Neuropathic pain is often described as shooting, electric, or burning discomfort. For some individuals, the pain is steady, while for others it comes and goes without warning. Tingling sensations, numbness, or partial loss of feeling are also frequently reported symptoms.
If you’ve ever wondered, “Why is my neuropathy worse when I lay down?” you’re not alone. Many people notice their nerve pain intensifies at night or when resting quietly. Changes in body position, reduced distractions, and shifts in circulation can all make nerve-related pain feel more pronounced when you’re trying to relax or sleep.

Neuropathic pain is typically caused by a chronic, progressive nerve disease, but it may also develop after an injury or infection. Unlike typical injury-related pain, it does not always require a clear trigger.
For those living with chronic neuropathic pain, flare-ups can happen at any moment, even without a specific pain-inducing event. Although less common, acute neuropathic pain can occur as well.
In contrast, non-neuropathic pain (nociceptive pain) generally results from an identifiable injury or illness. If you accidentally drop a heavy book on your foot, your nervous system immediately sends pain signals once the impact occurs.
With neuropathic pain, however, the discomfort is not usually initiated by a visible event. Instead, the body sends pain signals to the brain without an obvious cause. Over time, neuropathic pain often becomes more intense or persistent.
About 1 in 3 Americans live with chronic pain. Of those individuals, 1 in 5 experience neuropathic pain.
A 2014 study estimated that up to 10 percent of Americans have some form of neuropathic pain.
Understanding what may be contributing to your symptoms — especially if you’re asking why your neuropathy is worse when lying down at night — can guide you toward more effective treatments and long-term management strategies.
What causes neuropathic pain?
The leading causes of neuropathic pain generally fall into four broad categories: disease, injury, infection, and limb loss.
Disease
Neuropathic pain can be a symptom or complication of various diseases and medical conditions. These include multiple sclerosis, multiple myeloma, and other types of cancer.
Not everyone with these disorders will develop neuropathic pain, but for some, it becomes a significant concern.
According to the Cleveland Clinic, diabetes accounts for 30 percent of neuropathic cases. Long-standing diabetes can interfere with normal nerve function.
