Xerosis cutis is the clinical term for excessively dry skin, more intense than ordinary dryness. The word derives from the Greek “xero,” meaning dry.
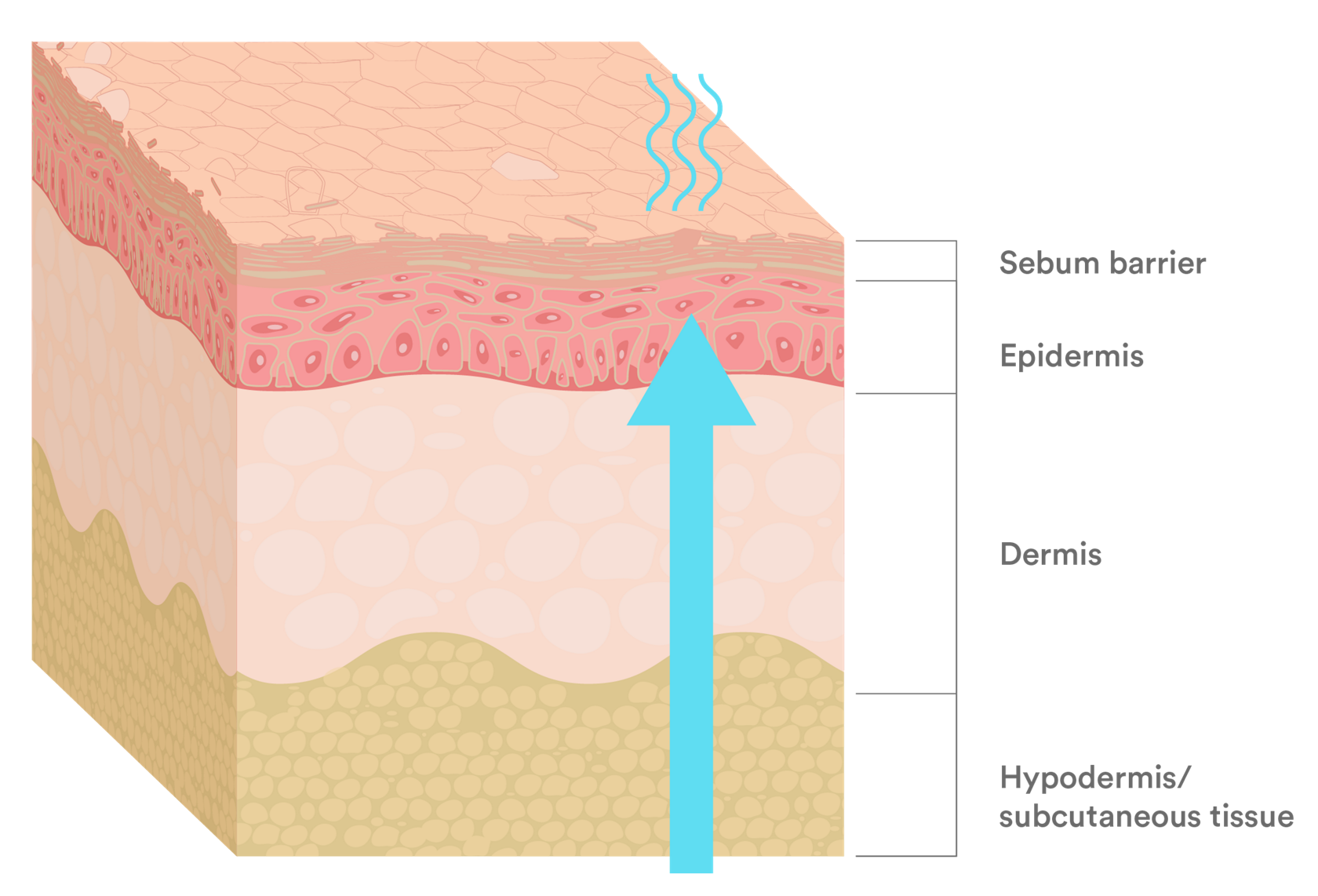
Dry skin affects many people, particularly older adults. Often it’s a mild, temporary issue, but it can cause irritation and discomfort. Skin requires moisture to remain supple. With aging, the skin’s ability to retain moisture diminishes, causing it to become rough and dehydrated as it loses water and natural oils.
