Key takeaways
- Life expectancy with congestive heart failure depends on factors such as age, stage at diagnosis, heart function, and overall health.
- Treatment options such as SGLT2 inhibitors, other medications, surgery, and lifestyle modifications can help control congestive heart failure.
- Lifestyle strategies including lowering sodium and alcohol intake, staying physically active, monitoring weight, and quitting smoking may help slow the progression of congestive heart failure.
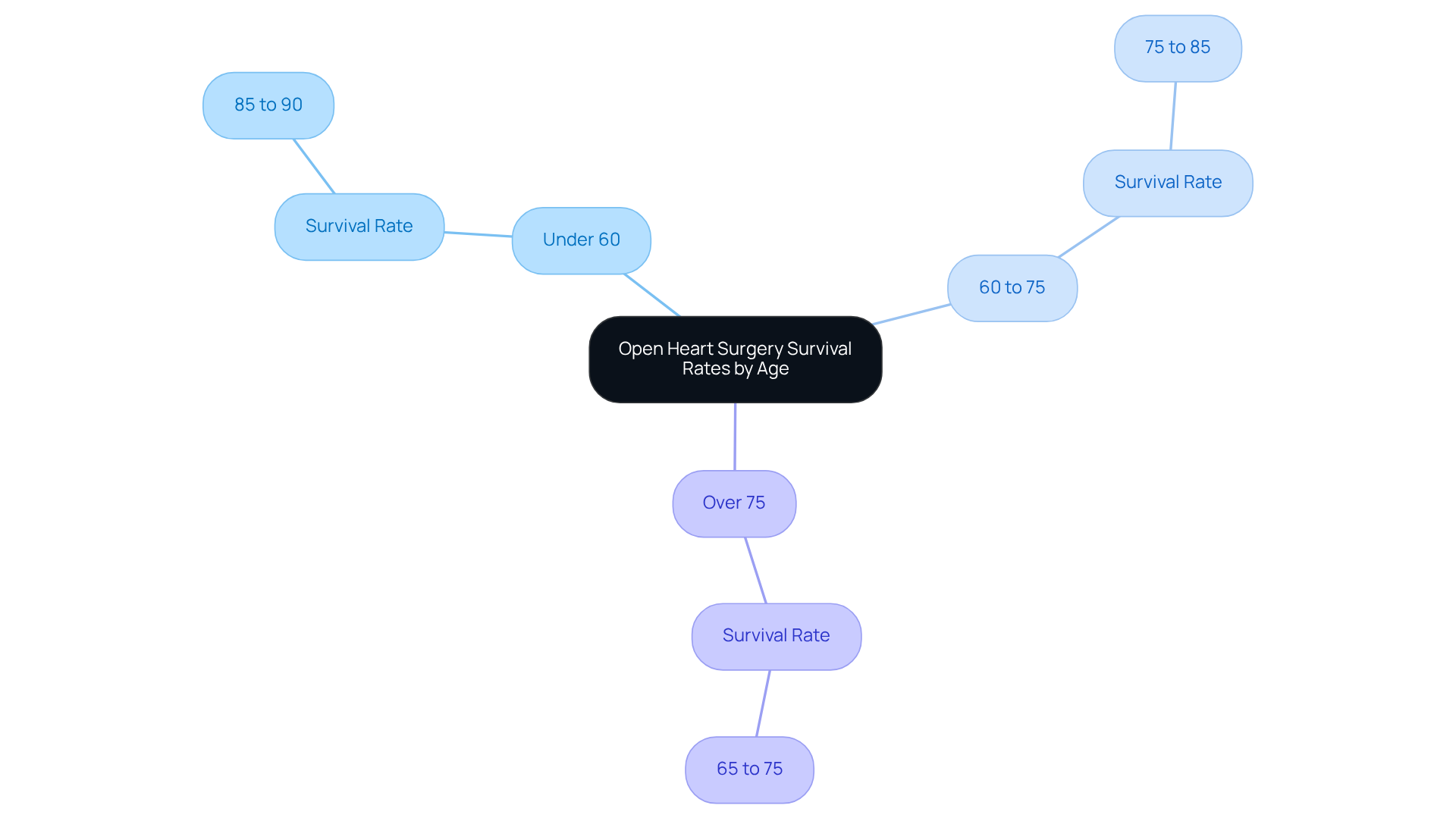
When discussing long-term heart health, many people search for information about the Open heart surgery survival rate by age 55 to better understand what the future may hold. While surgical outcomes are important, it’s equally essential to understand how chronic conditions like congestive heart failure (CHF) influence overall prognosis and quality of life.