Individuals with diabetes often report numbness and reduced sensation, followed by burning, stinging, and painful sensations in their hands, feet, and digits. These symptoms may become more noticeable at night, contributing to the common complaint: why is my neuropathy worse when I lay down?
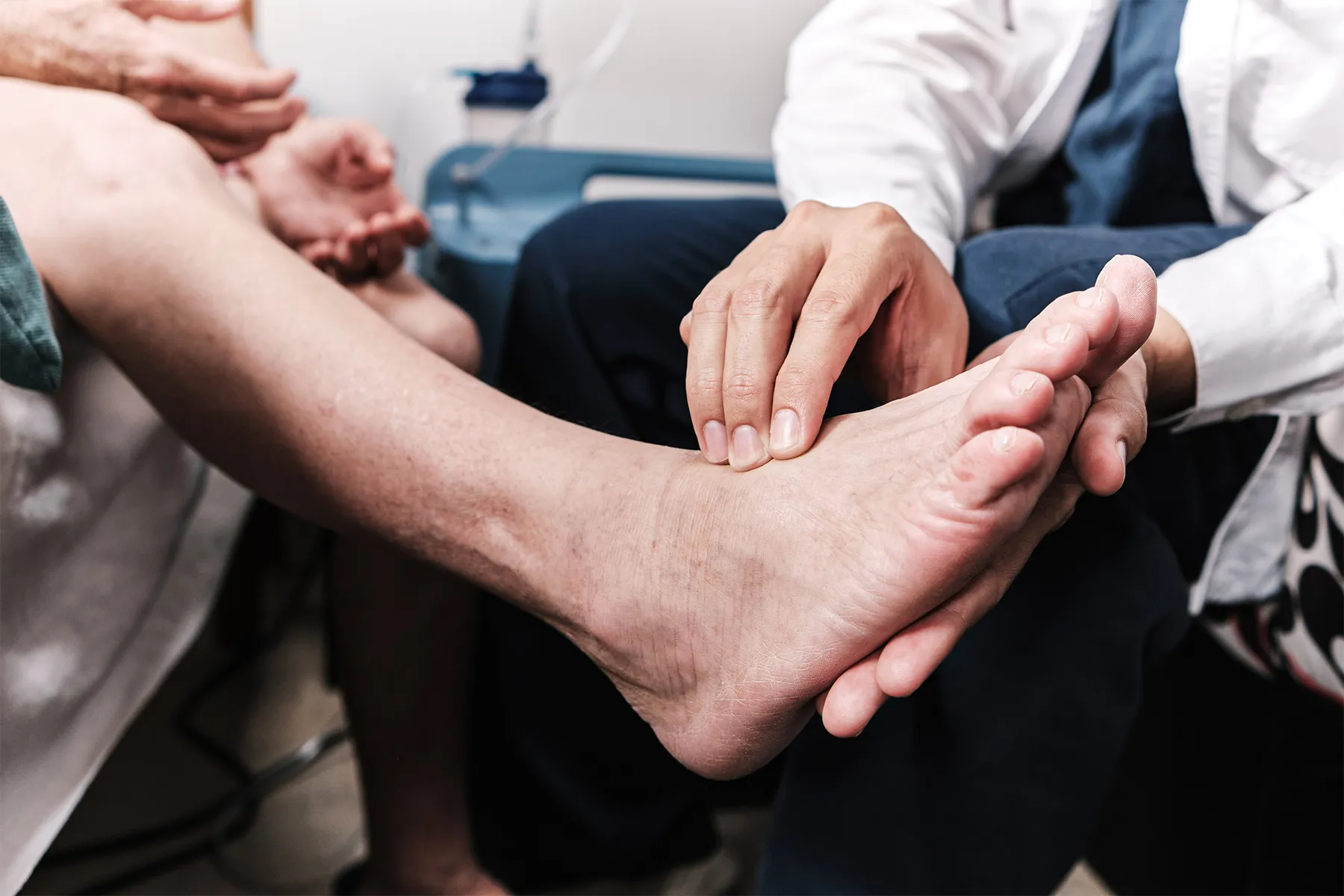
Chronic excessive alcohol use may also lead to numerous complications, including persistent neuropathic pain. Nerve damage related to long-term alcohol exposure can produce lasting and sometimes severe discomfort.
Trigeminal neuralgia is another painful condition characterized by intense neuropathic pain affecting one side of the face. It is among the more frequently diagnosed neuropathic pain disorders and may arise without a clear cause.
Cancer treatments, including chemotherapy and radiation, can also affect the nervous system. These therapies may disrupt nerve signaling and trigger abnormal pain sensations.
Injuries
Damage to tissues, muscles, or joints is a less common source of neuropathic pain. However, injuries involving the back, legs, or hips can result in lasting nerve damage.
Even after the visible injury has healed, the nervous system damage may persist. As a result, ongoing pain can continue for years following the original accident.
Spinal injuries or trauma affecting the vertebral column can also lead to neuropathic pain. Herniated discs and spinal cord compression may injure nearby nerve fibers, causing chronic nerve-related symptoms.
Infection
Infections are an uncommon but recognized cause of neuropathic pain.
Shingles, caused by reactivation of the chicken pox virus, can produce weeks of neuropathic pain along the affected nerve pathway. Postherpetic neuralgia is a rare but serious complication of shingles that involves ongoing neuropathic pain.
Syphilis may also result in unexplained burning or stinging pain. Additionally, individuals with HIV can experience similar unexplained nerve discomfort.
Limb loss
A rare type of neuropathic pain known as phantom limb syndrome can develop after an arm or leg has been amputated. Even though the limb is no longer present, the brain continues to perceive pain signals as if it were.
This phenomenon occurs because nerves near the amputation site misfire and transmit incorrect signals to the brain.
Phantom pain may also affect fingers, toes, the penis, ears, and other body parts.
Other causes
Additional causes of neuropathic pain include:
- vitamin B deficiency
- carpal tunnel syndrome
- thyroid problems
- facial nerve problems
- arthritis in the spine
What are the symptoms?
