Sore gums can develop for a variety of reasons, including gum disease, brushing too forcefully, or hormonal fluctuations. In some situations, they may also be associated with COVID-19 infection, although this is not considered a common symptom.
If you’re noticing Red spots roof of mouth COVID concerns along with gum discomfort, it’s understandable to feel worried. However, sore gums by themselves — without other symptoms — are unlikely to point to COVID-19. When gum tenderness appears together with more typical signs like fever, cough, fatigue, or loss of taste and smell, it becomes more plausible that COVID-19 or another systemic illness may be involved.
In this guide, we’ll explain how to determine whether your gum pain could be linked to COVID-19 or if another oral or medical condition is the more likely cause. We’ll also explore related symptoms such as red spots, oral ulcers, and dry mouth that sometimes accompany viral infections.
How to tell if it’s COVID-19
Sore gums may occur in people with COVID-19, but they are not among the hallmark symptoms. If gum pain is your only complaint, the likelihood that COVID-19 is the cause remains low.
That said, COVID-19 can indirectly increase the risk of gum discomfort. For example, the infection has been associated with dry mouth, which may create an environment that allows gum disease to develop more easily.
In addition to gum tenderness, COVID-19 has been linked to painful ulcers affecting the gums, lips, tongue, and other areas inside the mouth. Some people reporting Red spots roof of mouth COVID symptoms describe accompanying irritation or inflammation in nearby tissues. If you’re unsure what these changes look like, reviewing Red spots on roof of mouth pictures may help you better understand common presentations.
Mouth ulcers
Ulcers of the mouth may appear in individuals with COVID-19, as well as with other viral diseases such as dengue fever, Ebola, and measles. These lesions can form on the gums, lips, palate, tongue, or throat.
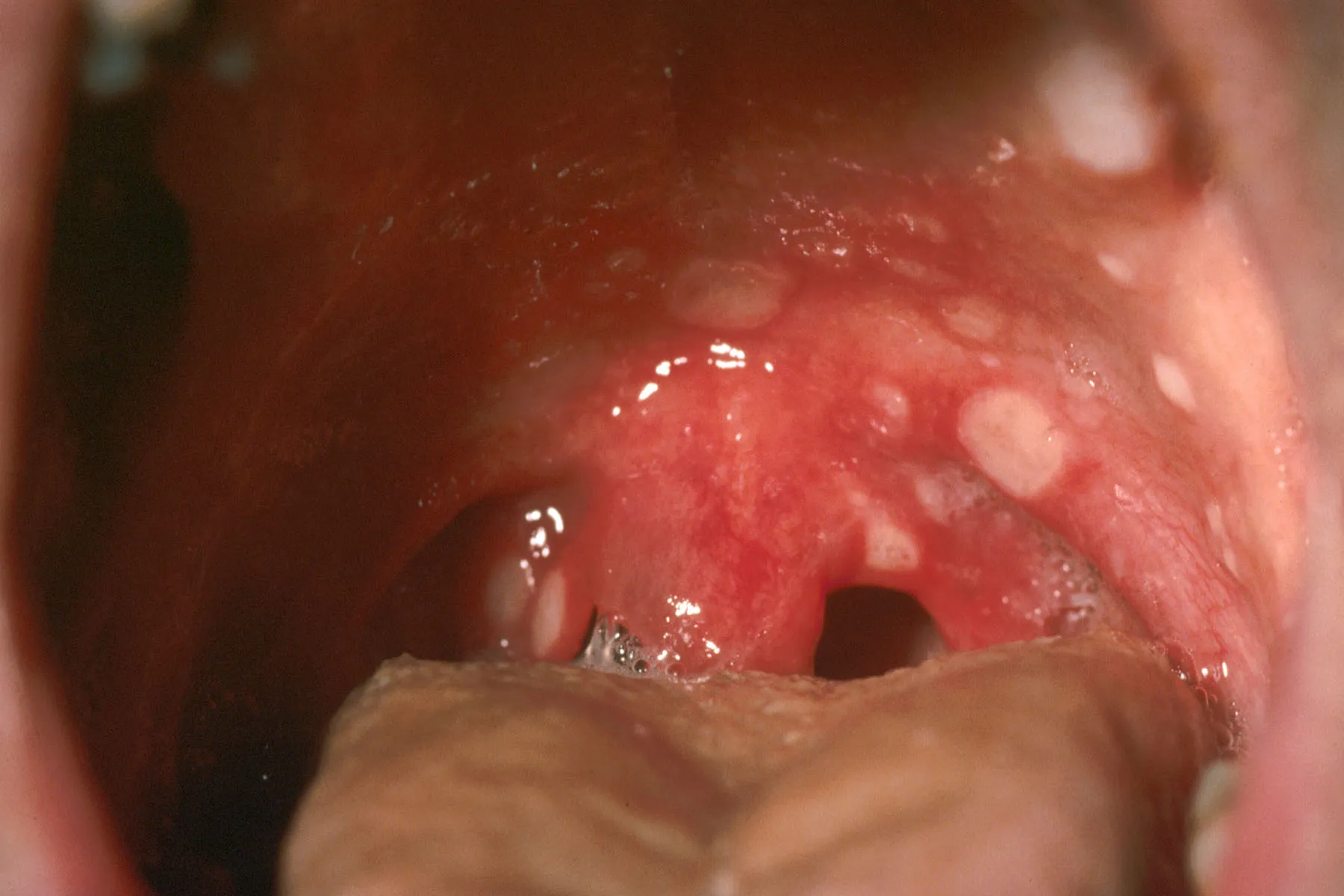
A February 2021 case series reported that mouth ulcers occurring during a COVID-19 infection were linked with loss of taste and smell. The ulcers were more frequently observed in older adults and in those experiencing severe infections.