Congestive heart failure (CHF) develops when the heart muscle can no longer pump blood as efficiently as it should. As a result, the body may not receive adequate oxygen-rich blood, potentially leading to a range of additional health complications.
Often simply called heart failure, CHF is a chronic and progressive condition. Over time, symptoms can worsen if not properly managed. However, with early detection and appropriate treatment, many individuals can stabilize or even improve their condition. Below, we explore how prognosis and survival rates may differ depending on individual factors.
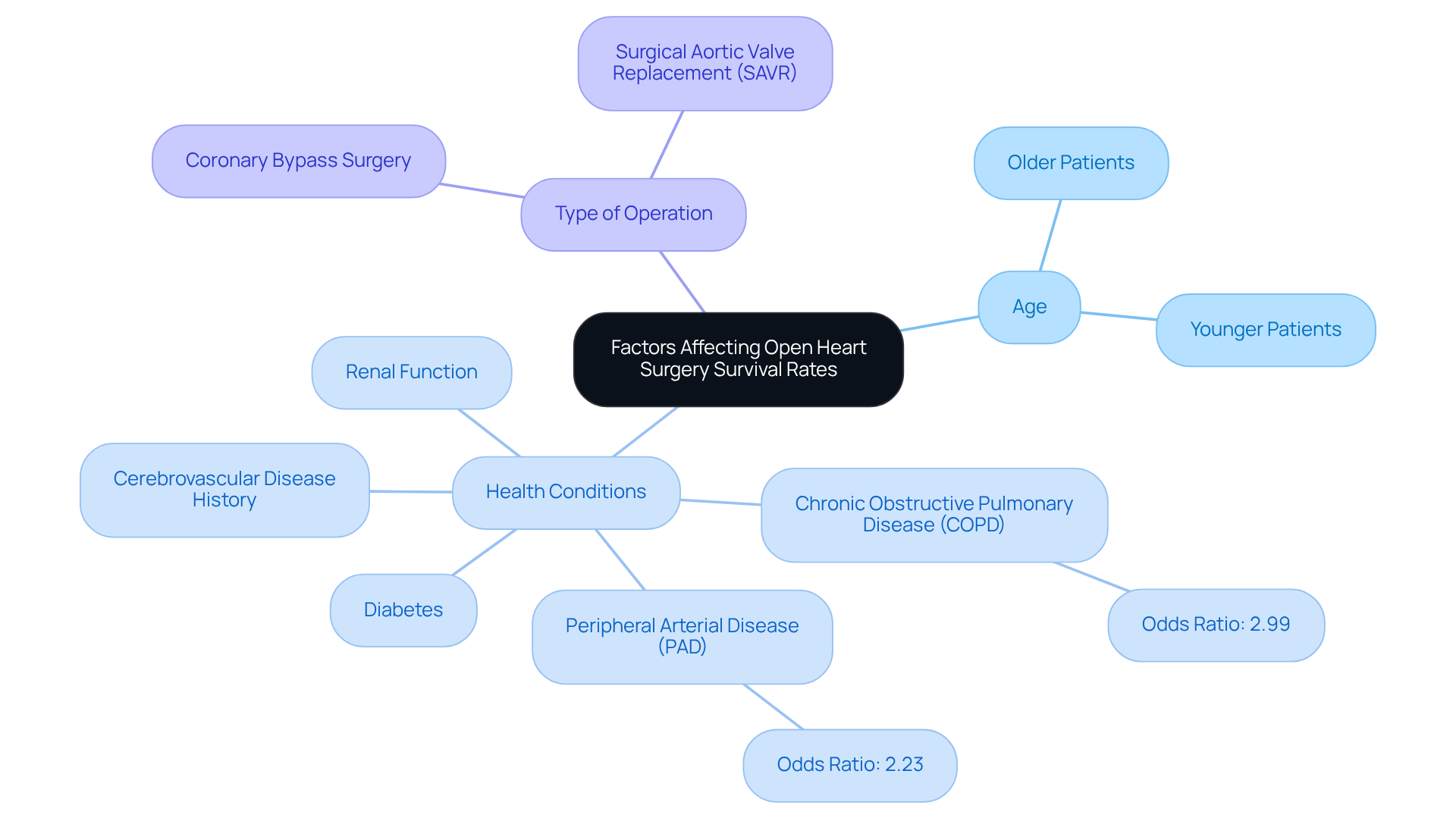
Factors affecting prognosis
There are many factors that influence the outlook for CHF. Your healthcare provider is the best source of guidance for your specific case.