Symptoms of neuropathic pain can differ from person to person, but several features are commonly reported:
- shooting, burning, or stabbing pain
- tingling and numbness, or a “pins and needles” sensation
- spontaneous pain, or pain that appears without a clear trigger
- evoked pain, or discomfort triggered by typically non-painful activities — such as light touch, exposure to cold, or brushing your hair
- a persistent sensation of discomfort or abnormal feeling
- difficulty sleeping or fully resting
- emotional distress related to chronic pain, sleep disruption, and challenges communicating your experience
Many individuals find that symptoms intensify in the evening. Reduced external distractions, natural circadian rhythm changes, and lying still can heighten awareness of nerve pain. This often leads people to search for solutions to nighttime nerve discomfort and explore strategies like How to sleep with peripheral neuropathy or How to sleep through nerve pain to improve rest.

How’s it treated?
The primary objective in treating neuropathic pain is to identify and address the underlying disease or condition responsible for the symptoms, whenever possible.
Another essential goal is pain relief, preserving daily functioning despite discomfort, and enhancing overall quality of life.
The most commonly used treatments for neuropathic pain include:
Over-the-counter pain medication
Nonsteroidal anti-inflammatory drugs (NSAIDs), such as Aleve and Motrin, are sometimes tried for neuropathic pain.
However, many individuals discover that these medications provide limited benefit because they do not specifically target nerve-related pain pathways.
Prescription medication
Opioid pain medications are generally less effective for neuropathic pain than for other pain types. In addition, physicians may be cautious about prescribing them due to the risk of dependence.
Topical pain relievers may also be recommended. These include lidocaine patches, capsaicin patches, and prescription-strength creams or ointments.
Antidepressant drugs
Antidepressant medications have demonstrated significant effectiveness in relieving symptoms of neuropathic pain.
Two primary categories are commonly prescribed:
- tricyclic antidepressants
- serotonin-norepinephrine reuptake inhibitors
These medications may help manage both nerve pain and symptoms of depression or anxiety that often accompany chronic pain conditions.
Anticonvulsants
Anti-seizure medications and anticonvulsants are frequently used to treat neuropathic pain. Gabapentinoids are among the most commonly prescribed options.
Although the exact mechanism is not fully understood, researchers believe these medications modify pain signaling and reduce abnormal nerve transmissions.
Nerve blocks
Your doctor may administer steroids, local anesthetics, or other pain-relieving medications directly into nerves believed to be responsible for abnormal pain signals. These nerve blocks are temporary and typically need to be repeated for sustained relief.
Implantable device
This surgical approach involves implanting a device within the body. Some devices are positioned in the brain, while others are placed along the spine.
Once implanted, these devices deliver electrical impulses to the brain, spinal cord, or specific nerves. These impulses can interrupt irregular nerve signals and reduce symptoms.
Implantable devices are generally reserved for individuals who have not achieved sufficient relief from other treatments.
Lifestyle treatments
Physical therapy, relaxation techniques, and massage therapy are often incorporated into neuropathic pain management plans. These approaches can help reduce muscle tension and improve mobility.
A healthcare provider may also teach coping strategies for managing chronic nerve pain. For example, some people experience worsening symptoms after prolonged sitting, which can make desk-based work challenging.
A physical therapist or occupational therapist can provide guidance on posture, stretching, standing routines, and movement techniques to help minimize pain flare-ups.
How can this pain be managed?
If an underlying cause of neuropathic pain can be identified, addressing it may lessen or even eliminate symptoms.
For instance, diabetes is a frequent cause of neuropathic pain. Effective diabetes management — including a balanced diet and consistent physical activity — may reduce or prevent worsening nerve pain.
Maintaining stable blood sugar levels can also help prevent progression of numbness and discomfort.
Multimodal therapy
A comprehensive, multipronged strategy is often the most effective approach.
Combining medications, physical therapy, psychological support, and, in some cases, surgical interventions or implantable devices may produce optimal outcomes.
Additionally, improving sleep hygiene, managing stress, and addressing nighttime discomfort can be especially helpful for those who notice their neuropathy worsens when lying down.
Outlook
Without appropriate treatment and symptom management, neuropathic pain can significantly affect daily life.
Over time, it may contribute to serious complications such as depression, sleep disturbances, anxiety, and reduced physical function.
Ongoing research continues to expand understanding of how neuropathic pain develops and how best to treat it. These advances are leading to improved therapeutic options.
Identifying the right combination of treatments may require patience. By working closely with your doctor, you can develop a personalized plan aimed at relieving symptoms and improving your overall quality of life.




















Leave a Reply
You must be logged in to post a comment.