Blood in your stool without pain is often linked to a hemorrhoid, but there are additional possible causes, such as anal fissures or polyps. A healthcare professional can determine the exact reason and recommend appropriate treatment options, including medicated ointments for hemorrhoids or fissures.
It’s completely understandable to feel alarmed if you notice blood during a bowel movement. Many people immediately associate it with a serious medical problem.
However, not every situation requires urgent care—especially if you’re not experiencing pain. In many cases, rectal bleeding without discomfort may be temporary and related to a manageable condition like hemorrhoids.
That said, persistent or recurring bleeding should never be ignored. Understanding When to worry about blood in stool can help you recognize when it’s time to seek medical advice and rule out more serious gastrointestinal conditions.
Below, you’ll learn about the potential causes of painless rectal bleeding, which symptoms signal the need for medical evaluation, and practical steps to manage the condition safely.
What causes rectal bleeding without pain?
Hemorrhoids are one of the leading causes of rectal bleeding without discomfort. Still, blood in your stool may stem from several other conditions that can sometimes be treated at home or with over-the-counter remedies.
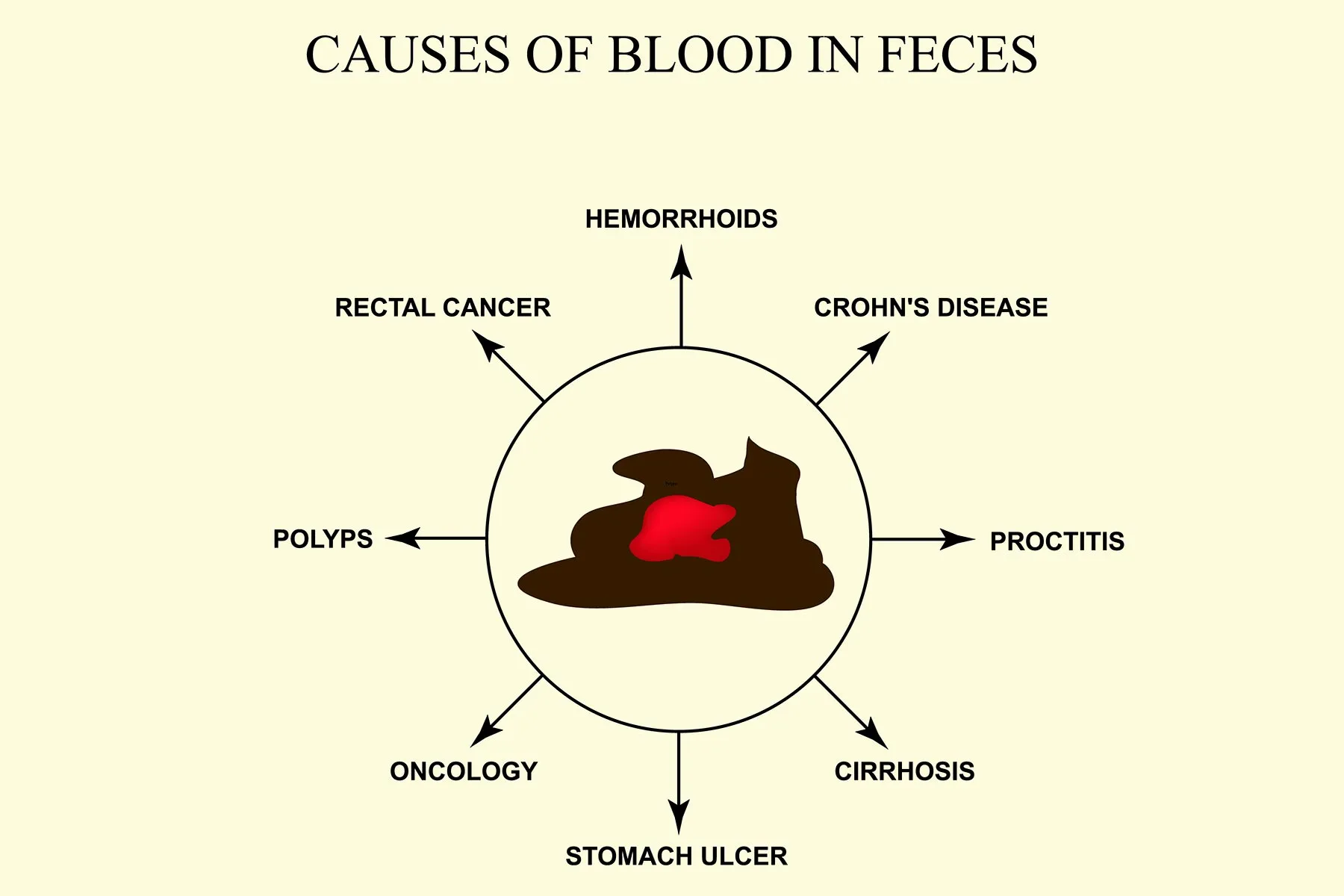
Hemorrhoids
Hemorrhoids develop when veins in the rectum or anus become swollen and enlarged. While they don’t always cause pain, the engorged veins can bleed, allowing blood to pass into the rectum and appear in the stool.
External hemorrhoids form beneath the skin around the anus and may bleed externally. Internal hemorrhoids, on the other hand, occur inside the rectum and may bleed without obvious external signs.