Key elements that commonly affect CHF prognosis include:
- age at diagnosis
- the underlying cause of CHF
- alcohol consumption
- gender
- stage of the disease at diagnosis
- your heart’s ejection fraction
- how often you’re hospitalized for CHF symptoms
- presence of other medical conditions
- how effectively you respond to treatment
- how closely you adhere to your treatment plan
According to older research published in 2008, African American individuals may face a higher risk of CHF compared with white and Hispanic individuals when hypertension and diabetes are present, along with social and economic influences. Addressing these underlying conditions is critical for improving long-term outcomes.
Prognosis at each stage
CHF outlook varies widely from one person to another because each case involves unique contributing factors. In general, individuals diagnosed in earlier stages who receive prompt and consistent treatment tend to have a more favorable prognosis than those diagnosed at later stages.
Some people whose CHF is identified early and treated effectively may achieve a life expectancy close to average, particularly when they follow medical advice and adopt heart-healthy habits.
Prognosis by ejection fraction
Ejection fraction (EF) measures the percentage of blood the heart pumps out with each contraction. A healthy heart typically has an EF between 55 percent and 75 percent.
Certain individuals with CHF experience a reduced EF, meaning the heart is pumping less blood than normal. Research consistently shows that people with CHF and reduced EF generally face a more difficult outlook compared with those whose EF remains preserved.
Although survival statistics differ among studies, all studies confirm that EF significantly influences prognosis. Your doctor can best explain how your specific EF measurement may impact your long-term outlook.
Prognosis at different ages
Age plays a meaningful role in survival rates. Broadly speaking, younger individuals diagnosed with CHF often have better outcomes than older adults.
A combined analysis of several smaller studies reported that people under age 65 had a 5-year survival rate of 78.8 percent after a CHF diagnosis. In contrast, individuals over age 75 had an average 5-year survival rate of 49.5 percent.
Older adults with CHF frequently have additional chronic conditions, which can complicate treatment and recovery. Similarly, when evaluating surgical outcomes such as the Open heart surgery survival rate by age or the Open heart surgery survival rate by age 50, age and coexisting health issues significantly influence overall survival statistics. For individuals specifically researching the Open heart surgery survival rate by age 55, outcomes are often shaped by cardiovascular fitness, diabetes status, kidney function, and adherence to postoperative care.
Treatment options for CHF
There are multiple treatment options available for congestive heart failure. The most suitable approach depends on:
- your overall health
- other medical conditions you may have
- your response to medications
- the stage of CHF
Common treatment strategies include:
- Sodium-glucose cotransporter 2 (SGLT2) inhibitors. These may be prescribed if you also have type 2 diabetes to help safeguard kidney and heart function.
- Angiotensin receptor-neprilysin inhibitor (ARNI). This combination of sacubitril and valsartan can help lower high blood pressure.
- Verquovo. This guanylate cyclase stimulator has been shown to reduce the risk of death from heart failure.
- I(f) channel blockers (ivabradine). These medications may ease heart failure symptoms by slowing the heart rate.