Dry skin tends to be more prevalent in cold winter seasons. Small adjustments to daily habits — such as taking shorter, lukewarm showers and applying moisturizers — can help reduce the likelihood of developing xerosis cutis.
What leads to xerosis cutis?
Xerosis results from a reduction in the skin’s surface oils. Environmental influences are common triggers. The following behaviors or circumstances can contribute to dry skin:
- excessive cleansing or scrubbing of the skin
- using very hot water for baths or showers
- bathing too often
- rubbing the skin vigorously with a towel
- living in low-humidity environments
- residing in regions with cold, dry winters
- using central heating at home or work
- not drinking enough fluids (dehydration)
- prolonged exposure to the sun
Who is more likely to get xerosis cutis?
Xerosis cutis worsens during winter months when the air is drier and humidity is low.
Older adults face a higher risk than younger people. Aging reduces activity of sweat and sebaceous glands, largely because of hormonal changes, making xerosis cutis a frequent issue for those 65 and older. Diabetes also raises the risk, so older individuals with diabetes are particularly prone to xerosis.

What symptoms occur with xerosis cutis?
Common signs of xerosis cutis include:
- dry, itchy, scaly skin, often on the arms and legs
- a tight feeling in the skin, particularly after bathing
- white, flaky patches
- red or pink irritated areas
- fine cracks developing in the skin
How is xerosis cutis managed?
Home care
Treatment focuses on easing symptoms. Managing dry skin at home typically involves regular application of moisturizers. Generally, oil-based creams are better at locking in moisture than water-based ones.
Choose creams that include lactic acid, urea, or both. If the itching is significant, a topical steroid like 1 percent hydrocortisone cream may help. Ask a pharmacist to suggest an appropriate moisturizing product for your needs.
Be aware that items labeled “lotion” usually contain less oil. Water-based lotions can sometimes aggravate xerosis cutis rather than soothe it. Additional helpful measures include:
- avoiding forced or excessive heat
- taking lukewarm showers or baths
- staying well-hydrated by drinking plenty of water
Many people try natural remedies such as essential oils or aloe, but evidence for their benefit is limited. One study even suggests avoiding aloe vera for xerosis, as it may increase skin sensitivity. Emollients like coconut oil can help seal in moisture and reduce itching. If you have issues with hand dryness, consider guidance on dry hands as part of your care routine. For people with mixed skin types, see tips for dry oily skin.
When should I consult a doctor?
See a dermatologist if:
- your skin is draining or oozing
- large areas are peeling
- you notice a ring-shaped rash
- there’s no improvement within a few weeks
- your condition worsens despite treatment
These signs could indicate a fungal or bacterial infection, an allergic reaction, or another dermatologic condition. Intense scratching of dry areas can also lead to infection.
In younger individuals, dry skin may indicate atopic dermatitis (eczema), a condition marked by severely dry, itchy skin. Eczema can produce blisters and thick, scaly patches. A dermatologist can determine if you or your child has eczema, which requires a different treatment approach than xerosis cutis.
Xerosis cutis may also be associated with other disorders, such as:
- ringworm
- thyroid problems
- psoriasis
Do not disregard persistent xerosis cutis. If irritation or itching continues after self-care, seek medical evaluation.
How can xerosis cutis be prevented?
Dry skin isn’t always avoidable, especially with aging. Still, you can reduce the chance or severity of xerosis cutis by adjusting daily habits:
- avoid very hot bath or shower water; use lukewarm instead
- keep baths and showers shorter
- limit prolonged water exposure and avoid long soaks in hot tubs or pools
- use mild, fragrance-free cleansers without dyes or alcohol
- pat skin dry with a towel instead of rubbing
- drink plenty of fluids to stay hydrated
- minimize soap use on dry patches and choose soaps with added oils
- try not to scratch affected areas
- apply oil-based moisturizers frequently, especially in winter and right after bathing
- use sunscreen when outdoors
- use a humidifier to raise indoor air moisture levels




















Leave a Reply
You must be logged in to post a comment.