Additional symptoms that may suggest an internal hemorrhoid is bleeding include:
- itching around the anus
- a burning feeling
- mild discomfort during bowel movements
- swelling near the anal opening
In many cases, hemorrhoids resolve on their own with conservative measures such as dietary changes and topical treatments.
Learn more about treatment options for bleeding hemorrhoids.
Anal fissures
Anal fissures occur when the delicate skin surrounding the anus tears and begins to bleed. Although they can be painful, especially during bowel movements, some fissures may bleed with minimal discomfort.
Common signs of anal fissures include:
- a visible crack or tear in the anal skin
- swelling or small skin tags near the anus
- blood on toilet paper after wiping
- itching or a burning sensation
Most fissures heal without extensive treatment unless the open area becomes infected. Increasing fiber intake and staying well hydrated can support healing by preventing constipation.
Learn about foods that may help with anal fissures.
Polyps
Polyps are small growths that form on the lining of the colon and often resemble mushrooms.
These growths typically do not cause pain. However, they may bleed intermittently, leading to visible blood in the stool.
While many polyps are benign tissue overgrowths, some can progress to cancer if left untreated. For this reason, routine screening is essential—particularly for adults over 45 or those with a family history of colorectal cancer.
Colorectal cancer
Certain polyps, known as adenomas, can develop into colorectal cancer. Cancer cells rely on blood vessels within the intestines to grow and spread. Blood from cancerous tumors may appear in the stool, sometimes without pain in early stages.
Colorectal cancer is often highly treatable when detected early. Physicians may remove cancerous polyps or surgically excise affected portions of the bowel to prevent the disease from spreading to other organs.
This highlights why recognizing When to worry about blood in stool is so important—especially if bleeding is persistent, unexplained, or accompanied by changes in bowel habits.
Inflammatory bowel disease
Inflammatory bowel disease (IBD) includes conditions characterized by chronic inflammation in the digestive tract.
The most common forms are ulcerative colitis, which affects the large intestine, and Crohn’s disease, which can involve any part of the digestive tract, including the stomach and small or large intestine.
IBD does not always cause continuous pain. However, inflammation can lead to narrowing or blockage, which may injure intestinal tissue as stool passes through. This irritation can result in blood mixing with the stool.
Some individuals experience mild symptoms that can be managed with dietary adjustments and medication. Others may develop more severe complications, including abdominal pain, urgency, or difficulty passing stool.
Color is a clue
The appearance and shade of blood in your stool can offer valuable insight into its source:

- Bright red: This usually indicates bleeding in the lower digestive tract, such as the rectum or anus. Hemorrhoids are a common cause.
- Maroon or dark red: This may suggest bleeding higher in the colon or possibly the small intestine.
- Black or tar-like: Dark, sticky stool may point to bleeding in the stomach, such as from a stomach ulcer.
Understanding these differences can help you determine when to monitor symptoms and when to seek medical evaluation.
When should I be worried about blood in my stool?
If you’re unsure When to worry about blood in stool, pay attention to accompanying symptoms. Seek immediate medical care if you experience severe abdominal pain, particularly if it begins suddenly after noticing rectal bleeding.
Other warning signs that require prompt medical attention include:
- dizziness or lightheadedness
- a constant sensation of rectal pressure
- chills
- fever
- nausea or vomiting without a clear cause
- constipation that doesn’t improve
- persistent diarrhea
- rapid heart rate
- difficulty urinating
- loss of consciousness
In some cases, people may confuse rectal bleeding with other sources of blood, such as urinary symptoms. If you are unsure about the origin, reviewing related concerns like Blood in pants male nhs or Blood in urine male with pain may help you better describe your symptoms to a healthcare provider.
To determine the underlying cause, a doctor or gastroenterologist (GI doctor) may recommend:
- a physical examination to check for visible causes
- a blood test to detect markers of underlying conditions
- a stool sample analyzed in a laboratory to identify bacteria or abnormalities
- gastroscopy to evaluate possible stomach bleeding
- sigmoidoscopy to inspect the rectum and lower colon
- colonoscopy to examine the colon for internal hemorrhoids, polyps, or other abnormalities
These diagnostic tools are essential when bleeding is ongoing, unexplained, or accompanied by systemic symptoms.
How can I manage rectal bleeding?
If you notice blood during bowel movements but have no significant pain, consider these supportive measures:
- Stand up and move around at least once every hour to relieve pressure from prolonged sitting.
- Apply topical creams or ointments formulated for hemorrhoids or fissures.
- Avoid straining during bowel movements, as this can worsen hemorrhoids and tears.
- Drink sufficient water daily to support healthy digestion and soften stool.
- Increase dietary fiber intake through fruits, vegetables, whole grains, or supplements to promote regularity.
Maintaining a balanced diet, engaging in regular physical activity, and managing constipation are key preventive strategies. If conservative measures fail, speak with a healthcare professional about procedural or surgical options for severe hemorrhoids, cancer, or IBD.
Takeaway
Passing blood without pain does not always signal a medical emergency. In many instances, the cause is minor and treatable.
Still, knowing When to worry about blood in stool is crucial. If bleeding continues over time or is accompanied by pain, fever, diarrhea, weakness, or other concerning symptoms, consult a healthcare professional promptly. Early diagnosis allows for timely treatment and reduces the risk of complications.




















Leave a Reply
You must be logged in to post a comment.