in your mouth?
Canker sores are frequently triggered by minor trauma, such as accidentally biting the cheek, burns from hot food, allergies, or sensitivities. They are not contagious. Emotional stress and immune system changes may also contribute.
Risk factors include:
- a weakened immune system due to illness or stress
- hormonal fluctuations, such as during menstruation
- vitamin deficiency, particularly folate and B12
- intestinal disorders like Crohn’s disease or ulcerative colitis, types of inflammatory bowel syndrome (IBS)
- exposure to toxins in drinking water
- smoking or a history of smoking
Cold sores
Cold sores are fluid-filled blisters that typically form around the lips or mouth. Before the blister appears, you may notice tingling, burning, or itching in the affected area. Many people search for Viral infection in mouth pictures to compare these early symptoms with visible outbreaks.


Cold sores result from the herpes simplex type 1 virus (HSV-1). During an outbreak, you may also experience mild flu-like symptoms, including low-grade fever, swollen lymph nodes, and body aches.
HSV-1 can remain dormant in the body and reactivate during times of stress or weakened immunity. Lesions typically last 1 to 2 weeks.
The virus is contagious and spreads through close contact, such as kissing or sharing utensils. Even without visible sores, transmission can occur. Genital herpes, caused by herpes simplex type 2 virus (HSV-2), may resemble cold sores and can be transmitted through sexual contact without barrier protection.
Folate deficiency and anemia
A folate deficiency occurs when the body lacks adequate folate (vitamin B9), a nutrient essential for DNA production and repair. Low folate levels can lead to folate deficiency anemia.
Anemia develops when red blood cell levels are insufficient or impaired, reducing oxygen delivery throughout the body. Both folate deficiency and anemia may cause mouth ulcers that resemble canker sores.

Symptoms of folate deficiency may include fatigue, weakness, pale skin, tongue swelling, and growth delay in children. Anemia symptoms can include dizziness, shortness of breath, pale gums, and heart palpitations.
Gingivostomatitis
Gingivostomatitis is a common infection affecting the gums and mouth, especially in children. It may cause tender gray or yellow sores with red borders. Viral causes include HSV-1 and coxsackievirus, while bacterial causes may involve Streptococcus.

Ulcers from this condition may persist for 2 to 3 weeks and can be accompanied by drooling, fever, and discomfort when eating.
Hand, foot, and mouth disease
Hand, foot, and mouth disease is caused by enteroviruses and commonly affects children under age 5. Painful red blisters may appear inside the mouth along with a rash on the hands and feet. Reviewing Viral infection in mouth pictures can help caregivers recognize this highly contagious but usually mild illness.