In many cases, ulcers developed early in the course of illness, after taste changes but before broader symptoms such as fever, cough, and fatigue. With appropriate treatment, most ulcers healed within 2 weeks. If you notice ulcers alongside red spots or other oral lesions, reviewing Viral infection in mouth pictures may provide helpful visual context.
Dry mouth may contribute to gum pain
A 2021 review of studies identified dry mouth as the most frequently reported oral symptom in people with COVID-19. Among 170 individuals with oral symptoms, 75 experienced dry mouth.
Reduced saliva production can significantly affect oral health. Saliva helps wash away bacteria and food particles, so when the mouth is dry, plaque buildup may increase. Over time, this can raise the risk of gum disease — and gum pain is a common symptom of gum disease. While COVID-19 may not directly inflame the gums, it can indirectly contribute to discomfort by triggering dry mouth.
Research has also connected gum disease with COVID-19 because they share several risk factors, including:
- diabetes
- obesity
- aging
- hypertension
Interestingly, dry mouth can appear before more recognizable COVID-19 symptoms. In a case study, a 56-year-old female developed dry mouth and loss of taste 2 days prior to the onset of fever, loss of appetite, and fatigue.
What other conditions can cause sore gums?
Although some people are concerned about Red spots roof of mouth COVID or gum pain being linked to coronavirus, many other conditions commonly cause gum tenderness. Below are several possibilities.
Gum disease
Gum disease usually develops due to a bacterial infection that forms when plaque and food debris accumulate along the gumline. Typical signs and symptoms include:
- gum swelling
- gum bleeding
- gums peeling away from your teeth
- bad breath
- loose teeth
Without proper treatment, gum disease can progress and lead to more serious oral health complications.
Hormonal changes
Hormonal fluctuations can make gums more sensitive and prone to inflammation. The hormones estrogen and progesterone increase blood flow to gum tissue, which may heighten tenderness.
Changes in these hormone levels may occur during:
- pregnancy
- puberty
- menstruation
- menopause
Malnutrition
Deficiencies in vitamin C, protein, or vitamin B can result in swollen, painful gums and additional oral symptoms. Addressing the root cause through dietary adjustments may resolve the issue in some cases. However, limited food access or medical conditions such as Crohn’s disease can also contribute to nutritional deficiencies.