- Spironolactone (MRAs). MRAs are sometimes used for hypertension that does not respond to other therapies.
- Beta-blockers and other heart medications. Drugs such as beta-blockers, angiotensin-converting enzyme (ACE) inhibitors, and angiotensin receptor blockers (ARBs) can improve the heart’s pumping efficiency.
- Diuretic medications (water pills).Diuretics like bumetanide, furosemide, and toresemide help the body eliminate excess fluid.
- Nitrates. These medications may relieve chest pain.
- Blood thinners.Blood thinners help lower the risk of blood clot formation.
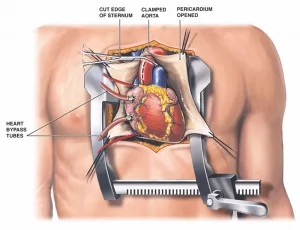
- Coronary bypass surgery. CHF may occur due to blocked arteries. In this procedure, healthy arteries from other areas of the body are used to reroute blood around blocked vessels.
- Implantable cardioverter-defibrillators (ICDs). Implanted in the chest, an ICD monitors heart rhythm and can deliver a shock if a dangerous rhythm occurs.
- Cardiac resynchronization therapy (CRT). A CRT device coordinates the heart’s chambers so they beat more efficiently and may be combined with an ICD.
- A left ventricular assisted device (LVAD).LVADs are mechanical pumps that help the heart pump more effectively and are sometimes used in end stage heart failure.
- A heart transplant. In select cases, heart transplant may be considered. However, older adults may not always be candidates. In such situations, an LVAD may not serve as a permanent alternative.
Living with congestive heart failure
Adopting heart-healthy habits can meaningfully slow CHF progression. Always consult your doctor before changing your diet or beginning a new exercise plan.

Diet
Sodium can increase fluid retention in the body’s tissues. For this reason, a low sodium diet is frequently recommended for people with CHF.
Limiting alcohol and caffeine is also advised, as both can affect the heart muscle and potentially contribute to weakness.
The American Heart Association suggests no more than two cups of coffee per day and limiting alcohol to two drinks daily for men and one drink daily for women.
Exercise
Aerobic activity has been shown to enhance the heart’s overall performance, supporting improved quality of life and possibly extending longevity.
Your healthcare team can design an exercise plan tailored to your abilities and tolerance levels, ensuring safety while maximizing benefits.
Fluid restriction
People with CHF are often encouraged to monitor fluid intake, since excess fluid can worsen symptoms. Those taking diuretics to remove extra fluid may offset the medication’s benefits if fluid intake is too high.
Individuals with advanced CHF are commonly advised to limit total fluid intake to 2 quarts daily.
Weight monitoring
Rapid weight gain can signal fluid buildup. Gaining 2–3 pounds within a few days should prompt a call to your doctor.
Your provider may adjust your diuretic dosage to better control fluid retention before it becomes more serious.
Quit smoking
Smoking places additional strain on the heart by raising heart rate and blood pressure. Many people notice improvement in CHF symptoms after quitting.
Clothing choices
Very tight garments, especially around the legs, may increase the risk of blood clots. Choosing looser-fitting clothing can help reduce this risk.
Avoid becoming excessively hot or cold. Wearing layers that can be added or removed as needed is often helpful.
Take care of your mental health too
Emotional stress can negatively affect heart health. Learning anger management and stress reduction techniques can be beneficial.
Working with a therapist or participating in a support group may help you maintain healthy coping strategies and stay committed to lifestyle adjustments.
Takeaway
The prognosis for CHF varies considerably based on disease stage, age, and other medical conditions. Understanding related cardiovascular risks — including concerns such as the Open heart surgery survival rate by age 55 — can provide helpful context, but individual outcomes depend on many interconnected factors.
Younger individuals often have a more favorable outlook, but lifestyle changes, medications, and surgical interventions can substantially improve outcomes at any age. Collaborate closely with your healthcare team to create a treatment strategy that best supports your long-term heart health.



















Leave a Reply
You must be logged in to post a comment.