Treatments for hyperthyroidism are designed to reduce or halt the excessive production of thyroid hormones. If you’re wondering, Can Graves’ disease be cured, the answer depends on how “cure” is defined. While therapies can effectively control symptoms and regulate hormone levels, most people will require ongoing management or lifelong medication to maintain healthy thyroid function.
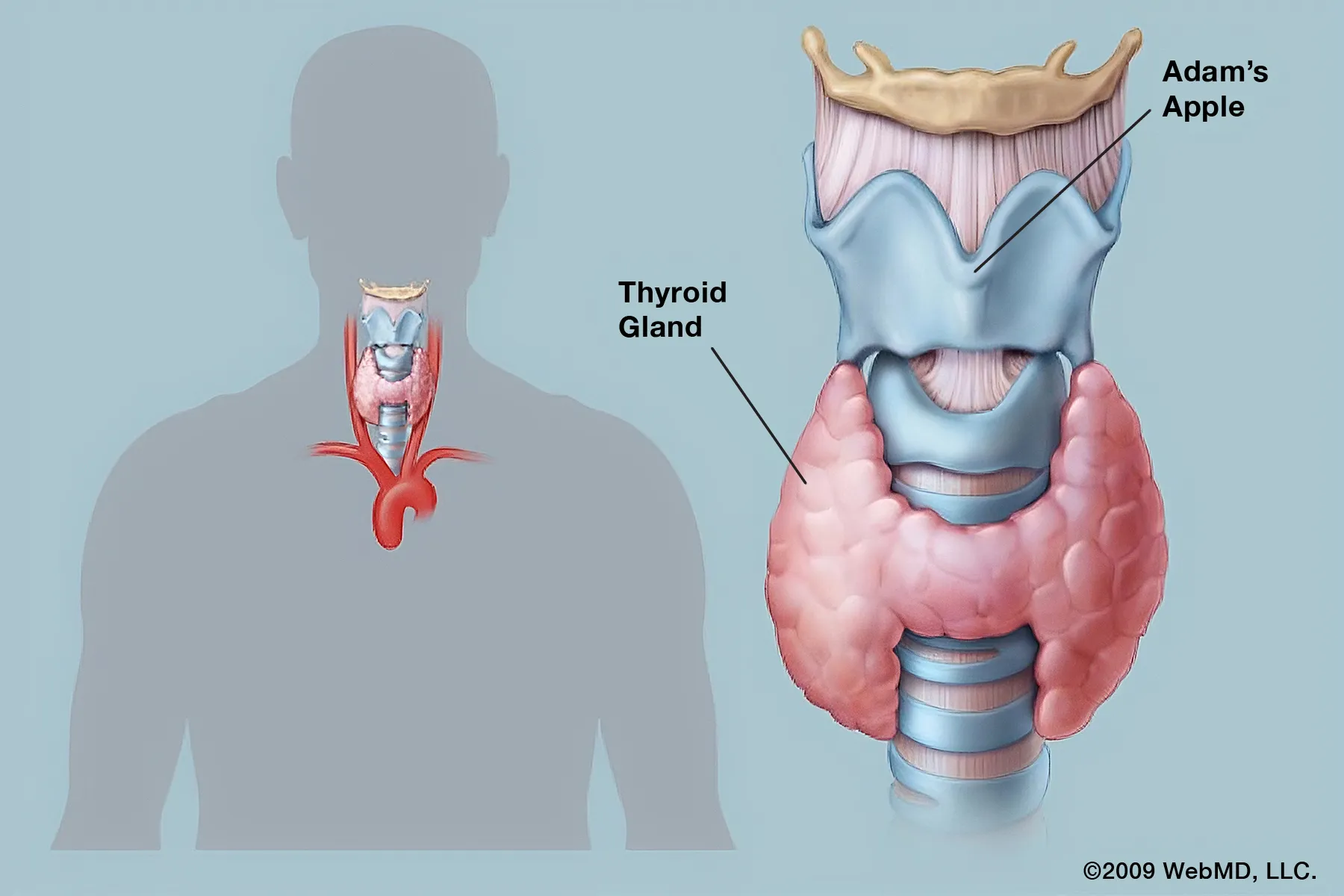
Hyperthyroidism, also known as an overactive thyroid, can be addressed through several proven treatment strategies. In some cases, symptoms may disappear entirely for a period of time. However, even when symptoms improve, continuing the recommended treatment plan is essential to prevent relapse and long-term complications.
Other treatment options work by eliminating the thyroid’s overactivity altogether, often by removing or destroying thyroid tissue. Although this approach resolves the excess hormone production, it also means you’ll need lifelong thyroid hormone replacement therapy to compensate for the loss of natural hormone production.
For individuals with autoimmune hyperthyroidism, particularly Graves’ disease, medication may sometimes induce remission. During remission, symptoms subside and medication might be paused under medical supervision. However, many people eventually experience a recurrence. If you have concerns about potential complications, you may also want to read about Can Graves’ disease kill you and how long can you live with graves’ disease for a broader understanding of long-term outlook.
Continue reading to explore the available treatment options for hyperthyroidism and what they mean for long-term thyroid health.
Fast facts about hyperthyroidism