Oral thrush
Oral thrush is a yeast infection that produces yellowish-white patches on the cheeks, gums, lips, or tongue.
Other symptoms may include:
- bleeding
- sore or burning mouth
- cotton-like sensation
- a bad taste in your mouth
- loss of taste
Oral herpes
Herpes simplex is a viral infection that spreads through close contact and can cause cold sores in or around the mouth.
During outbreaks, painful sores may develop on the lips, gums, or palate. These lesions can be tender to the touch and may resemble other viral-related oral changes.
Dental abscess
A dental abscess is a collection of pus resulting from a bacterial infection. It may form in the gum tissue or at the root of a tooth.
The main symptom is intense, throbbing pain. Additional symptoms can include swollen gums, bad breath, and swelling of the face. Prompt dental treatment is typically necessary.
Are there other causes of sore gums?
Several everyday factors may also trigger gum discomfort, such as:
- scratches of your gums
- brushing your teeth too vigorously
- flossing aggressively
- allergy to dental products such as toothpaste or mouthwash
- food allergy
- burns
- improperly fitting dentures
- gum damage from tobacco use
- canker sores
When should I see a doctor?
If your gum pain lasts longer than a few days or is accompanied by signs of gum disease — such as bleeding or gums pulling away from your teeth — it’s wise to schedule an appointment with a dentist or healthcare professional.
If you develop classic COVID-19 symptoms or suspect recent exposure, isolate yourself from others and follow public health guidance. Seek urgent medical care if severe symptoms arise.
What treatments are available?
Appropriate treatment for sore gums depends on the underlying cause.
| Cause | Treatment |
| COVID-19 | – Get plenty of rest and stay hydrated – Seek immediate medical attention if you have severe symptoms |
| Thrush | – Oral antifungal medication – Thrush will often go away without treatment in healthy adults |
| Oral herpes | – Over-the-counter pain relievers, such as acetaminophen (Tylenol) – Stay hydrated – Topical anesthetics |
| Dental abscess | – Root canal – Removing the affected tooth – Incision and drainage – Antibiotics if the infection spreads |
| Malnutrition | – Treatment to target the root cause of malnutrition – Dietary changes |
| Hormonal changes | – Treatment of the underlying condition causing hormonal changes – Treatment to manage symptoms |
| Canker sores/cold sores | – Often, treatment is not needed – Steroid mouth rinses – Oral medications |
How can I prevent sore gums and COVID-19?
Practicing strong oral hygiene habits can reduce your risk of gum disease–related pain. The American Dental Association advises:
- brushing your teeth twice a day with a fluoride toothpaste
- cleaning between your teeth once per day
- minimizing sugar and maintaining a nutrient-rich diet
- visiting your dentist regularly for prevention and treatment of oral disease
Supporting your immune system through adequate sleep, balanced nutrition, hydration, and stress management can also lower your risk of infections that may contribute to oral symptoms, including Red spots roof of mouth COVID concerns.
To decrease your risk of COVID-19, follow preventive recommendations from the Centers for Disease Control and Prevention (CDC):
- get a COVID-19 vaccine when available
- avoid crowded areas and poorly ventilated spaces
- wash your hands often with soap and water or use hand sanitizer
- avoid contact with people who have a recent COVID-19 infection
- stay six feet away from people not in your household
- wear a mask that covers your nose and mouth
The takeaway
COVID-19 may be linked to sore gums and other oral changes, including ulcers and dry mouth.
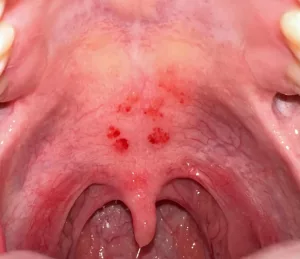
However, gum pain has many possible causes. It’s unlikely to indicate COVID-19 unless it appears alongside more common symptoms such as fever, fatigue, cough, or loss of taste and smell. If you’re concerned about persistent symptoms or notice unusual changes like red spots on the palate, consult a healthcare professional for personalized evaluation and care.

















Leave a Reply
You must be logged in to post a comment.