Symptoms often include fever and sore throat. The infection generally resolves within 7 to 10 days.
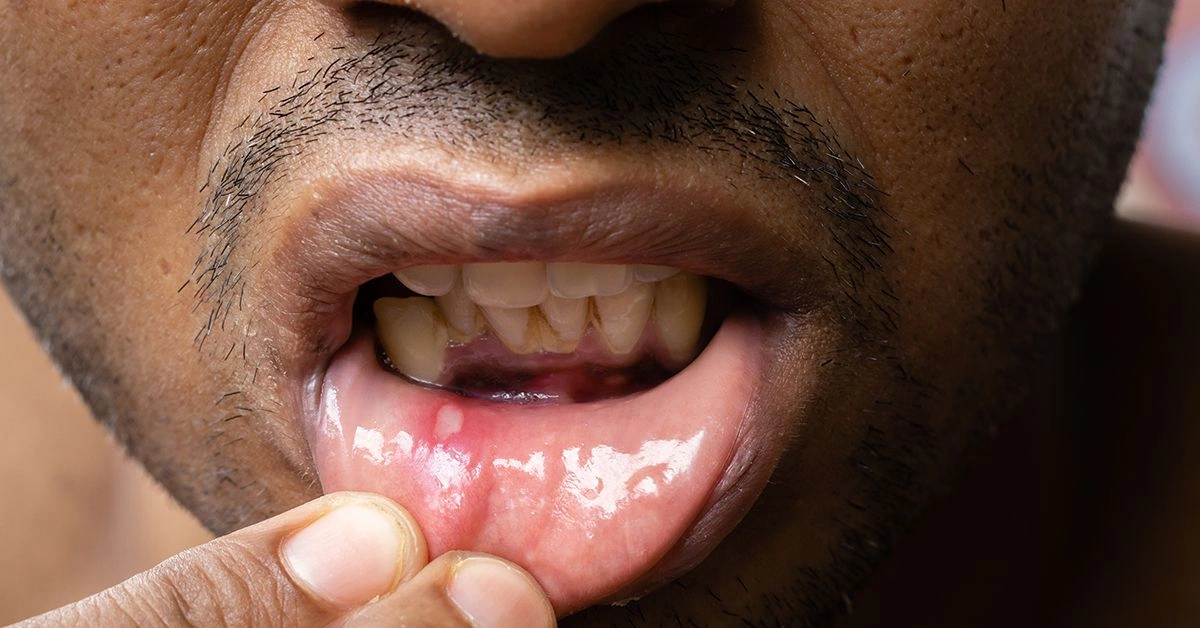
Leukoplakia
Oral leukoplakia presents as thick white patches on the tongue or inner cheeks. It is commonly associated with tobacco use.

While often benign, studies suggest 1 to 9% of individuals with leukoplakia may develop oral cancer. Regular dental evaluations can aid early detection.
Oral lichen planus
Oral lichen planus is a chronic inflammatory condition affecting mucous membranes. It may produce white, lacy patches or red swollen tissues with ulcers.

It is not contagious but is a long-term condition managed with medications such as corticosteroids.
Mouth cancer
Mouth cancer, or oral cancer, originates in the oral cavity and may appear as persistent ulcers, red patches (erythroplakia), or white patches (leukoplakia) that do not heal.

Additional symptoms may include bleeding gums, ear pain, swollen lymph nodes, and unexplained weight loss. Early biopsy and diagnosis significantly improve outcomes.
What are the symptoms of mouth sores?
Common signs include redness, pain when eating or drinking, burning sensations, and tingling. Larger or deeper lesions may interfere with swallowing or speaking.
What causes mouth sores?
Causes range from minor trauma to viral, bacterial, or fungal infections, autoimmune disorders, medication reactions, and systemic diseases. For example, some individuals experiencing Red spots on roof of mouth pictures may actually be observing viral or inflammatory changes. Others researching Red spots roof of mouth COVID may be concerned about infection-related oral symptoms.
How are mouth sores diagnosed?
Diagnosis often begins with a physical examination. Persistent white patches, worsening ulcers, or sores lasting more than two weeks warrant medical evaluation. If cancer is suspected, a biopsy may be performed.
Are there home remedies for mouth sores?
Minor sores usually heal within 1 to 2 weeks. Helpful strategies include avoiding spicy or acidic foods, rinsing with salt water, applying baking soda paste, staying hydrated, and using over-the-counter pain relievers such as acetaminophen (Tylenol).
Are there medications for mouth sores?
Treatment depends on the cause. Healthcare professionals may prescribe antiviral, antifungal, or antibacterial medications, as well as steroid gels for inflammation. Oral cancer treatment may involve surgery or chemotherapy.
Can you prevent mouth sores?
Although not all sores are preventable, risk can be reduced by maintaining good oral hygiene, using a soft toothbrush, eating a balanced diet rich in B vitamins, avoiding tobacco and excessive alcohol, managing stress, and protecting lips from sun exposure with SPF lip balm.
Takeaway
Mouth sores are common and typically resolve within 1 to 2 weeks. Reviewing Viral infection in mouth pictures and other oral lesion images may help with awareness, but persistent, painful, or recurring sores require medical evaluation. Early diagnosis ensures proper treatment and helps rule out serious conditions.



















Leave a Reply
You must be logged in to post a comment.