- Hyperthyroidism is a condition in which the thyroid gland produces an excessive amount of thyroid hormone.
- Thyroid hormone plays a crucial role in many vital body functions, including regulating metabolism and heart rate.
- Although anyone can develop hyperthyroidism, it is most commonly diagnosed in women between the ages of 20–40 years.
- In the United States, about 1 out of every 100 people ages 12 years and older have hyperthyroidism.
How is hyperthyroidism treated?
There are three main treatment approaches for hyperthyroidism. The most appropriate option depends on the underlying cause — such as Graves’ disease, thyroid nodules, or toxic adenoma — the intensity of your symptoms, your age, overall health, and how your body responds to therapy.
- Medication: Drugs known as antithyroid medications reduce the thyroid gland’s ability to produce excess hormones. These medications may take several months before noticeable improvement occurs. Dosage adjustments are often necessary to stabilize thyroid hormone levels and prevent complications such as hypothyroidism. Regular blood tests are essential during this period to monitor progress and ensure safe treatment.
- Radioactive iodine treatment: This therapy involves taking radioactive iodine in capsule or liquid form. Because the thyroid naturally absorbs iodine, the radioactive iodine specifically targets thyroid cells. Once absorbed, it gradually destroys overactive thyroid tissue without significantly affecting other parts of the body. Over time, this typically leads to reduced hormone production. Many individuals who undergo this treatment will eventually require lifelong thyroid hormone replacement.
- Surgery: Surgical removal of part or all of the thyroid gland (thyroidectomy) may be recommended in certain cases, such as when a large goiter causes swallowing or breathing difficulties, when nodules are suspicious, or when other treatments are not suitable. After radioactive iodine treatment or complete thyroid removal, lifelong replacement thyroid hormones are necessary to maintain normal metabolic function.

Each of these treatments has benefits and potential risks. A healthcare professional will consider your specific diagnosis, including whether you have Graves’ disease, before recommending a personalized plan.
Can hyperthyroidism go back to normal on its own?
In rare instances, hyperthyroidism may resolve without long-term intervention. One example is postpartum thyroiditis, a temporary inflammation of the thyroid that can develop after childbirth. This condition affects a small percentage of individuals shortly after delivery.
Postpartum thyroiditis often begins with hyperthyroidism and may transition into hypothyroidism before resolving completely. Approximately 80% of people recover within 12–18 months. However, it can recur in subsequent pregnancies, and some individuals may eventually develop permanent thyroid dysfunction.
Outside of temporary inflammatory conditions, spontaneous resolution of hyperthyroidism is uncommon. This is especially true for autoimmune causes like Graves’ disease, which typically require medical treatment and ongoing monitoring.
What causes hyperthyroidism?
Hyperthyroidism can develop from several underlying conditions that cause the thyroid gland to become overactive and release too much thyroid hormone into the bloodstream.
Common causes include:
- Graves’ disease: Graves’ disease is an autoimmune disorder and the leading cause of hyperthyroidism. In this condition, the immune system mistakenly attacks the thyroid, stimulating it to produce excess hormones. Graves’ disease often has a genetic component and may run in families.
- Thyroid nodules: Thyroid nodules are lumps that form within thyroid tissue. Some nodules can independently produce thyroid hormone, leading to hormone imbalance. They are more frequently diagnosed in individuals over age 60.
- Toxic adenoma: A toxic adenoma is a noncancerous growth that generates excess thyroid hormones. While most adenomas are harmless and do not significantly affect hormone levels, a small percentage — called toxic adenomas — can trigger hyperthyroidism.
- Swelling of your thyroid: Inflammation or swelling of the thyroid gland can increase hormone release. Although hyperthyroidism often causes thyroid enlargement, inflammation itself can also initiate overproduction.
- Thyroid cancer: In rare cases, a tumor in the thyroid may lead to increased hormone production.
- Certain medications: Some medications may stimulate the thyroid or contain thyroid hormone, resulting in excess levels.
Identifying the precise cause is essential, as it influences both treatment decisions and long-term prognosis.
What are the symptoms of hyperthyroidism?
Regardless of the cause, hyperthyroidism typically presents with similar symptoms due to the accelerated metabolic state it creates in the body. These symptoms may range from mild to severe.
- a racing heart
- trouble sleeping
- heat sensitivity
- sweating
- unintentional weight loss
- fatigue
- weakness
- trembling or shaking
- mood changes
- anxiety
- irritability
- visible swelling of the thyroid gland in your neck, known as a goiter
Because many of these symptoms overlap with other health conditions — including anxiety disorders and heart conditions — it’s important to seek medical evaluation if they persist. Early diagnosis can help prevent complications such as heart rhythm abnormalities or bone thinning.
A healthcare professional may diagnose hyperthyroidism through a physical examination and blood tests that measure thyroid hormone levels and thyroid-stimulating hormone (TSH). Determining the root cause, whether it’s Graves’ disease or another condition, is the first step toward selecting the most effective treatment strategy.
If you’ve experienced symptoms for more than a week or two, or if you notice new or worsening changes, scheduling a medical appointment is strongly recommended. Prompt care can improve outcomes and reduce the risk of long-term effects.
Takeaway
Most forms of hyperthyroidism are chronic conditions that require ongoing management. Although treatment can successfully control hormone levels and relieve symptoms, a permanent cure is uncommon in many cases.
For example, surgically removing the thyroid completely eliminates excess hormone production, but lifelong thyroid hormone replacement therapy becomes necessary afterward.
In autoimmune hyperthyroidism such as Graves’ disease, medication may lead to remission for some individuals. Still, relapse is common, which is why continuous monitoring is essential. While treatments are highly effective at controlling symptoms and protecting long-term health, maintaining regular follow-up care remains a key part of living well with hyperthyroidism.


















Leave a Reply
You must be logged in to post a comment.